What Level of Blood Sugar is Dangerous?
Article Summary
- Blood sugar levels are largely influenced by the hormone insulin.
- Disruptions in how the body produces and/or reacts to insulin can lead to blood sugar problems.
- Blood sugar levels that are both too high and too low can cause health problems and can be fatal in serious cases.
Knowing what level of blood sugar is dangerous is important for people with diabetes to stay healthy and prevent complications.
It can also be beneficial for people without a diabetes diagnosis, since knowing what your blood sugar levels are like can lead to earlier intervention for previously undiagnosed blood sugar problems.
Diabetes mellitus, more commonly referred to as diabetes, is a disease that is, unfortunately, becoming increasingly well-known.
Diabetes is a disease affecting the pancreas and its ability to produce the hormone insulin. When the insulin-producing cells of the pancreas are destroyed, or when the body doesn’t respond to insulin as well as it should, blood sugar levels rise, and diabetes can develop.
Insulin helps blood glucose (blood sugar) enter our cells, which is used as fuel to support all of the body’s functions. Without enough insulin, sugar remains in the bloodstream and can become dangerously high. Having high blood sugar over a prolonged period of time is detrimental to health.
What Level Of Blood Sugar Is Dangerous?
According to the University of Michigan, a reading of more than 300 mg/dL in a sequence can be harmful. If you have two or more readings over 300 mg/dL in a run, call your doctor right once. Extremely high blood sugar levels (far above 300 mg/dL) can lead to coma in severe circumstances.
A high blood sugar reading ranges between 180 to 250 mg/dL. Below 70 mg/dl is low blood sugar.
A level of blood sugar above 250 mg/dL or under 50 mg/dL is dangerous and requires medical emergency treatment.
The optimal blood sugar level that you want to achieve is generally between 70 and 130 mg/dL.
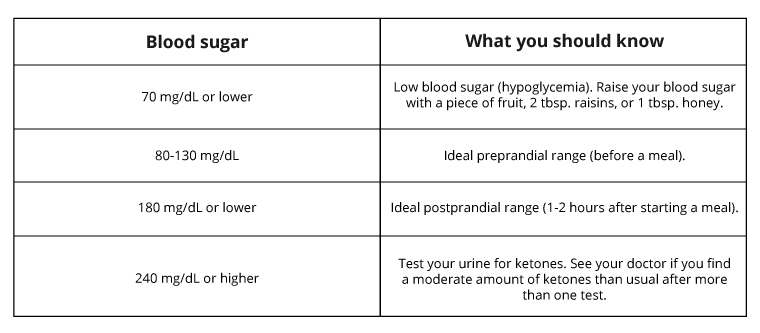
Blood Sugar Chart
Here are some general guidelines for blood sugar ranges:
What are the symptoms of high blood sugar?
The symptoms of high blood sugar can vary depending on severity.
When your blood sugar is around 200 mg/dL, but not yet dangerously high, you may experience the following symptoms:
- Increased thirst
- Frequent need to urinate
- Fatigue
- Achy muscles
- Slightly blurred vision
- Headache
If you have ketones and are at risk of falling into DKA, you may experience these symptoms:
- Nausea
- Vomiting
- Fruity-smelling breath
- Dry mouth
- Weight loss
- Weakness
- Extreme fatigue
- Confusion
- Severely achy muscles
- Extremely blurred vision
- Shortness of breath
- Coma
If you are experiencing any of the later-stage symptoms of high blood sugar, seek immediate medical attention.
What Are the Signs of High and Low Blood Sugar?
Signs of High Blood Sugar
When your blood sugar levels rise, symptoms may include:
- passing more urine than normal, especially at night
- being very thirsty
- tiredness and lethargy
- thrush or other recurring bladder and skin infections
- headaches
- blurred vision
- weight loss
- feeling sick
Signs of Low Blood Sugar
Symptoms of low blood sugar can occur suddenly. They include:
- pale skin
- hunger
- shaking
- sweating
- dizziness
- rapid heartbeat
- mood changes
- irritability/anxiety
- difficulty sleeping
- skin tingling
- blurry vision
- trouble thinking clearly or concentrating
- loss of consciousness

Types Of Diabetes
There are two types of diabetes, type 1 and type 2. Type 2 diabetes is the most common and is linked to insulin resistance. It is more likely to be passed along genetically, and can also occur due to lifestyle factors, such as a sedentary lifestyle.
People can also have a condition called prediabetes, which is when blood sugar levels are slightly elevated, but not enough to be considered diabetes. People with prediabetes are at increased risk of developing type 2 diabetes later on.
[bensnaturalhealthIinlineLeadGen id =”1″ event=”15 Food Blood Sugar eBook Download” image=”https://blog.bensnaturalhealth.com/wp-content/uploads/2021/04/Ipad-15-Foods.png” title=”Get Your FREE Diabetes Diet Plan” content=”##15 foods to naturally lower blood sugar levels ##3 day sample meal plan ##Designed exclusively by our nutritionist”]
What is hyperglycemia?
Hyperglycemia is the term for high blood glucose (sugar) levels. While having sugar in our blood is necessary for survival, having too much blood sugar is unhealthy and can lead to health problems if it remains high over a long period of time.
When someone has diabetes, blood sugar is considered high if it’s above 130 mg/dL before eating, and above 180 mg/dL 1-2 hours after starting a meal based on the American Diabetes Association guidelines.
However, the American Association of Clinical Endocrinologists (AACE) has stricter guidelines for hyperglycemia. AACE considers fasting blood sugar of 110 mg/dL or higher as high as a blood sugar of 140 or higher two hours after a meal.
The most common cause of hyperglycemia is diabetes. Diabetes is classified as type 1 or type 2, with type 2 being the most prevalent type. Type 1 diabetes, also called juvenile-onset diabetes, is often diagnosed before age 18.
What are normal blood sugar levels before and after eating?
For people with and without diabetes, blood sugars should be less than 130 mg/dL before eating to be normal. People without diabetes should ideally have blood sugars in the low 100’s or lower before meals. Still, there isn’t an official recommendation for normal pre-meal blood sugar ranges in non-diabetic individuals.
After eating, people with diabetes should have a blood sugar less than 180 mg/dL one to two hours after starting a meal, or less than 140 mg/dL two hours after a meal, depending on the standards being used (ADA vs. AACE). People without diabetes should have blood sugar less than 140 mg/dL two hours after a meal.
If blood sugar levels are high before eating, it could be a sign of underlying insulin resistance, or a need to increase diabetes medications.
If the blood sugar levels are only high after eating, it can be indicative of a diet-related issue. Making diet changes can significantly help reduce postprandial (after eating) blood sugars. Some people take insulin before eating, so increasing the dose can help with high postprandial blood sugars as well.

Are high levels of blood sugar dangerous?
High blood sugar levels can be dangerous. Blood sugar above 200 mg/dL at any time is considered very high. In type 1 diabetes, very high blood sugar can lead to a life-threatening condition called diabetic ketoacidosis (DKA).
DKA occurs when insulin levels are very low, which causes the body to start producing ketones to use as fuel instead of glucose. A sign of ketone bodies being present is fruity-smelling breath.DKA can be fatal, so prompt medical attention is required.
Some symptoms of DKA include:
- Excessive thirst
- Frequent urination
- Abdominal pain
- Nausea and vomiting
In type 2 diabetes, very high blood sugar can cause hyperglycemic hyperosmolar syndrome (HHS). HHS doesn’t cause ketones to build up, but it does present as:
- Very high blood sugar
- Dehydration
- Decreased alertness
Complications from chronic high blood sugar
Over time, high blood sugar damages the arteries and vessels of the body. When these vessels are damaged, complications can occur.
- Heart (cardiovascular) disease: people with diabetes are two to four times more likely to die from cardiovascular disease than those without diabetes. People with diabetes are also more likely to have high blood pressure, which is another risk factor for heart disease.
- Stroke: Diabetes increases the risk of stroke, as well as increases mortality when a stroke occurs.
- Kidney disease and failure: High blood sugar damages the kidneys and can lead to kidney disease. About one in four people with diabetes have kidney disease.
- Poor wound healing leading to amputations: High blood sugar inhibits proper wound healing. Diabetes is thought to be the leading cause of leg amputations worldwide.
- Neuropathy: Damage to the nerves, which can cause painful symptoms like numb and tingling legs and feet, as well as delayed stomach emptying from damage to the stomach’s nerves.
- Retinopathy and blindness: Damage to the nerves in the eyes is called retinopathy, which can lead to blindness if not treated.
Are low blood sugar levels dangerous?
Low blood sugar is called hypoglycemia. Hypoglycemia occurs when blood sugar falls below 70 mg/dL. Low blood sugar is dangerous, as it can cause dizziness and fainting, which increases the risk of a fall. Prolonged periods of severe hypoglycemia can cause insulin shock. Insulin shock can be life-threatening and lead to coma and death if it’s not treated quickly.
The most common symptoms of hypoglycemia include:
- Feeling shaky and/or dizzy
- Sweating
- Hunger
- Feeling irritable or moody
- Feeling anxious or nervous
- Headache
Severe hypoglycemia can occur if hypoglycemia is untreated.
Signs and symptoms of severe hypoglycemia
- Clumsiness or jerky movements
- Muscle weakness
- Slurred speech or difficulty speaking
- Blurry or double vision
- Drowsiness
- Confusion
- Convulsions or seizures
- Unconsciousness/fainting
- Coma
- Death
Recent studies have associated severe hypoglycemia as a risk factor for dementia, falls, fractures, and heart attacks. Elderly people are at higher risk of hypoglycemia-related fractures; thus, many healthcare providers are more lenient with blood sugar targets in older patients with diabetes.
People without diabetes can also develop hypoglycemia. Some people without diabetes produce too much insulin in response to eating, especially simple sugars like candy and juice. Reactive hypoglycemia usually occurs within a few hours after eating and can happen very quickly in some cases.
Alcohol can cause an increase in insulin secretion as well as interferes with the liver’s ability to create sugar (gluconeogenesis), which can both cause hypoglycemia.
How to lower blood sugar quickly
When high blood sugar levels are treated early, complications such as DKA can be avoided.
Try the following strategies if you have high blood sugar and need to lower it quickly:
Take your insulin exactly as directed
When your body doesn’t have enough insulin or can’t utilize it effectively, your blood sugar rises. Insulin therapy can help you lower your blood sugar levels. Check your blood sugar 15–30 minutes after taking insulin to make sure it’s moving down and not dipping too low.
Exercise
Exercising can help you lower your blood sugar levels quickly and effectively. Exercise can lower blood sugar levels for up to 24 hours after you’ve completed it. This is due to the fact that it makes your body more insulin sensitive.
Physical activity causes the body to demand glucose for energy. As a result, the cells transfer glucose to the muscles, which lowers blood sugar levels.
You’ll need a sort of exercise that makes your heart race faster than usual for this to work. Walking at a fast pace is one example.
If your blood sugar level is more than 240 mg/dl, you should examine your urine for ketones. If you have ketones, don’t exercise because it will raise your blood sugar even more.
Exercising with ketones in your urine raises your risk of high blood sugar problems.
If you have type 1 diabetes, your doctor will almost certainly advise you to monitor your blood sugar levels before exercising. Avoid vigorous exercise if your ketone levels are high and instead opt for mild exercise such as walking.

Tips for healthful living with diabetes
There are many things people with and without diabetes can do to manage their blood sugar levels. Some healthy habits to keep blood sugar levels in a healthy range include:
1) Eat consistent, balanced meals
When you eat a balance of carbohydrates, protein, and fat (otherwise known as the Plate Method), blood sugar tends to rise more slowly and not drop quickly. Foods rich in fiber help promote stable blood sugars, such as whole grains, fruits, vegetables, legumes, nuts, and seeds.
Having a good source of protein with carbohydrates is also good for promoting healthy blood sugar levels. Some protein sources include meat, eggs, fish, dairy products, legumes, nuts, and seeds. Eating protein with carbohydrates can also help reduce reactive hypoglycemia in people without diabetes.
2) Exercise regularly
Being active helps lower insulin resistance and blood sugars. Muscles take up sugar for energy, so doing a mix of cardiovascular exercise (like walking) and weight training (bodyweight exercises or lifting weights) is ideal. Increasing muscle mass can help reduce insulin resistance since muscle tissue takes up glucose regardless of how much insulin is present.
3) Take medications as prescribed
For those with diabetes, it’s important to take diabetes medications as prescribed. Skipping doses, or taking more than prescribed, can be detrimental. Never adjust diabetes medications on your own; always consult with a healthcare provider.
4) Check blood sugar regularly
People who regularly check their blood sugar tend to have better-controlled blood sugar overall. Checking blood sugar levels at home helps people become aware of their blood sugar trends. It can also help people identify how their lifestyle habits affect their blood sugar and make adjustments to achieve better blood sugar control.
5) Practice good sleep hygiene
Poor sleeping habits and shift work link with an increased risk of developing type 2 diabetes. Lack of sleep or a disrupted circadian rhythm seems to interfere with the body’s insulin response, leading to insulin resistance. The National Sleep Foundation also recommends several things to improve sleep hygiene, such as:
- Limiting daytime naps
- Avoiding caffeine and other stimulants close to bedtime
- Exercising during the day
- Avoiding heavy, fatty, or spicy foods close to bedtime
- Exposure to natural light during the day
- Establishing a relaxing bedtime routine
- Keeping the sleeping environment comfortable, e.g., temperature between 60-67 degrees, using white noise machines, etc.
6) Manage your stress
Some studies have suggested a link between stress and the increased risk of developing type 2 diabetes. Stress stimulates our body’s fight or flight response, which can result in increased blood sugar levels and insulin resistance.
Stress can also lead to poor eating habits, low-quality sleep, and other aspects of reduced self-care, which can also contribute to diabetes risk. Finding ways to manage stress can help improve both mental and physical health.
7) Watch your weight
Being at a higher weight (“overweight” or “obese” according to body mass index) is associated with an increased risk of type 2 diabetes. Studies have found that a 5% reduction in body weight in those considered overweight or obese significantly reduced their risk of developing type 2 diabetes. Losing weight can also help reduce blood sugar levels in people with existing diabetes.
Why are good blood sugar levels important?
Healthy blood sugar levels are important for overall health. When blood sugar is high, it does damage to the entire body.
The longer the duration of high blood sugar (chronic high blood sugar or diabetes), the higher risk of developing complications. This is why managing blood sugar in people with diabetes is the biggest goal. Low blood sugar is also dangerous.
Maintaining healthy blood sugar levels can help reduce the risk of developing diabetes later in life. People at increased risk of diabetes should be especially mindful of their blood sugar trends and get screened for prediabetes and diabetes regularly.
Risk factors for type 2 diabetes include:
- Being overweight or obese
- Age >45 years
- Family history of diabetes
- Race/ethnicity
- High blood pressure
- Dyslipidemia
- History of gestational diabetes
- Sedentary lifestyle
- Smoking
- Polycystic ovarian syndrome (PCOS)
- Acanthosis nigricans
Conclusion
Now you know what level of blood sugar is dangerous, this can help you to remain healthy and avoid diabetes complications.
The hormone insulin largely influences blood sugar levels. Disruptions in how the body produces and/or reacts to insulin can lead to blood sugar problems. Blood sugar levels that are both too high and too low can cause health problems and can be fatal in serious cases.
High blood sugar is hyperglycemia, and low blood sugar is hypoglycemia, and both can be dangerous. The optimal blood sugar level falls between those two extremes, generally between 70 and around 130 mg/dL.
People with diabetes can promote healthy blood sugar levels by taking medications as prescribed, checking blood sugar regularly, and practicing healthy lifestyle habits, such as eating a healthy diet and being active.
People without diabetes can promote healthy blood sugar levels by practicing healthy lifestyle habits such as healthy eating, being active, and reducing controllable risk factors for diabetes, like stopping smoking and practicing good sleep hygiene.
Periodically screening for blood sugar problems at preventative healthcare visits is also important since more than 1 in 3 Americans have prediabetes, which significantly increases the risk of developing type 2 diabetes.
Explore More

This article is for informational purposes only and does not serve as medical advice. The details provided here are not a replacement for, and should never be depended upon as, professional medical advice. Always consult your physician regarding the potential risks and benefits of any treatment.
Our Medical Review Process
At Ben’s Natural Health, we are committed to maintaining the highest standards of accuracy, transparency, and scientific integrity. Every piece of content is carefully developed by medical professionals and undergoes a thorough review every 12 to 24 months. This ensures that our information remains current, reliable, and rooted in credible, evidence-based research. We reference only peer-reviewed studies from reputable medical journals, providing full citations and direct links to enhance trust and confidence.
Our Editorial Guidelines
For over 25 years, Ben’s Natural Health has been a trusted source of scientifically backed, reliable health information. Our editorial guidelines uphold the highest quality and integrity for every article we publish. Each piece is written by qualified experts and undergoes independent quality checks. We prioritize transparency by clearly displaying contributor credentials and biographies at the beginning of every article.
Medical Disclaimer
The content on this blog is for informational purposes only and should not be considered a substitute for professional medical advice, diagnosis, or treatment. While our articles are authored and reviewed by licensed medical professionals, they may not address your specific health concerns. Always consult a qualified healthcare provider before making any medical decisions.
Article Sources
- Frankum S, Ogden J. Estimation of blood glucose levels by people with diabetes: a cross-sectional study. Br J Gen Pract. 2005;55(521):944‐948.
- https://www.pcori.org/research-results/2013/does-daily-self-monitoring-blood-sugar-levels-improve-blood-sugar-control-and
- Freckmann G, Hagenlocher S, Baumstark A, et al. Continuous glucose profiles in healthy subjects under everyday life conditions and after different meals. J Diabetes Sci Technol. 2007;1(5):695‐703. doi:10.1177/193229680700100513
- https://care.diabetesjournals.org/content/24/12/2023
- https://www.diabetes.org/diabetes/medication-management/blood-glucose-testing-and-control/checking-your-blood-glucose
- https://www.niddk.nih.gov/health-information/diabetes/overview/preventing-type-2-diabetes/game-plan
Article Update History
Updated on 5 April, 2026 (Current Version)
Created on 12 June, 2020
Explore More

Diabetes MODY: Signs, Causes, Treatment, Lifestyle Changes
MODY stands for maturity-onset diabetes of the young. MODY describes diabetes that is more similar to type 2 diabetes than type 1 diabetes but ...

