The urethra forms part of the urinary tract. It is an important part that allows urine to be expelled from the human body. The urethra is attached to the bladder neck.
From here, urine flows from the bladder through the urethra during urination. The urethra expels the urine through the opening at the tip of the penis in the male body.
Some conditions can affect the urethra. When this is the case, damage can cause a restriction in the flow of urine.
Urethral stricture disease is one condition that can cause problems with this structure of the urinary system. We take a closer look at what urethral stricture is.
We also consider the symptoms that patients should look out for. The article also focuses on how urethral stricture is diagnosed and looks at the current available treatments.
Get Your FREE PSA Lowering Diet Plan!
- Naturally lower PSA levels
- Reduce nighttime trips to the bathroom
- Enjoy better bladder control and urine flow
What Is Urethral Stricture?
Urethral stricture is an unpleasant condition. It can affect men and women. The condition is generally described as a narrowing of the patient’s urethra1. This is an essential part of the urinary system. A narrowing of the patient’s urethra causes complications with the flow of urine.
Various parts of the urethra can be affected by the condition. The bulbar urethra is considered the most common area to be affected. Other areas of the structure can be affected, too, including the membranous urethra in men.
This includes the posterior urethra and the anterior urethra. In men, the penile urethra can become constricted due to urethral stricture as well. In such a case, the scar tissue develops near the region where the tunica albuginea is located.
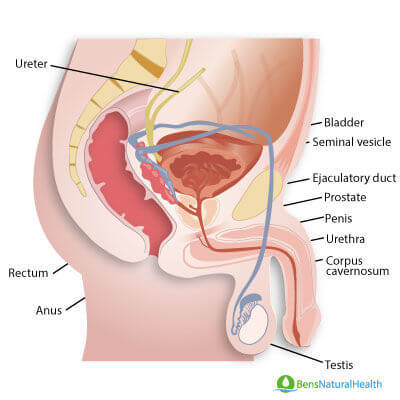
Scar tissue is considered a common reason for urethral stricture to develop. The scar tissue causes the opening of the urethra to become narrower. This reduces the flow of urine. The patient will generally find that their urine flow is weaker and slower. In some cases, urine flow may also be inhibited.
Obstructive voiding dysfunction is a common complication that patients are concerned about. The urinary tract can also suffer when the patient develops urethral stricture.
The condition is more common in men than it is among women. It is also considered a somewhat common condition. Studies have found that about 0.6% of the male population is at risk for urethral stricture2.
Older men have a higher risk of developing the disease. In most cases, the urethral stricture is diagnosed in men who are over 60 years of age.
Patients need to understand what the condition is and how it will affect them. Recognizing the symptoms during an early developmental stage can be beneficial. This ensures the patient receives early treatment.
In many cases, a retrograde urethrogram is one of the first routine tests to show signs of the condition. Once diagnosed, men should ensure the right treatment is offered to them.
What Are The Causes Of Urethral Stricture?
There are several different reasons why urethral stricture can develop.
The stricture can occur at any part of the patient’s urethra. This includes the area where the urethra attaches to the bladder. It can also happen in a different region, such as where the urethra enters the penis in men.
Most men find that no specific cause is identified when they are diagnosed with urethral stricture. There are, however, a few possible causes that have been linked to the occurrence of the condition.
Inflammation: A condition that causes the urethra to be affected by inflammation is a common cause. Various conditions can lead to such complications.
While not very common, the inflammation from Prostatitis could cause problems with the urethra3. This can include a trigger of inflammation. The inflammation can lead to scar tissue building up in the urethra. In turn, a urethral stricture may develop.
STI’S: Sometimes, a sexually transmitted infection can trigger inflammation in the urethra. This, in turn, may also be a factor that causes a urethral stricture to develop. Chlamydia is one sexually transmitted infection that affects the urinary tract. The bacteria can infect the urethra.
Chlamydia would lead to urethritis4. This is a condition that is classified as an inflammation of the urethra. When the patient has urethritis, they can develop a urethral stricture.
Trauma: is another potential cause of urethral stricture. Men who suffer a fall that affects their perineum and scrotum may develop the disease. A trauma that directly affects the urethra also puts the man at risk for a urethral stricture.
Surgery: Certain medical procedures may cause urethral strictures too. This includes the removal of kidney stones. Prostate surgery has also been linked as a possible cause behind the disease.
Pelvic Fracture: Patients who experience a pelvic fracture, often due to a motor vehicle accident, may develop posterior urethral stricture. A straddle injury that causes trauma can lead to anterior urethral stricture. This can also happen when a man suffers a direct injury to his penis.
What Are The Risk Factors For Urethral Stricture?
One of the most critical risk factors to be noted for urethral stricture is gender. Most cases where the condition is diagnosed seem to be found among men. It is relatively rare for a woman to be diagnosed with a urethral structure.
The main reason for this is the fact that a man’s urethra is longer than a woman’s urethra. The longer structure holds more potential for inflammation, scar tissue, and other problems to occur.
Other risk factors should be taken into consideration too.
- Men with benign prostatic hyperplasia seem to be at an increased risk of developing urethral stricture. This is due to the enlargement that occurs in the prostate.
- Any scenario where a tube should be inserted into the tip of the penis can also increase the risk of this disease. This includes urinary catheterization. During this procedure, a catheter is placed into the urethra. The catheter is used with a suprapubic tube. It is then linked with the bladder to collect urine.
- A cystoscope can also increase the patient’s risk for the condition.
- Patients with a sexually transmitted infection are also at a higher risk of developing a urethral stricture5. Chlamydia is not the only STI that should be a concern. There are other STIs that can trigger inflammation of the urethra too.
- Men with certain conditions are at a higher risk too. Lichen sclerosis may rarely affect the penis itself, including on the inside. Balanitis Xerotica Obliterans is another chronic condition that can affect the urethra.
What Are The Symptoms Of Urethral Stricture?
Men should realize what symptoms of urethral stricture can develop. The condition can cause complications with the entire urinary system.
Early diagnosis is a critical part of improving the outlook for this condition. When symptoms associated with urethral stricture are experienced, a man should seek medical assistance.
Symptoms depend from one patient to the next. The severity of the urethral stricture plays a big role in the symptoms that will be experienced.
Sometimes, the symptoms will be mild. Some men experience more serious symptoms. In such a case, the symptoms can interfere with the man’s day-to-day life.
Some of the symptoms that a man may experience when he has a urethral stricture include:
- Sometimes there may be a discharge that comes from the urethra
- The man may need to urinate more frequently
- There may be a consistent need to urinate
- Urinary retention occurs in a lot of men with a urethral stricture
- There may be a loss of the patient’s bladder control
- The urine stream may become slower than normal
- Sometimes, urine sprays during urination
- The penis can sometimes swell up
- The urine may appear darker than usual
- Some men experience blood in their urine
- It is possible for blood to be present in semen too
It should be noted that the location of the urethral stricture also matters. This is another factor that can affect the symptoms experience. Penile urethral stricture, for example, is more likely to cause the penis to swell.
Diagnosis
The first step of diagnosis is a physical examination. The patient should make an appointment with a doctor. The doctor will perform a thorough examination of the patient. The patient will also be asked about the symptoms they experience.
Some abnormalities can be identified through a physical examination. This includes an enlargement of the bladder. The doctor will also be able to identify if the prostate is enlarged or perhaps tender.
The doctor can also look at a discharge that comes from the urethra. In many cases, no obvious abnormalities are identified during the physical examination.
A few tests are needed to provide a diagnosis for urethral stricture. There are a few tests that can be used.
The doctor will not only test for a urethral stricture. Several conditions can cause these symptoms. Thus, other possible causes also need to be ruled out. The doctor may also try to find the cause behind urethral stricture during such tests.
Some of the tests that the doctor may order include:
- STI test (To detect gonorrhea or chlamydia)
- A cystoscopy
- A postvoid residual volume test
- A urinary flow rate test
- A urinalysis
- Voiding cystourethrography can be used
- A urine culture test
- Retrograde urethrography
The specific tests ordered may depend on findings made during the physical examination. The doctor may also order additional tests once they receive the initial results. The doctor also looks at the fossa navicularis of the patient.
What Are The Treatment Methods For Urethral Stricture?
Some treatments can help with a urethral stricture. Treatments are not the same for every patient.
A doctor will try to determine why the man has developed a urethral stricture. When a cause is identified, the doctor will consider addressing the reason for the urethral stricture. This allows further damage to the urethra to be avoided.
Urethral dilation is one of the more common treatments. This is generally done while a cystoscopy is conducted. The doctor will use a topical numbing agent before they start the procedure. The urethra is stretched slightly using a very thin instrument. This instrument is inserted at the tip of the male penis, where the urethra ends.
Certain methods allow men to improve the dilation of the urethra at home. The doctor may explain these procedures to the patient.
Urethral dilation does not always correct the problem. In such a case, alternative treatments need to be considered. Most of the other available treatments may involve a surgical process.
Different surgeries can be performed to treat urethral stricture.
- Internal urethrotomy may be advised. During this procedure, a tool is used to cut the scar tissue that has formed. In recent times, laser urethrotomy is becoming a more commonly used option. A laser is used to cut the scar tissue. This helps to reduce the narrowing of the urethra. A knife may also be used in some cases. A scope is used to assist during the procedure. This allows the doctor to see the inside of the urethra and ensure the stricture is targeted. The scope also helps to reduce the risk of damaging the urethra.
- Open surgery is another option. In such a case, the patient may be provided with urethroplasty. Substitution urethroplasty is sometimes used too. The procedure is sometimes referred to as urethral reconstruction. The stricture is removed through an open surgical procedure.
Reconstruction is then needed. This includes the reconnection of urethral parts that were cut during the surgery. Grafts are sometimes used to assist in reconnecting the urethra. The specific type of urethroplasty conducted depends on where the urethral stricture develops.
- Anterior urethroplasty is used in patients with anterior urethral stricture, for example. Perineal urethrostomy, bulbar urethroplasty, and anastomotic urethroplasty are other options.
- Some patients may undergo a transurethral resection procedure. Primary anastomosis is rarely considered. There are also rare cases where the doctor may recommend an appendicovesicostomy mitrofanoff procedure.
- No drugs are available to treat urethral stricture.
Patients also need to realize that failure to receive treatment can cause complications. The risk of infections is significantly increased. The patient will face a risk of testicular and urinary tract infections.
It is also possible for stones in the bladder to develop when the patient does not receive treatment. Urinary retention is another possible complication that can happen when a urethral stricture is not treated.
How Can I Prevent Urethral Stricture?
There are some cases of a urethral stricture that cannot be avoided. This is generally the case where prostate enlargement causes the condition. The same applies to cases where another condition leads to inflammation of the urethra. This can ultimately contribute to urethral stricture.
Some causes can, however, be prevented. In such a case, the risk of developing a urethral stricture can be reduced. This is not a guarantee that the patient will never develop the condition, but still produces a reduction in the risk.
Sexually transmitted infections can be prevented. With this in mind, men should ensure they practice safe sex. Using a condom can reduce the risk of being infected with chlamydia and gonorrhea.
These conditions have both been linked to an increased risk of urethral stricture. A man should also reduce the number of sexual partners they have. A higher number of sexual partners mean the man is at a greater risk of being infected with an STI.
This is the only effective way of reducing the risk of urethral stricture. Men can prevent serious complications caused by the condition. This can be done by obtaining an early diagnosis and treatment.
Men should notice when they experience symptoms linked to urethral stricture. They should see a doctor when the symptoms develop. This ensures the doctor can recognize the abnormality with the urethra early.
Conclusion
Urethral stricture can limit the flow of a patient’s urine. This can cause several complications to occur. Some patients may also find that the condition causes pain symptoms.
Recognizing symptoms and taking action early on can help to improve the outcome of treatment. There are multiple treatments available. The severity of the condition first needs to be considered by a practitioner. This allows them to decide on a surgical or non-surgical treatment option that would be most appropriate.







