Diabetes mellitus is one of the most common diseases on the face of the earth, and it is responsible for lots of side effects and complications.
One such complication is diabetic neuropathy, and it’s this ailment that we will look at in this blog.
Diabetic neuropathy can be constant, it can be severe, and it can be notoriously difficult to treat.
Because it has a reputation for being so tough to treat, this often leads to people wondering whether diabetic neuropathy can be reversed.
Get Your FREE Diabetes Diet Plan
- 15 foods to naturally lower blood sugar levels
- 3 day sample meal plan
- Designed exclusively by our nutritionist
What is Diabetic Neuropathy?
Before we can look at whether or not this condition can be reversed, we first need to bring you up to speed with what the condition actually is.
There are four main types of diabetic neuropathy; these include:
Peripheral neuropathy
Diabetic peripheral neuropathy is the most common type of diabetic neuropathy. It affects the feet and legs first, followed by the hands and arms.
Autonomic neuropathy
The autonomic nervous system controls your heart, bladder, stomach, intestines, sex organs, and eyes.
Radiculoplexus neuropathy (diabetic amyotrophy).
Moreover, radiculoplexus neuropathy affects nerves in the thighs, hips, buttocks, or legs. It’s more common in people with type 2 diabetes and older adults.
Mononeuropathy
Mononeuropathy, or focal neuropathy, is damage to a specific nerve in the face, middle of the body (torso) or leg. It’s most common in older adults. Mononeuropathy often strikes suddenly and can cause severe pain.
Diabetic neuropathy is best described as being a fairly common, and severe complication of both type 1 and type 2 diabetes.
It is a form of nerve damage, which is the result of fluctuating blood glucose (sugar) levels within the body. Primarily it is high blood sugar levels that are to blame.
Normally it is a progressive disease that sees its symptoms progressively worsen with the passing of each year.
It has been found that individuals that are obese, people with high cholesterol levels, people with high blood pressure, and people with high blood glucose levels are the most susceptible, along with those with diabetes of course.
Symptoms of Diabetic Neuropathy
It typically affects the extremities, with the hands and feet being most commonly affected.
Ordinarily, diabetic neuropathy symptoms manifest themselves in the form of:
- Numbness
- Tingling
- Weakness
- Foot ulcers, Charcot’s foot
- Varying degrees of pain.- Some experience mild pain, while others experience more severe levels of neuropathic pain.
- In very severe cases and cases of peripheral neuropathy, the extremities may become infected or injured, and amputation may be the only solution.
Causes of Diabetic Neuropathy
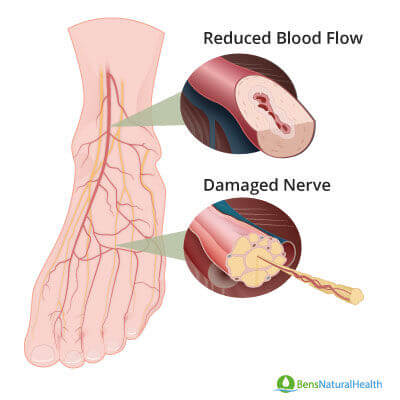
The exact cause likely differs for each type of neuropathy. However, researchers believe that over time, uncontrolled high blood sugar causes nerve damage.
High blood sugar also weakens the walls of the small blood vessels (capillaries) that supply the nerves with oxygen and nutrients.
Managing Diabetic Neuropathy
Diabetic neuropathy can be controlled in a variety of different ways.
Some of the most effective ways of managing the disease require the patient to perform various forms of physical exercise.
Low impact cardiovascular exercise, so things like walking or leisurely cycling are great for enhancing blood vessel health and boosting circulation.
Several studies suggest low-intensity exercise may be of benefit for diabetic patients with neuropathy.
This was shown in a pilot study looking at exercise in previously inactive diabetic patients with peripheral neuropathy.
This study focused on implementing normal walking three times a week for 30 minutes increasingly adding time to 50 minutes over a period of 16 weeks.
Participants were between the ages of 40 and 70 with diabetes and symptoms of peripheral neuropathy.
The pain was assessed using the Brief Pain Inventory Short Form for Diabetic Peripheral Neuropathy. This scale has a pain intensity component as well as pain interference assessments.
Although the data did not suggest a reduction in pain intensities, the results showed a statistically significant improvement in pain interference with daily activities such as walking.
Yoga, meditation, and Tai Chi are also great for managing the condition, as they help to calm the mind and relax the body.
This is very beneficial for the nervous system, plus these types of activity have also been found to reduce blood pressure, stress, and inflammation, which are all contributing factors to the progression of diabetic neuropathy.
Treating Diabetic Neuropathy
As well as managing the condition, there are also ways of actively treating diabetic neuropathy as well.
One of the best ways of helping to treat diabetic neuropathy is to keep your blood sugar levels stable.
As mentioned, one of the leading causes of this condition is dangerously high blood sugar levels.
Therefore, if you wish to treat it, you should aim to keep blood sugar stable. If you use insulin or medication for your diabetes, make sure you take it.
Try to eat fresh and healthy produce, and avoid foods that are very high in carbohydrates or those that contain simple sugars.
Your doctor will determine the best target range for you based on several factors, such as your age, how long you’ve had diabetes, and your overall health.
For many people who have diabetes, the American Diabetes Association generally recommends the following target blood sugar levels:
- Between 80 and 130 mg/dL (4.4 and 7.2 mmol/L) before meals.
- Less than 180 mg/dL (10.0 mmol/L) two hours after meals.
Drugs
If possible, you should try to use drugs as a treatment option only as a last resort.
If you are experiencing painful diabetic peripheral neuropathy, your doctor may prescribe medication as a treatment to help relieve nerve pain.
Commonly prescribed medications include anti-seizure drugs and antidepressants. When considering any medication, discuss the potential side effects with your doctor to determine which is best for you.
Physical therapy
Physical therapy is a great option for people affected by diabetic neuropathy, as this type of treatment can help to alleviate pain and discomfort, while simultaneously reducing the risk of drug dependency.
Electrical nerve stimulation
Electrical nerve stimulation is a painless treatment option that is useful for people experiencing stiffness, numbness, and tingling in the extremities.
Complications of Diabetic Neuropathy
Diabetic neuropathy can vary from person to person in terms of severity. A few potential complications associated with the condition, however, include the following:
Loss of limbs
Damage to the nerves can cause people to lose feeling in their hands and feet. Patients may experience foot sores and ulcers, which could, therefore, become infected and go undetected for a long period of time.
Further, the infection may spread and could cause necrosis of the tissue, meaning that amputation would be the only option.
Reduced blood pressure
Generally, having low blood pressure is more favorable than high blood pressure. However, if blood pressure levels drop too low, you may also be at risk.
If your nerves become damaged, those that control blood flow may be affected, and this could cause a severe drop in pressure. Then, this can lead to light-headedness, dizziness, and even fainting.
Perspiration
Damage to the nerves can also cause disruptions to the sweat glands. This can affect the body’s ability to regulate its temperature.
Those suffering from diabetic neuropathy often experience profuse perspiration, especially while eating, or at night in bed.
Other complications include:
- Sexual dysfunction
- Damage to the joints
- Urinary tract infections
- Hypoglycemia
Can Diabetic Neuropathy be reversed?
Unfortunately, we cannot reverse diabetes nerve damage.
The good news, however, is researchers are reviewing ways to treat and manage nerve damage caused by diabetes. Although you can not reverse neuropathy damage, there are several ways to help manage the condition, including:
- practicing glycemic control
- taking medications your doctor has prescribed for the treatment of neuropathy
- regularly self-checking your feet and legs for injury
- talking with your doctor and working with them to manage your condition
- monitoring blood sugar levels
There are also non-invasive, pain-free options available, which you can discuss with your Doctor or Diabetes Educator.
What else can cause neuropathy?
While diabetes is the most common cause of neuropathy, other conditions can cause it.
This includes:
- tumors
- alcohol addiction
- toxin exposure
- abnormal vitamin B and E levels
- trauma causing nerve pressure
- side effects of medications, for example, chemotherapy
- autoimmune disease and infections
Conclusion
Diabetic neuropathy is a form of nerve damage, which is the result of fluctuating blood glucose (sugar) levels within the body.
Although we cannot reverse diabetic neuropathy, there are a variety of ways we can control it.
In particular, stabilizing blood sugar levels is one of the best ways to control this diabetes complication.
Explore More








