What Percentage of Prostate Biopsies Detect Cancer?

Prostate cancer is rated second on the list of the most common cancers that develop in male patients.
When your doctor suspects prostate cancer, they will often suggest a prostate biopsy.
Not all of these biopsies come back positive, so you might have questions about when a biopsy is not needed.
Keep reading to learn what percentage of prostate biopsies are cancer.
What Percentage Of Prostate Biopsies Are Cancer?
Although prostate biopsies are a valuable tool for diagnosing cancer, it’s important to understand that a significant portion of these biopsies result in negative findings.
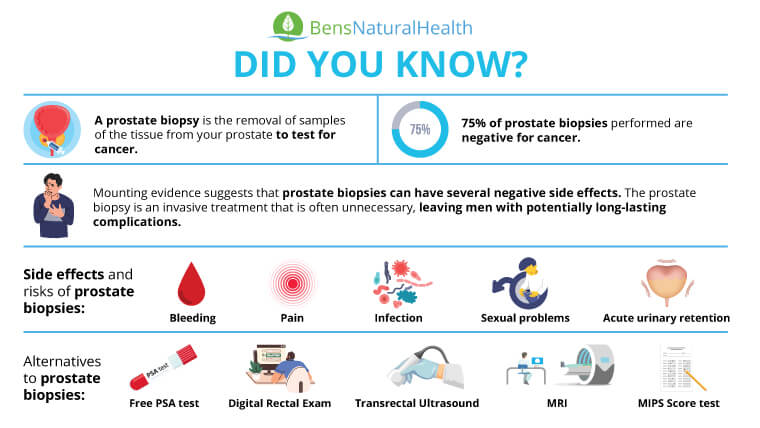
Approximately 75% of prostate biopsies come back without any evidence of cancer.
With this said, it’s also not the most accurate diagnostic tool, as negative cancers are also often reported.
Why Are Doctors Recommending Prostate Biopsies If They Aren’t Always Needed?
A biopsy is frequently recommended when signs of prostate cancer are present. However, a study suggests that the use of a prostate MRI may be more effective in detecting cancer within the gland compared to biopsies.
With alternative screening options that are less invasive, the question remains – why do doctors sometimes advise a prostate biopsy when there are other diagnostic tools that can be used?
The reasons for this choice may vary, but in some cases, it could be attributed to physicians adhering to traditional protocols established during their training.
Due to the massive size of the pharmaceutical industry, doctors may also prefer to use a biopsy in the diagnosis of prostate cancer in order to present pharmaceutical solutions as a treatment for your condition.
Statistics show that by the year 2028, the prostate cancer treatment industry will reach a global worth of $25.43 billion. Between 2022 and 2028, the market is also expected to grow at an annual rate of 5.6%.
Major players in the market all focus on the use of pharmaceuticals to treat prostate cancer and related complications in male patients.
Hence, some doctors may opt for a biopsy due to the influence and involvement of the pharmaceutical industry in contemporary medicine.
When you undergo a prostate biopsy, it’s important to know the risks so you can make an informed decision.
Pain in your prostate area can linger on for a while, as your doctor will usually take multiple samples during the biopsy procedure. Apart from pain, there are complications that you also need to recognize.
There is a risk of prolonged bleeding after you undergo a prostate biopsy. Additionally, some people experience pain that gradually gets worse.
Urination difficulties and fever are also complications that you could experience after the procedure.
A Word From Ben’s Natural Health
Many doctors solely follow the data that they have in medical books and based on their time at University, which often leads to a prostate biopsy even in cases where it’s not required.
Understanding the risks of a prostate biopsy can help you understand when it might be time to get a second opinion and why alternative solutions are sometimes better.
In our view, a significantly safer and less invasive alternative to a prostate biopsy is our Advanced Prostate Cancer Risk Assessment (APCRA). This consists of non-invasive blood tests and specialized color Doppler scans.
The diversity and advanced nature of certain blood tests make them a highly viable alternative to a prostate biopsy, particularly if you prefer non-invasive diagnostic methods and treatments.
To learn more or book our Advanced Prostate Cancer Risk Assessment, please call our customer service team on +1-888-868-3554 who will be happy to assist you and offer any further information.
Explore More

This article is for informational purposes only and does not serve as medical advice. The details provided here are not a replacement for, and should never be depended upon as, professional medical advice. Always consult your physician regarding the potential risks and benefits of any treatment.
Our Medical Review Process
At Ben’s Natural Health, we are committed to maintaining the highest standards of accuracy, transparency, and scientific integrity. Every piece of content is carefully developed by medical professionals and undergoes a thorough review every 12 to 24 months. This ensures that our information remains current, reliable, and rooted in credible, evidence-based research. We reference only peer-reviewed studies from reputable medical journals, providing full citations and direct links to enhance trust and confidence.
Our Editorial Guidelines
For over 25 years, Ben’s Natural Health has been a trusted source of scientifically backed, reliable health information. Our editorial guidelines uphold the highest quality and integrity for every article we publish. Each piece is written by qualified experts and undergoes independent quality checks. We prioritize transparency by clearly displaying contributor credentials and biographies at the beginning of every article.
Medical Disclaimer
The content on this blog is for informational purposes only and should not be considered a substitute for professional medical advice, diagnosis, or treatment. While our articles are authored and reviewed by licensed medical professionals, they may not address your specific health concerns. Always consult a qualified healthcare provider before making any medical decisions.
Article Sources
- World Cancer Research Fund International. Prostate cancer statistics.
- Drost FH, Osses DF, Nieboer D, Steyerberg EW, Bangma CH, Roobol MJ, Schoots IG. Is prostate MRI, with or without MRI-targeted biopsy, better than systematic biopsy for detecting prostate cancer in men? Cochrane. 2019.
- MarketWatch. Prostate Cancer Treatment Market | Industry Outlook Analysis Report 2023-2028.
- American Cancer Society. Key Statistics for Prostate Cancer.
Article Update History
Updated on 19 October, 2023 (Current Version)
Created on 12 May, 2023
Explore More

New Guidelines On Prostate Cancer Screening For Black Men
The goal of prostate cancer screening is to detect it early and find it before it spreads and causes symptoms. Late detection can lead ...

