Coronary Artery Disease: Risk Factors, Symptoms, and Treatment
Article Summary
- Coronary artery disease (CAD) is the most common type of heart disease.
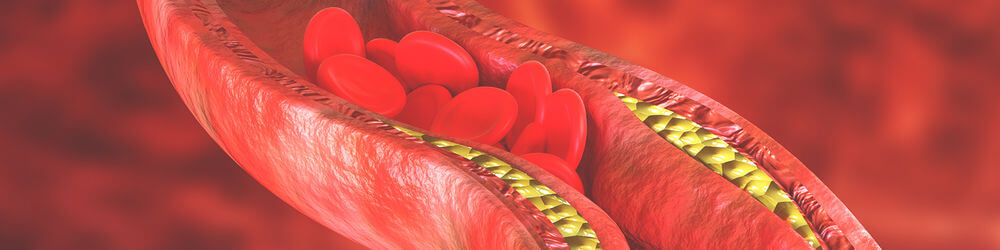
- It occurs when the arteries that supply blood to the heart become hardened and narrowed.
- Risk factors such as family history and age are outside of your control.
- However, several risk factors are preventable, including high cholesterol, high blood pressure, obesity, smoking, and lack of physical activity.
Heart disease is the number one cause of death worldwide, according to the World Health Organization.
In the United States alone, heart disease accounted for almost 650,000 deaths in 2017.
Coronary artery disease (CAD) is the most common type of heart disease. It occurs when the arteries that supply blood to the heart become hardened and narrowed.
This is due to the buildup of cholesterol and other material, called plaque, on their inner walls. In this article, we will explore the details of what it is, why it occurs, and what you can do to decrease your risk of developing it.
What is Coronary Artery Disease?
The heart is the primary pump of the body working to supply blood throughout your system. For the heart itself to stay functioning properly, it contains large blood vessels known as coronary arteries that supply it with nutrients and oxygen.
These coronary arteries can become damaged when plaque is allowed to build up inside the vessels. When the plaque build-up is significant enough to cause a reduction in blood flow, the damage becomes known as coronary artery disease.
Plaque is mostly cellular debris composed of fats, cholesterol (especially from low-density lipoprotein or LDL), minerals, dead cells, and other substances. Plaque build-up can take decades to develop in a process known as atherosclerosis. Atherosclerosis is the progressive accumulation of plaque.
Plaque also is thought to lead to inflammation, which draws inflammatory materials that further contribute to plaque build-up.
Note that significant amounts of inflammation can be tested using a c-reactive protein test. The plaque filled artery narrows and hardened in response, which leads to high blood pressure.
When this process causes issues, it is also known as atherosclerotic cardiovascular disease.
When the heart is unable to get enough oxygen due to these blockages, the heart muscle itself can begin to die, causing symptoms such as severe chest pain and shortness of breath. At this point, a heart attack is occurring.
Outside of heart attacks, coronary artery disease can also lead to dangerous alterations in heart rhythms and heart failure.
To prevent this from occurring, doctors may decide to place a stent during a percutaneous coronary intervention procedure to open up the plaque filled blood vessels or prescribe medications such as alpha-blockers.
Of course, preventing plaque build-up from occurring in the first place is the best treatment strategy. Read on to discover the risk factors of CAD.
[bensnaturalhealthIinlineLeadGen id =”1″ event=”15 Food Blood Sugar eBook Download” image=”https://blog.bensnaturalhealth.com/wp-content/uploads/2021/04/Ipad-15-Foods.png” title=”Get Your FREE Diabetes Diet Plan” content=”##15 foods to naturally lower blood sugar levels ##3 day sample meal plan ##Designed exclusively by our nutritionist”]
Risk Factors for CAD
It is impossible to know for sure if coronary artery disease is in your future. Still, medical professionals can make educated guesses based on a variety of risk factors.
Risk factors generally involve either genetics, lifestyle, or pre-existing conditions and are outlined below.
- Age. Heart disease risk starts to increase significantly after the age of 40. This is a significant age to connect with a primary care provider for a risk assessment.
- Genetics. Researchers are working to understand how genes influence CAD risk. There are several genes involved in the development of CAD, but there is no guarantee that any of these genes will cause the condition; instead, they would increase risk. It is useful to know your family history, as this helps inform health care providers about your level of risk.
- Abnormal cholesterol. Cholesterol is broken down into low-density lipoprotein (LDL) and high-density lipoprotein (HDL). LDL is often considered the “bad” cholesterol because it is associated with plaque build-up and inflammation. HDL is known as the “good” cholesterol because it has the opposite effect, helping to reduce plaque build-up. Having an abnormally high LDL is a major risk factor for developing CAD.
- Smoking status. Tobacco directly harms blood vessels, leads to inflammation, and promotes plaque build-up. Not only are people who smoke at high risk for CAD, but they also tend to die more often from the condition as well.
- High blood pressure. If you have hypertension or high blood pressure, your blood vessels will work harder to pump blood throughout your body, and you are at an increased risk for blood clots. Similar to plaque, blood clots can also stop the flow of blood and contribute to CAD. Healthy blood pressure is under 130/80 mmHg.
- Diabetes Mellitus. Those with diabetes are twice as likely to die from cardiovascular disease than the general population, although this will highly depend on the degree of diabetes control. Over time, high blood sugars will affect the proper flow of blood and lead to toxic byproducts.
- Peripheral artery disease. Peripheral artery disease is a similar condition to CAD, except that it occurs in other arteries of the body, such as the legs and feet. People with pre-existing peripheral artery disease are at greater risk of developing CAD.
- Obesity. Having extra body fat, especially around the abdomen, places extra strain on your heart and blood vessels. Also, fat tissue itself is inflammatory. Obesity is defined by a BMI greater than 30; however, measuring waist circumference may be a more accurate marker. A waist circumference higher than 40” (102cm) or men and 35” (88 cm) for females indicates an increased risk for CAD.
- Poor diet. Eating an unbalanced diet full of foods high in saturated fats, trans fats, added sugars, and low in fruits and vegetables is likely to lead to elevated cholesterol and other metabolic issues. Diet choices represent a major area of CAD prevention that is within your control.
- Lack of physical activity. Experts believe exercise is one of the best medicines for your health, and heart disease is no exception. There is a dose-response effect on exercise, which means that the more you exercise, the more your CAD risk is reduced. This also means that even small amounts of exercise and sitting less can offer significant benefits.
The American College of Cardiology and the American Heart Association developed a calculator using some of these factors to determine your 10-year risk of cardiovascular disease. Health care providers use this calculator to decide on various treatments.
Signs and Symptoms of CAD
Recognizing the signs of coronary artery disease can be the difference between life and death during acute episodes.
The most common symptom of CAD is chest pain, known as angina. Angina has varying degrees of severity.
It can be mild and happen during times of physical exertion, after meals, or during times of stress. It can also be more severe, which is known as unstable angina.
Unstable angina can occur at any time and can be described as a sharp, intense burning pain in the chest that lasts for an extended period.
While in general, angina should not be ignored, unstable angina is a medical emergency that should be treated immediately.
Other symptoms of CAD include fatigue, weakness, and shortness of breath. Recall that in CAD, the heart is unable to get enough blood flow, which can zap the body of needed energy.
How to reduce your risk of CAD
To recap, lifestyle changes that are helpful to reduce the risk of heart disease, including the following:
- At least 150 minutes of physical activity per week. Include resistance or strength exercises at least twice weekly.
- Choose healthier types of fats, including plant oils, nuts, seeds, and fish.
- Avoid trans fats at all costs; look for “partially hydrogenated oil” on an ingredient list.
- Keep added sugar and saturated fats to less than 10% of total calories. You can use a nutrition calculator or food labels to keep track of these items.
- Try to make half of your meals, non-starchy vegetables, and fruits.
- If you have extra weight to lose, aim for losing about one pound per week by reducing your daily calorie intake by about 500 and keeping a food diary.
- Keep alcohol in moderation.
- Do not use tobacco products.
Supplements helpful in CAD
Those looking for an edge in further reducing their risk of heart disease may be interested in dietary supplements.
While there is no substitute for making the proper lifestyle changes and following medical advice, there are certain supplements that can assist in those prone to CAD.
- Fish oil. Fish oil capsules are now widely available and contain valuable sources of omega 3 fatty acids. The active ingredients: EPA and DHA are thought to help reduce the risk of heart disease. These omega-3 fatty acids are also helpful in reducing inflammation. Finally, medical providers often recommend fish oil to help lower triglycerides, a storage form of fat in the blood. Omega-3 fats are also available in other supplement forms, such as flaxseed oil.
- Psyllium. Psyllium is a form of soluble fiber made from a specific plant. It can be taken as a powder or in pill form. Since getting enough fiber through the diet can be difficult for many people, fiber supplements can help. Soluble fiber forms a gel in the digestive tract and has been shown to reduce LDL cholesterol by binding to the cholesterol particles. Other forms of fiber, such as polydextrose, are also available, but the evidence seems to favor psyllium.
- Plant Sterols. One of the benefits of eating a more plant-based diet is to obtain valuable compounds such as plant sterols. Plant sterols can also be taken in supplement form and have been shown to reduce LDL cholesterol levels.
- Red Yeast Rice. Red yeast rice is a naturally occurring form of a statin – a medication that is often used to treat high cholesterol and reduce the risk of heart disease. One thing to consider is that the side effects profile of red yeast rice is similar to standard statin medications. In addition, the FDA has warned that some ingredients in supplemental red yeast rice may be harmful.
- Beetroot. Beetroot, taken as a powder or in juice form, contains the natural chemical, nitric oxide. Nitric oxide expands blood vessels and reduces blood pressure, an essential target in preventing CAD. Some research suggests that supplemental beetroot can significantly lower blood pressure.
- Coenzyme q10. CoQ10 is a substance involved in energy metabolism in the body and exists in higher concentrations in the heart. Thus, it has been proposed that taking supplemental Coq10 can assist in heart muscle function. To date, research remains inconclusive on this, with recent reviews calling into question whether Coq10 is worth considering.
Conclusion
Coronary artery disease is a major killer in developed countries. It develops slowly over many years in the process of plaque build-up, known as atherosclerosis. At worst, CAD can lead to fatal heart attacks or heart failure.
Risk factors such as family history and age are outside of your control. However, several risk factors are preventable, including high cholesterol, high blood pressure, obesity, smoking, and lack of physical activity.
Outside of healthy lifestyle habits and regular medical checkups, certain supplements such as fiber powders and fish oil may offer an added benefit.
Explore More

This article is for informational purposes only and does not serve as medical advice. The details provided here are not a replacement for, and should never be depended upon as, professional medical advice. Always consult your physician regarding the potential risks and benefits of any treatment.
Our Medical Review Process
At Ben’s Natural Health, we are committed to maintaining the highest standards of accuracy, transparency, and scientific integrity. Every piece of content is carefully developed by medical professionals and undergoes a thorough review every 12 to 24 months. This ensures that our information remains current, reliable, and rooted in credible, evidence-based research. We reference only peer-reviewed studies from reputable medical journals, providing full citations and direct links to enhance trust and confidence.
Our Editorial Guidelines
For over 25 years, Ben’s Natural Health has been a trusted source of scientifically backed, reliable health information. Our editorial guidelines uphold the highest quality and integrity for every article we publish. Each piece is written by qualified experts and undergoes independent quality checks. We prioritize transparency by clearly displaying contributor credentials and biographies at the beginning of every article.
Medical Disclaimer
The content on this blog is for informational purposes only and should not be considered a substitute for professional medical advice, diagnosis, or treatment. While our articles are authored and reviewed by licensed medical professionals, they may not address your specific health concerns. Always consult a qualified healthcare provider before making any medical decisions.
Article Sources
- Cholesterol-lowering supplements may be helpful. (2018, November 20). Retrieved from https://www.mayoclinic.org/diseases-conditions/high-blood-cholesterol/in-depth/cholesterol-lowering-supplements/art-20050980.
- Coenzyme Q10. (2019, January 17). Retrieved from https://nccih.nih.gov/health/coq10.
- Red Yeast Rice. (2018, March 19). Retrieved from https://nccih.nih.gov/health/redyeastrice.
- Siscovick, D. S., Barringer, T. A., Fretts, A. M., Wu, J. H. Y., Lichtenstein, A. H., Costello, R. B., … American Heart Association Nutrition Committee of the Council on Lifestyle and Cardiometabolic Health; Council on Epidemiology and Prevention; Council on Cardiovascular Disease in the Young; Council on Cardiovascular and Stroke Nursing; and Council on Clinical Cardiology. (2017, April 11). Omega-3 Polyunsaturated Fatty Acid (Fish Oil) Supplementation and the
- Sweis, R. N., By, Sweis, R. N., Jivan, A., & Last full review/revision April 2019 by Ranya N Sweis. (n.d.). Overview of Coronary Artery Disease (CAD) – Heart and Blood Vessel Disorders. Retrieved from https://www.merckmanuals.com/home/heart-and-blood-vessel-disorders/coronary-artery-disease/overview-of-coronary-artery-disease-cad.
- The top 10 causes of death. (n.d.). Retrieved from https://www.who.int/news-room/fact-sheets/detail/the-top-10-causes-of-death.
- Unstable angina: MedlinePlus Medical Encyclopedia. (n.d.). Retrieved from https://medlineplus.gov/ency/article/000201.htm.
Article Update History
Updated on 5 April, 2026 (Current Version)
Created on 7 January, 2020
Explore More

Is Diabetes Causing Your Yellow Toenails and Foot Fungus?
If you want to know why your toenails are yellow, we discuss possible causes in this article. Yellow toenails can be associated with diabetes ...

