Cancer is one of the significant causes of death in the EU, US, and worldwide
It is a complex and diverse condition that can affect any organ.
The condition occurs when specific body cells start growing abnormally due to gene mutation.
They start growing aggressively, depriving the affected organs of nutrients, resulting in the failure of that organ.
Cancer cells can also migrate to surrounding tissues, and travel to different body parts through the lymphatic system in a process called metastasis, ultimately causing widespread destruction and untimely death.
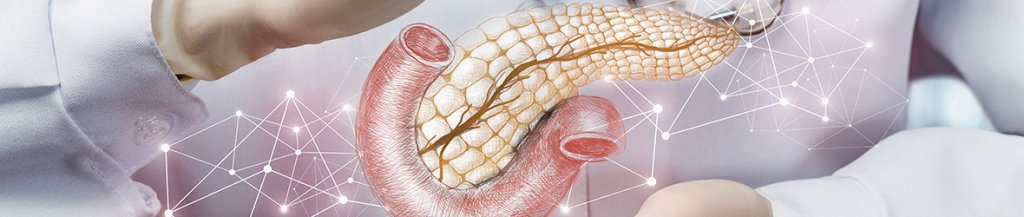
The pancreas is an organ located just behind the stomach. It produces many vital hormones on enzymes.
For example, it plays an important role in glucose metabolism by producing hormones like insulin and glucagon.
It also produces digestive enzymes that help digest carbs, lipids, and proteins – the pancreas produces almost eight cups of pancreatic juice daily.
Pancreatic cancer ranks among the top ten most prevalent cancer types, contributing to approximately 441,000 global deaths annually
Approximately 2% of all cancer cases are attributed to pancreatic cancer, accounting for about 4.6% of all cancer-related deaths.
However, the prevalence of pancreatic cancers is 2-3 times higher in the developed world (EU and the US). (1,2)
The higher prevalence of pancreatic cancer in the EU and US is significantly related to lifestyle choices.
This suggests that many cases of pancreatic cancer are preventable through lifestyle modification and the use of preventive measures like health supplements.
What is pancreatic cancer?
Pancreatic cancer, like many other cancers, often results from genetic mutations in pancreatic cells, leading to uncontrolled cell growth.
The growth of these cells can sometimes be non-cancerous (benign) or cancerous (malignant), potentially leading to pancreatic cancer.
There are two types of pancreatic cancers: exocrine and neuroendocrine tumors. Among all the pancreatic cancers, exocrine makes 93%, and only about 7% are neuroendocrine.
The higher prevalence of exocrine pancreatic cancer is due to the pancreas’s production of digestive juices, which makes the cells responsible for this function more susceptible to cancer.
On the other hand, neuroendocrine cancer occurs due to the mutation of islet cells that produce minute amounts of hormones each day.
Adenocarcinoma is another common name for pancreatic cancer. It most commonly occurs in the pancreatic duct.
Cancers like insulinoma causing uncontrolled insulin production are a type of pancreatic neuroendocrine tumor.

Stages
The two most common ways of defining stages of pancreatic cancer are using a simple approach like stage 0 to 4 or the TNM system.
Doctors often use the TNM (tumor size, nodes, metastasis) system to provide more details. However, for ordinary people, a simple numbering system is better understood. Generally, the lower the number, the less severe the cancer is.
When considering the staging of pancreatic cancer, it is vital to understand that there are also sub-stages like Stage 1A and 1B. However, for the sake of simplicity, this article does not describe sub-stages.
- Stage 0. This is just the beginning of cancer, also called carcinoma in situ. It is a small tumor that affects only the top layers of the pancreatic duct. The deeper layer of the duct is not affected.
- Stage 1. Cancer has grown in size, become deeper, and may be of size up to 4 cm. Nonetheless, it is localized, not spread to lymph nodes or distant sites.
- Stage 2. Cancer may be bigger than 4 cm, or it has spread to no more than 3 nearby lymph node groups.
- Stage 3. Cancer has spread to four or more nearby lymph node groups but has not spread to distant sites.
- Stage 4. Cancer has spread to distant sites like the liver, abdominal cavity, and more.
Signs and symptoms
Pancreatic cancer, like many other cancers, may not initially exhibit noticeable signs. However, as the tumor increases in size or spreads to adjoining areas, it starts causing symptoms.
- Fatigue and unexplained weight loss can be early indicators of cancer.
- As the tumor grows, it may lead to upper abdominal discomfort, which can radiate to the back.
- Jaundice, characterized by yellowing of the skin, is a common symptom associated with pancreatic cancer.
- Dark-colored urine may be an observable symptom.
- Other symptoms can include blood clots, nausea, vomiting, and itchy skin.
- The onset of new or worsening diabetes could be a potential indicator of pancreatic cancer.
Many individuals may experience various gastrointestinal issues as well. The above signs are mainly of exocrine pancreatic cancer. However, pancreatic neuroendocrine cancer may produce different kinds of signs due to hormone overproduction.

What does the pain of pancreatic cancer feel like?
Pain may not be a typical symptom of early-stage pancreatic cancer. However, as cancer progresses, it becomes more pronounced.
Many cases of pancreatic cancer diagnosis involve patients reporting pain as a symptom, with studies indicating it in approximately 70% of cases.
Most people describe pain with pancreatic cancer as dull. However, pain intensity continues to increase. Unlike the intermittent pain associated with gastrointestinal issues, pain in pancreatic cancer tends to be persistent.
As the cancer progresses, the pain may radiate to the back, worsen when lying down, and improve when sitting or leaning forward. It can also be aggravated by food intake.
In some cases, pain may originate in the back, which can be mistaken for back pain. However, pain related to pancreatic cancer typically does not affect the lower back.
Causes
The exact causes of pancreatic cancer remain unclear. However, it is known that specific lifestyle and environmental factors can increase the risk of the disease. Studies have shown a higher prevalence of pancreatic cancer in developed economies.
Risk factors
The risk of pancreatic cancer varies among individuals, and lifetime risk estimates suggest one in sixty-four may develop the disease.
The western lifestyle has been associated with an increased risk of pancreatic cancer, potentially linked to dietary factors and exposure to environmental toxins.
- The risk of pancreatic cancer is much higher in those who smoke tobacco.
- Chronic pancreatitis or inflammation of the pancreas due to alcohol, smoking, and other issues may considerably increase the risk of pancreatic cancer.
- Obesity is recognized as a risk factor for several types of cancer, including those affecting visceral organs.
- It seems that obesity, along with type 2 diabetes, may significantly increase the risk of pancreatic cancer.
- Some people are at greater risk due to exposure to specific chemicals, including some commonly used chemicals and cleaners.
Certain risk factors are non-modifiable, like ethnicity and family history of pancreatic cancer. It appears that blacks are also at a greater risk of cancer.
This risk of cancer is higher in those older than 45 years of age. Similarly, the risk is higher in those living with BRCA genes.
Screening
Doctors do not recommend regular screening for pancreatic cancer. That is why there are no screening guidelines for pancreatic cancer. In addition, no blood test can help in screening.
Nevertheless, it may be a good idea to consider cancer screening for those with family history, those carrying BRCA genes, who developed type 2 diabetes, and are older than 45 years (3).
Genetic tests may help identify the cancer risk. In high-risk people, doctors may consider tests like MRI or endoscopic ultrasound.
It is worth knowing that screening tests for pancreatic cancer are not very sensitive and accurate. Thus, despite the screening, doctors may miss the diagnosis in its early stages. For example, stage 0 cancer may not be visible in MRI or endoscopic ultrasound.
When to see a doctor
Timely intervention may prevent metastatic pancreatic cancer and improve patient outcomes. Thus, it is vital to seek timely help from the healthcare team. The survival rate of any cancer depends on how quickly you seek medical attention.
Thus, do not neglect any upper abdominal pain that has been continuing for some time and affects the back. Especially if the pain is not relieved by rest and is felt during the night when lying on the bed.
Often a person may have other signs like changes in appetite, pain after eating food, and more. In addition, some may unexpectedly develop diabetes. All these are reasons for pancreatic cancer screening.

Diagnosis
It is quite challenging to diagnose pancreatic cancer, especially in its early stages when the tumor is still minute. This means that doctors may struggle to diagnose the condition, and they might even miss the diagnosis.
No blood test can diagnose pancreatic cancer. Some tests might suggest cancer risk. However, these tests do not essentially confirm the diagnosis.
For example, doctors may test blood for high carbohydrate antigen (CA) levels 19-9. This blood test may suggest pancreatic cancer, but not essentially. It may be falsely positive or positive to other kinds of cancer (4).
If doctors think that person might have pancreatic cancer, they may go for MRI or even better endoscopic ultrasound (EUS). In EUS, the ultrasound probe is introduced to the stomach via mouth, which helps provide a clearer picture.
EUS or MRI are helpful but cannot confirm the diagnosis. Therefore, tissue biopsy is the only way to confirm the diagnosis.
However, obtaining a tissue sample of the pancreas for the biopsy is quite challenging. Nonetheless, it is the primary way to confirm the diagnosis.
Complications
Pancreatic cancer is a severe condition and may cause many complications. Some of them are:
Pancreatic insufficiency
It would be present in 80-90% of cases. This means reduced production of digestive enzymes, and thus gastrointestinal issues and severe malabsorption syndrome.
This may cause significant weight loss. It may even affect insulin-producing beta-cells, leading to severe diabetes.
Intestinal obstruction
As cancer grows in size, it may pressurize surrounding organs, thus causing many complications. In addition, the larger tumor may cause severe intestinal obstruction.
Blood clots
The formation of blood clots causing deep vein thrombosis is a common complication of cancer. It may sometimes be the primary sign of the condition. If unmanaged, it may cause pulmonary emboli or even heart attack.
Severe pain
In the later stages of the disease, pain may be severe. It often occurs when the tumor grows and thus pressurizing various nerves, organs, and more.
Treatment
If detected early enough, doctors can cure pancreatic cancer. However, regretfully, it is often identified late and thus has a poor survivability rate.
Researchers have been slow to find pancreatic cancer remedies, and very few clinical trials are ongoing.
Doctors treat it using a traditional approach combining surgery, radiotherapy, and chemotherapy. Generally, doctors would remove the tumor surgically and may even remove the surrounding tissues. After that, they may use radiotherapy and chemotherapy to kill the remaining cancer cells.
Some new treatments under development are immunotherapy and targeted therapy (targets specific genes or proteins). However, these new therapies can help only in some cases.
Additionally, doctors would also provide supportive treatment. This includes pain management, jaundice treatment, reducing intestine blockage, and diabetes control. Cancer patients also require emotional support.
Pancreatic cancer diet (foods to eat and avoid)
The pancreas produces digestive enzymes that help digest carbs, fats, and proteins. Additionally, it also produces insulin.
In cancer, both exocrine and endocrinal functions of the gland are affected, resulting in poor digestion and poor blood glucose control.
Thus, the most important thing to do when living with pancreatic cancer is to eat five or more times a day in small portions. This will help digest food.
At the same time, avoid starchy foods, limit intake of fats, and focus on lean proteins. It means consuming berries, green vegetables, non-starchy vegetables like broccoli, and lean protein like eggs, fish, and tofu.
It is good to consume foods rich in dietary fiber, as they promote gut microbiota and help detoxify. Thus, beans, lentils, quinoa, and oatmeal are good to eat.
Consume healthy fats that are more readily digested, like olive oil, nuts, avocadoes, and so on. Similarly, MCT oil may be good to consume as it bypasses digestive processes and is readily absorbed by the body.
On the other hand, avoid foods like red meat, processed meat, alcohol, sugar and sugary drinks, foods rich in saturated fats, fried items, and so on.

Prevention
Since pancreatic cancer is more prevalent in certain population groups, it has some association with lifestyle choices. Some of the ways to prevent the condition are:
- Avoid smoking tobacco in any form.
- Avoid excessive alcohol drinking.
- Try to maintain a normal body weight.
- Avoid getting diabetes, and manage your blood glucose levels even if diabetes occurs.
- Prevent exposure to toxins by using safety equipment.
Additionally, one may consider discussing dietary measures with a healthcare provider, as well as seeking guidance on natural supplements, if appropriate. It’s essential to consult with professionals who can provide evidence-based recommendations tailored to individual health needs and goals.
Conclusion
Pancreatic cancer is not uncommon. However, people are less aware of its risk than breast, lung, and prostate cancers.
Moreover, it is difficult to diagnose in its early stages, and pancreatic cancer survivorship is low, especially in the case of pancreatic cancer metastasis.
Hence, the better strategy is to focus on its prevention. Moreover, prevention measures like countering obesity and giving up smoking have many other beneficial health effects.
Explore More