Gastroparesis, A Lesser Known Diabetes Complication
Article Summary
- Gastroparesis is a disorder which affects both type 1 and type 2 diabetics, though it is more common in people with type 1.
- In many cases of gastroparesis, there’s no apparent cause. This is known as idiopathic gastroparesis.
- However, gastroparesis is more likely in people who have high blood sugar levels that go uncontrolled over a long period of time.
- It can be successfully managed by making changes to your diet, medication, and good blood sugar control.
Diabetes is a condition that affects 30.3 million Americans, and numbers are set to rise in the upcoming years.
Although type 2 diabetes can be successfully controlled and even reversed through lifestyle changes, it can also result in a number of health complications.
While many people with diabetes are familiar with common health complications, such as high blood sugar, eye damage, and kidney disease, some may not have heard of gastroparesis.
This is a lesser-known diabetes complication, yet it is becoming an increasing diagnosis for many people with diabetes.
This article will explore what gastroparesis is, its symptoms, and how it can be treated.
What is Gastroparesis?
Gastroparesis is a disorder that affects both type 1 and types 2 diabetics, though it is more common in people with type 1.
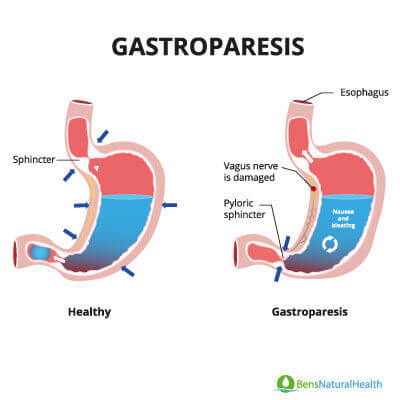
Gastroparesis, also called delayed gastric emptying, is a disorder that slows or stops the movement of food from your stomach to your small intestine, even though there is no blockage in the stomach or intestines,” explains the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK).
Over time diabetes can affect many elements of your body, including the vagus nerve, which controls how your stomach empties its contents and how fast it can do this.
If the vagus nerve is damaged, the stomach does not work properly, and your digestion slows down, affecting gastric motility.
This is defined by the movements of the digestive system and the contents within it.
When nerves or muscles in any portion of the digestive tract do not function with their normal strength and coordination, a person develops symptoms related to motility disorders. This causes food to stay in your stomach longer than it should.
As with other types of neuropathy, diabetes can damage the vagus nerve if blood sugar levels remain high for a long span of time, causing damage to the nerves.
What Causes Gastroparesis?
In many cases of gastroparesis, there’s no apparent cause. This is known as idiopathic gastroparesis.
However, it has been shown that people with diabetes are at higher risk of developing it.
Research has shown that the prevalence of gastroparesis in people with type 1 diabetes ranges from 27- 58% and for people with type 2 diabetes is around 30%.
Controlling blood sugar levels is of the utmost importance, not only for managing your present condition but to prevent the development of dangerous health complications down the line.
Gastroparesis is more likely in people who have high blood sugar levels that go uncontrolled over a long period of time.
Long lapses of high blood glucose levels result in nerve damage, including the vagus nerve and digestive tract, which could eventually lead to gastroparesis.
Other causes not related to diabetes include:
- Surgery causes damage to the vagus nerve.
- Medications (such as narcotics and some antidepressants).
- Parkinson’s disease.
- Multiple sclerosis.
- Rare conditions such as amyloidosis (deposits of protein fibers in tissues and organs).
What are the symptoms of Gastroparesis?
Some of the symptoms of gastroparesis include the following:
- Heartburn or acid reflux.
- Delayed gastric emptying.
- Nausea and vomiting.
- Problems controlling blood sugar.
- Feeling full quickly when eating (Early satiety).
- Abdominal bloating/ abdominal pain.
- Poor appetite.
- Weight loss.
What are the complications of Gastroparesis?
- Constant vomiting can cause dehydration.
- Food that is not digested can harden into a solid mass called a bezoar. Bezoars can cause nausea and vomiting and may be life-threatening if they prevent food from passing into your small intestine.
- If food stays too long in the stomach, it can lead to bacterial overgrowth because the food has fermented.
- Unpredictable blood sugar changes. Although gastroparesis doesn’t cause diabetes, frequent changes in the rate and amount of food passing into the small bowel can cause erratic changes in blood sugar levels.
- Decreased quality of life. An acute flare-up of symptoms can make it challenging to work and keep up with other responsibilities.
Diagnosis methods
Gastric Emptying Test-The The most common way of diagnosing gastroparesis is through a test called a gastric emptying study. This study involves consuming a meal that contains a small amount of radioactive metal.
A scanner is then placed over the stomach for several hours to monitor the radioactivity in the stomach. If the scan results show that more than 10% of food is still in your stomach after 4 hours, you are diagnosed with gastroparesis.
Gastric manometry– This involves having a thin tube passed through your mouth, into the stomach. This is done to measure the stomach’s electrical and muscular activity, helping to determine your ability to digest food.
Upper endoscopy also known as EGD is a procedure in which a thin scope with a light and camera at its tip is used to look inside the upper digestive tract — the esophagus, stomach, and first part of the small intestine called the duodenum.
Barium X-ray– This process involves drinking a liquid substance (barium) that coats the stomach and small intestine, showing up clearly on an x-ray.
Treatment of Gastroparesis
Gastroparesis is a chronic condition, and there is currently no known cure. However, it can be successfully managed by making changes to your diet, medication, and good blood sugar control.
Your doctor might refer you to a dietitian who will help you implement the necessary dietary changes. Some of their suggestion may include:
- Avoiding high fiber foods fruit and vegetables, such as broccoli and oranges.
- Eating well-cooked fruit and vegetables rather than raw.
- Eating smaller meals.
- Avoiding carbonated drinks, smoking, and alcohol.
- Drinking lots of water to stay hydrated, especially if you are vomiting.
- Avoiding high-fat foods may be difficult to digest.
It is important when making changes to your diet to check blood sugar levels frequently after eating. Be sure to monitor your blood glucose regularly and consult with your doctor about any changes you may need to make to your insulin.
Conclusion
At times, diabetes can feel like a condition that takes over your life.
While it can be easy to panic on learning the health complication of diabetes, this article isn’t set out to frighten you but simply to give you an understanding of the risks.
Taking the time to become informed and educated about your condition will be a big help when it comes to managing your diabetes and finding treatment.
Yes, as a diabetic, you are at risk of a number of health complications, but by knowing how to maintain a healthy lifestyle, you can prevent developing any in the first place.
This article is for informational purposes only and does not serve as medical advice. The details provided here are not a replacement for, and should never be depended upon as, professional medical advice. Always consult your physician regarding the potential risks and benefits of any treatment.
Our Medical Review Process
At Ben’s Natural Health, we are committed to maintaining the highest standards of accuracy, transparency, and scientific integrity. Every piece of content is carefully developed by medical professionals and undergoes a thorough review every 12 to 24 months. This ensures that our information remains current, reliable, and rooted in credible, evidence-based research. We reference only peer-reviewed studies from reputable medical journals, providing full citations and direct links to enhance trust and confidence. Learn more about our medical review process and research standards.
Our Editorial Guidelines
For over 25 years, Ben’s Natural Health has been a trusted source of scientifically backed, reliable health information. Our editorial guidelines uphold the highest quality and integrity for every article we publish. Each piece is written by qualified experts and undergoes independent quality checks. We prioritize transparency by clearly displaying contributor credentials and biographies at the beginning of every article. Read more about our editorial standards.
Medical Disclaimer
The content on this blog is for informational purposes only and should not be considered a substitute for professional medical advice, diagnosis, or treatment. While our articles are authored and reviewed by licensed medical professionals, they may not address your specific health concerns. Always consult a qualified healthcare provider before making any medical decisions.
Article Sources
- Krishnasamy S, Abell TL. Diabetic Gastroparesis: Principles and Current Trends in Management. Diabetes Ther. 2018;9(Suppl 1):1–42. doi:10.1007/s13300-018-0454-9
- Choung RS, Locke GR 3rd, Schleck CD, Zinsmeister AR, Melton LJ 3rd, Talley NJ. Risk of gastroparesis in subjects with type 1 and 2 diabetes in the general population. Am J Gastroenterol. 2012;107(1):82–88. doi:10.1038/ajg.2011.310
- Alipour Z, Khatib F, Tabib SM, et al. Assessment of the Prevalence of Diabetic Gastroparesis and Validation of Gastric Emptying Scintigraphy for Diagnosis. Diyabetik Gastroparezi Prevalansı ve Tanısında Mide Boşalma Sintigrafisinin Geçerliliğinin Araştırılması. Mol Imaging Radionucl Ther. 2017;26(1):17–23. doi:10.4274/mirt.61587
- Janatuinen E, Pikkarainen P, Laakso M, Pyörälä K. Gastrointestinal symptoms in middle-aged diabetic patients. Scand J Gastroenterol 1993;28:427-32. Back to cited text no. 5
- Holt S, Colliver J, Guram M, Neal C, Verhulst SJ, Taylor TV.. (1990). Measurement of gastric emptying rate in humans. Simplified scanning method.. Digestive Diseases and Sciences. 35 (11), p1345-2351.
- Sun XM, Tan JC, Zhu Y, Lin L. Association between diabetes mellitus and gastroesophageal reflux disease: A meta-analysis. World J Gastroenterol. 2015;21(10):3085–3092. doi:10.3748/wjg.v21.i10.3085
- Parkman HP. Idiopathic gastroparesis. Gastroenterol Clin North Am. 2015;44(1):59–68. doi:10.1016/j.gtc.2014.11.015
- Parkman HP, Fass R, Foxx-Orenstein AE. Treatment of patients with diabetic gastroparesis. Gastroenterol Hepatol (N Y). 2010;6(6):1–16.
Article Update History
Updated on 30 May, 2026 (Current Version)
Created on 8 October, 2018
Explore More

Is Diabetes Causing Your Yellow Toenails and Foot Fungus?
If you want to know why your toenails are yellow, we discuss possible causes in this article. Yellow toenails can be associated with diabetes ...

