Testosterone is a male sex hormone (androgen) that is mainly produced in men’s testicles.
The testicles primarily make testosterone in men. Women’s ovaries also make testosterone, though in much smaller amounts.
Testosterone plays an essential role in men’s health.
The key function of testosterone in males is the development of reproductive organs, including prostate and testes, association with sex drive, and promoting sexual characteristics such as increased muscle mass, bone mass, and the growth of body hair.
This article will provide an overview as to what role testosterone plays in the men and how to increase declining testosterone levels.
Testosterone Levels
Testosterone in the human body appears in two states.
Free state: Not bound to any proteins
Bound to sex hormone-binding globulin (SHBG), which is a protein produced by the liver and transports testosterone in the blood in an inactive form.
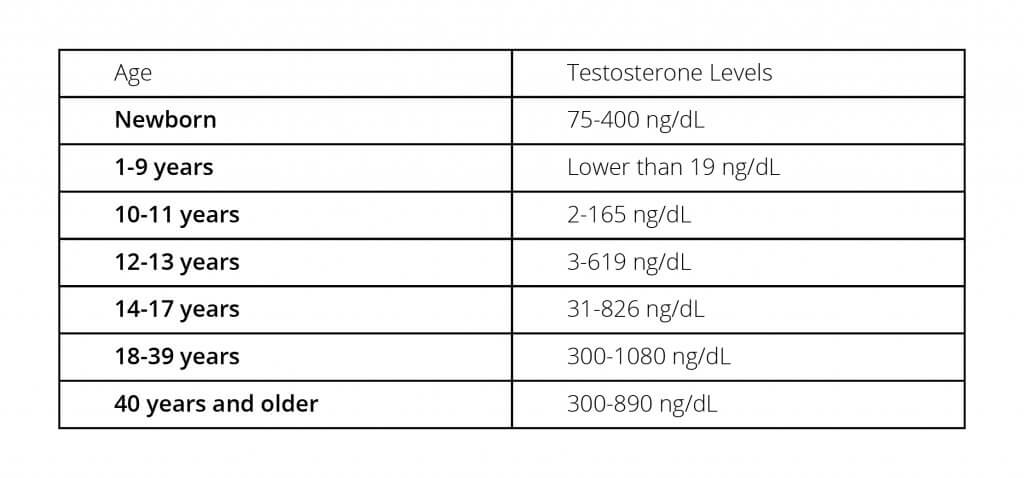
The levels of testosterone vary in males according to age. If the levels are quoted in the units of ng/dl, it is low from 1st till the 9th year of the life measuring less than 19 ng/dl.
From the 10th year of life, its level rises to measure 2-165 ng/dl till the 11th year, 3-619 ng/dl till the 13th year, and 31-826 ng/dl till the 17th year.
The highest level of this hormone will be in men of 18 to 39 years of age and are stated to be 300-1080 ng/dl. After 40 years, the level of testosterone starts falling and usually is 300-890 ng/dl approximately.
What Happens if Testosterone Levels Vary?
Some physicians recommend that monitoring testosterone levels every five years, starting at age 35, is a reasonable strategy to follow. This regular testing of the hormone level calls attention to the importance of it even in older ages of life.
Low testosterone is the more problematic side. Here is how the low levels of the hormone alter various normal body functions in men.
Loss of libido, which means a decrease in sex drive that can interfere with sexual activity.
Erectile dysfunction is the persistent difficulty in achieving and maintaining penis erection sufficient to have sexual intercourse.
The decrease in the number of sperms, which are the male reproductive cells and are ejaculated in the semen during sexual intercourse. This decrease in the number of chief reproductive cells can lead to:
- Male infertility
- Obesity
- Diabetes
- Reduced cognitive function
- Depression
- Irritability
- Less energy
- Low self-esteem
- Reduction of muscle mass, a condition which is medically termed as sarcopenia
- Increased risk of prostate disease, including prostate cancer and benign prostatic hyperplasia.
Causes of Low Testosterone
The levels of testosterone naturally go down with age. Therefore, older men are more likely to be suffering from low testosterone levels.
However, few other conditions have been reported to cause low levels of this hormone. These include:
- Injury to the testes
- Chemotherapy or radiotherapy
- Kidney disease
- Liver disease
- AIDS
- Hypogonadism (a condition characterized by negligible production of sex hormones)
- Use of opioids
- Disorders of thyroid glands.
Some by-birth conditions also result in low testosterone levels. These conditions include:
- Klinefelter syndrome
- Noonan syndrome
- Ambiguous genitalia (when the sex organs develop in ways that are not typical-looking).
The causes and consequences of low testosterone levels indicate well how various functions of the body are interlinked and how malfunction of a single process can affect the activity of others, cause detrimental changes in the body and affect the state of health and well-being.
Testosterone Level Assessment – Diagnosis and Laboratory Tests
To make a diagnosis, your doctor will use other specific signs and symptoms in addition to your testosterone blood level.
On your visit to the physician, your health-related history will be recorded. Your doctor will also perform an examination, i.e., a checkup and look for some of the signs and symptoms which have been mentioned in this article.
A few points which the physician will inquire while recording history include:
- Headache, visual field change (possible symptoms of brain mass such as a pituitary tumor)
- How you developed at puberty
- History of head trauma
- Cranial (head) surgery/brain tumor or cranial irradiation
- Anosmia (loss of ability to smell)
- History of infection in your testicles
- Injury to your testicles
- Mumps after puberty
- Past or present use of anabolic steroids
- Use of opiates
- Use of glucocorticoids (medicines, such as cortisone, used to treat inflammation)
- History of chemotherapy or irradiation
- Family history of diseases linked to low testosterone
- History of stroke or heart attack
- History of unexplained anemia
The physician will then perform a checkup for the following.
- BMI or waist circumference for obesity
- Metabolic syndrome. These are symptoms (seen together) of increased blood pressure, high blood sugar, excess body fat around the waist, and abnormal cholesterol or triglyceride levels
- Hair pattern, amount, and location
- Gynecomastia (enlarged breasts)
- Whether testicles are present and their size
- Prostate size and any abnormalities
To evaluate the level of testosterone in the blood, the following laboratory tests will be prescribed and required.
SHBG- Sex hormone-binding globulin
SHBG is a protein made by your liver, that, along with testosterone, also binds with estrogen and dihydrotestosterone (DHT) and carries these hormones throughout your blood. SHBG controls the amount of testosterone that your body tissues can use.
The level of SHBG in your blood changes because of factors such as sex and age. It can also change because of obesity, liver disease, and hyperthyroidism.
A high SHBG level means that it is likely that less free testosterone is available to your tissues than is indicated by the total testosterone test.
A low SHBG level means that more of the total testosterone is bioavailable and not bound to SHBG.
This information may be important in your overall evaluation when you have signs and symptoms of a condition related to excess or deficient sex hormone production.
Increased SHBG levels may be seen in liver disease, overactive thyroid (hyperthyroidism, eating disorders (anorexia nervosa), estrogen use (hormone replacement therapy and oral contraceptives), decreased sex hormone production in men (hypogonadism) and pregnancy.
Decreases in SHBG are seen with obesity, type 2 diabetes or the metabolic syndrome, polycystic ovary syndrome, underactive thyroid (hypothyroidism), Cushing syndrome, or excessive use of glucocorticoids (such as prednisone or dexamethasone).
The physician will also prescribe total and free testosterone blood levels. This is because SHBG levels are inclined to vary. Both the SHBG and total testosterone tests are needed to confirm testosterone deficiency.
Testosterone levels fluctuate throughout the day and usually are highest in the morning. Therefore, your doctor will probably want to do the blood test in the morning.
Testosterone Therapy – Treating Low Testosterone Levels
“A new multi-year study from the Intermountain Medical Centre Heart Institute in Salt Lake City shows that testosterone therapy helped elderly men with low testosterone levels and pre-existing coronary artery disease reduce their risks of major adverse cardiovascular events — including strokes, heart attacks, and death.
The study showed that patients who received testosterone as part of their follow-up treatment fared much better than patients who didn’t.
Non-testosterone-therapy patients were 80 percent more likely to suffer an adverse event.”
Testosterone therapy is widely used for treatment for men with low testosterone. It can be administered through a range of methods, including:
- Oral medications: Oral medications such as Methyltestosterone are a synthetic form of testosterone, which is similar to the testosterone that’s naturally found in your body. It’s taken in the form of pills, which are only available when prescribed by your doctor.
- Injections: Testosterone injections are a prescription medication that is administered by your doctor. The dose is usually an oil-based solution that contains testosterone.
There are short-acting and long-acting forms of testosterone injection. The short-acting medicine may be given under the skin or in the muscle. The long-acting one is usually given in the muscle. Injections are usually given either weekly, every two weeks, or monthly.
- Oral/buccal (by mouth): The buccal dose comes in a patch that you place above your incisor (canine or “eyetooth”). The medication looks like a tablet, but you should not chew or swallow it. The drug is released over 12 hours. This method has fewer harmful side effects on the liver than if the drug is swallowed, but it may cause headaches or cause irritation where you place it.
- Testosterone patches: A testosterone transdermal patch is a medicated patch that is applied directly onto the skin and stays in place thanks to a sticky backing.
- Intranasal: This form of testosterone comes in a gel. You pump the dose into each nostril, as directed. It is usually taken three times daily.
- Topical creams: Topical creams, such as testosterone gel, can be applied to the skin, entering your system directly. It is effective in improving symptoms associated with low t, such as sexual dysfunction, reduced muscle mass, and low energy levels.
- Pellets: Your doctor will place the testosterone pellets under the skin of your upper hip or buttocks. Your doctor will give a shot of local anesthesia to numb your skin, then make a small cut and place the pellets inside the fatty tissues underneath your skin. This medication dissolves slowly and is released over about 3-6 months, depending on the number of pellets.
The gels, creams, liquids, and patches are topical medicines that most often last for about four days. They absorb better if covered with air or watertight dressing. They are to be applied to the skin, which is dry and without cuts or scratches. The area must then not be washed until it is time for the next dose.
A topical patch is like a band-aid with medicine on it. It is put on and left until the next dose. The medicine on the patch is less likely than liquids, gels, and creams to transfer to others.
Reported side effects of testosterone therapy include:
- Acne
- Disturbed breathing while sleeping
- Breast swelling or tenderness, or swelling in the ankles.
- Doctors also watch out for high red blood cell counts, which could increase the risk of blood clots.
How to Raise Testosterone Levels Naturally
So owing to the above mentioned side effects, one must ask if there are some natural ways to increase testosterone levels.
The following are a few of them, but they are not applicable completely in every case.
Sleep: Testosterone levels in men rise and peak during sleep and therefore, both quality and quantity of sleep are important.
“Studies have shown that men who suffer from sleep apnea also have lower low testosterone than men who do not have sleep apnea.”
Exercise: Studies have shown that testosterone levels rise after exercise, but only briefly. This suggests that exercise doesn’t affect your hormones directly. However, it is still beneficial for men who have levels bordering the average and low ranges of testosterone.
Weight loss: These fat cells produce an enzyme called aromatase, which speeds up the reaction that converts testosterone into estradiol, a form of estrogen. More estrogen in the bloodstream results in less testosterone being produced and so more female physical traits start showing up. So losing muscle and developing those man-boobs is a result of that extra fat you’re storing in your body.
Diet: Certain foods, including oysters, leafy greens, fatty fish, and olive oil, may encourage the body to produce more testosterone. Foods that contain zinc, vitamin D, and magnesium may be vital. Therefore a balanced diet is essential.
Conclusion
Testosterone plays an important role in the development of male characteristics, such as muscle mass, bone density, sexual arousal and facial and body hair.
However, as men age, it is natural for testosterone levels to start to decline. By learning about the essential role of testosterone and understanding the effect low levels can have on men’s health, you are better prepared to take the right steps to prevent this.






