Why Is Male Prostate Anatomy Important?

Article Summary
- The prostate gland is an integral part of the reproductive system in the male body.
- While small, it still forms as the most significant accessory gland that is part of a man’s reproductive system.
- Recognition of the prostate gland anatomy is a crucial part of a better understanding of how the gland functions.
The prostate gland is an integral part of the reproductive system in the male body. While small, it still forms as the most significant accessory gland that is part of a man’s reproductive system.
The prostate has many roles to play. Problems with the prostate gland affect more than the reproductive system.
In some cases, the prostate gland can cause problems with the urethra and bladder. This can lead to urinary symptoms.
Recognition of the prostate gland anatomy is a crucial part of a better understanding of how the gland functions.
This also gives a man the ability to understand how specific problems with the prostate can lead to complications.
The prostate’s anatomy also plays a role in testing and diagnosing certain conditions.
Prostate Gland Anatomy
We take a closer look at the prostate gland’s anatomy before considering the importance of understanding the anatomy of this gland. Prostate tissue forms of the prostate gland. We take a closer look at where the prostate gland sits in the abdomen and pelvis1.
A better understanding of the prostate gland also helps a man understand BPH risks and how they can be recognized. The information is also important to help men understand why they need to identify symptoms of BPH and other related conditions.
In turn, this may help a condition like benign prostatic hyperplasia to be diagnosed during an early stage. The result would be a treatment plan that provides more effective results.
Where Is The Prostate Gland Located?
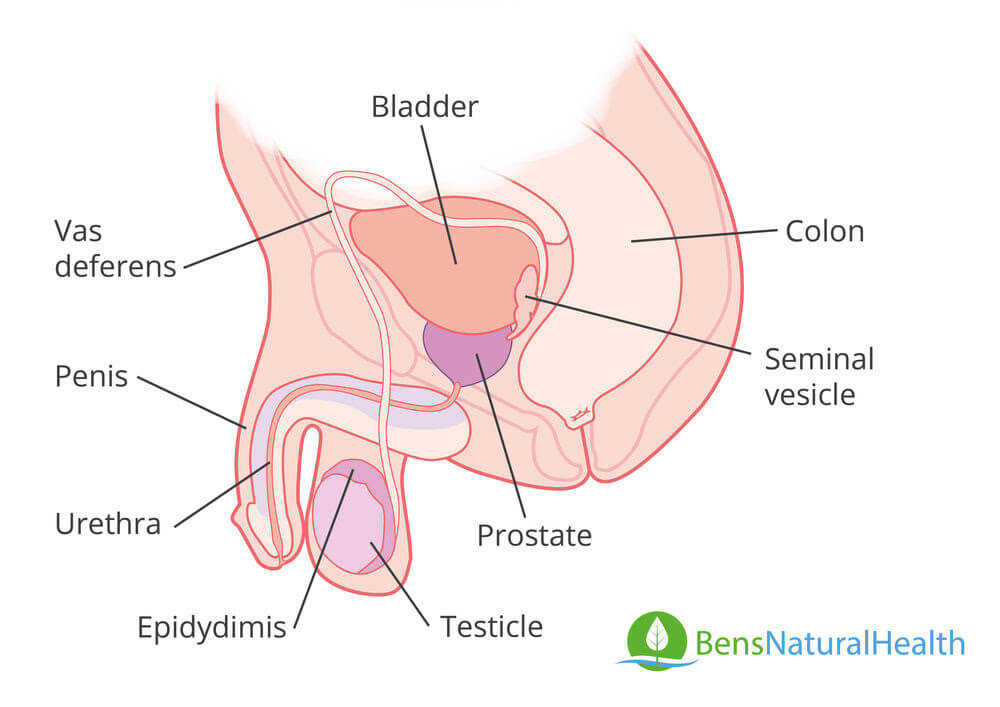
The location of the prostate gland is important. The prostate gland is situated in the pelvis area, along with the other primary parts that make up the male reproductive system. The gland is located just below the neck of the male patient’s bladder.
It surrounds the urethra that comes out of the bladder neck. Nerve supply to the prostate is derived from the prostatic plexus and arterial supply by the branches of the internal iliac artery.
This is why the patient’s urine abilities may change when problems develop with their prostate gland. There are also urinary tract symptoms that tend to develop when the prostate gland becomes enlarged, for example.
This is because the prostate gland’s tissue sits around the urethra. An enlargement can cause a constriction effect in the urethra. This may also cause the prostate gland to push against the bladder’s neck.
[bensnaturalhealthIinlineLeadGen id =”1″ list_name=”funnel_a2_aatp”]
What Is The Anatomical Structure Of The Prostate Gland?
The prostate gland itself is quite small in size. It has a size that is often compared to a walnut.
Even though small, the prostate gland consists of multiple parts that work together. Each part has its role to play in ensuring the prostate gland can perform its appropriate functions.
The prostate is considered a fibromuscular gland. It consists of dense fibromuscular tissue. The shape is often described as an inverted cone. The base of the prostate gland surrounds the urinary bladder’s neck. The apex at the bottom region of the prostate gland sits at the outside of the urethra’s sphincter.
Several layers make up the prostate gland. These should be noted, too, when looking at the anatomy of the gland. At the inside of the prostate gland, there is a collection of tissue called the central one. This forms the base of the prostate gland. The base surrounds the male patient’s ejaculatory ducts.
The most substantial part of the prostate gland is the peripheral zone. This makes up an estimated 70% of the entire prostate gland. The majority of the central zone is surrounded by the tissue that makes up the peripheral zone of the gland. Some of the distal parts that are located at the prostatic urethra are also surrounded by the peripheral zone’s tissue.
A transition zone also forms part of the prostate gland. This is a small part called a glandular zone. It surrounds part of the urethra, located between the verumontanum and the bladder itself.
There is also a fibrous layer that surrounds the entire prostate. This layer is often referred to as a capsule.
The apex of the prostate gland is surrounded by both fibrous tissue and muscular tissue.
What Does The Prostate Gland Connect To?
There are two significant parts of the male body that the prostate gland connects to. The prostate gland sits around the urethra. It does not only sit around the urethra, however, but also connects to it. During ejaculation, sperm is mixed with prostate fluids in this gland. Once mixed, the prostate gland will secrete the combination – called semen – into the urethra.
In addition to being connected to the urethra, the prostate gland is also connected to the ejaculatory ducts in the male body. This is another crucial part of the reproductive system.
It is not only crucial to understand the anatomy of the prostate gland. Men should also ensure they recognize why the anatomy of this gland is so important. Recognition of how prostate tissue is shaped, where it is situated, and other factors related to its anatomy is beneficial. This helps a man better recognize the purpose of the prostate gland in the male reproductive system.
Men with BPH symptoms will also be able to understand why they are having specific problems. For example, when urinary symptoms are experienced, the man will understand how these develop. On a medical level, an understanding of the prostate’s anatomy also helps both physicians and surgeons.
How Does The Prostate Gland’s Anatomy Contribute To Its Function?
There are several ways that the anatomy of the prostate gland contributes to the specific functions that the gland has in the male productive system. The position of the prostate gland should be noted here. The prostate is located between the penis and the bladder2.
As noted previously, it sits just below the neck of the bladder. It surrounds the urethra. The prostate gland also connects to the urethra. The position and connection of the prostate gland and the urethra are what helps with the process of ejaculation.
When a man ejaculates, semen is mixed with prostate fluid, which is then sent to the urethra through the prostate gland. This makes its position ideal for the particular function.
The small size of the prostate also makes it ideal for the particular location where it is situated. Unless enlarged, the prostate gland does not cause any specific problems in the male patient’s body.
What Does The Prostate Do?
An overview of the prostate gland’s functions is also essential. Men need to understand why their prostate gland is such an important part of their body.
The main function of the gland is to produce prostate fluids. This is a fluid that combines with semen during ejaculation. The prostate fluid helps to balance the acidity level of semen. Once combined with semen, it creates a substance called sperm. This is what is expelled from the penis when a man ejaculates.
The prostate fluid itself is considered an acidic compound. Seminal vesicles produce another fluid that is also combined with the semen. This helps to make the semen slightly alkaline. Sometimes the fluid would make the semen basic.
The prostate fluid contains citric acid and zinc, along with certain enzymes3. About one-third of sperm consists of prostate fluid. The nutrients and enzymes found in prostate fluid help to nourish and protect semen. This ensures the semen can survive the acidic environment it will be exposed to in a woman’s vagina.
Why Is Prostate Anatomy Important?
There are several reasons why prostate anatomy is important. Firstly, prostate anatomy contributes to the specific functions performed by this gland.
Without its particular location or structure, it would have been more difficult for the prostate to combine its fluids with semen, thus creating sperm. The prostate’s anatomy also ensures semen can be nourished and protected from acidity – which it is exposed to when the semen enters a vagina.
Anatomic Imaging Of The Prostate
A healthy prostate can produce prostate fluids and nourish semen with no problem. Unfortunately, there is a large number of men who suffer from prostate-related issues.
Chronic prostatitis (chronic pelvic pain)4 is one relatively common issue that men tend to develop. This is a consistent inflammation that affects the prostate gland.
Another common issue that affects the male population would be benign prostatic hyperplasia. This condition is often referred to as BPH or an enlarged prostate. BPH is linked to several potential complications. This includes urinary symptoms, such as frequent urination, urinary incontinence, urinary retention, and even renal failure. The risk increases if the condition is not treated.
Anatomic imaging of the prostate is sometimes used as a way to assist in diagnosing certain prostate-related conditions. The testing procedure can be utilized to assist with identifying prostatitis, an enlarged prostate, and even prostate cancer.
How Is Anatomic Imaging Of The Prostate Performed?
Anatomic imaging of the prostate refers to certain imaging tests being used as a diagnostic tool. These tests are sometimes preferred when the Gleason score returns a suspicious result.
Other tests, such as a PSA test, may also be considered suspicious when levels of the compound are abnormally high.
Magnetic resonance imaging, or MRI, forms as one of the critical elements in prostate anatomic imaging. Scientific papers explain that MRI is one particularly important tool to help with the recognition of prostate cancer5. This is not the only condition that the use of these imaging tests is able to identify.
An endorectal coil will be used when imaging tests are performed from the rectum of the patient. This is an important process in many cases. When a rectal route is chosen to assist with imaging tests, a more transparent overview of the prostate gland can be obtained.
This is because the prostate gland sits in front of the rectum. In such a case, the imaging test may be referred to as a prostate MRI. Other tests can also be performed through this route – including an ultrasound.
What Does Anatomic Imaging Of The Prostate Reveal?
There are several factors that a doctor may be able to identify when anatomic imaging of the prostate gland is performed.
One particularly important factor that doctors are often able to identify through these tests includes prostate cancer. More than 10% of all men will be affected by prostate cancer at some point in their lives6. In 2020, an estimated 191,930 men will be diagnosed with prostate cancer for the first time.
Prostate cancer is not the only factor that may be identified through these imaging tests. Doctors are generally able to identify any abnormalities with the prostate gland through such an analysis. When an anomaly is detected, a doctor may advise the patient to undergo further tests.
When Is Anatomic Imaging Of The Prostate Typically Done?
Anatomic imaging of the prostate gland is not a first-line diagnostic tool. This process is also not done as part of a routine examination that men tend to undergo. It is a diagnostic tool that will only be requested under certain circumstances.
A doctor will generally perform a digital rectal examination during a regular check-up with a male patient. During this procedure, a finger, covered in a glove, will be placed in the patient’s rectum. During this exam, the doctor will feel for abnormalities with the patient’s prostate gland. A digital rectal exam may also be performed when a patient complains about symptoms that signal a problem with his prostate gland.
If an abnormality is detected during a digital rectal exam, then anatomic imaging tests may be advised. These can help to provide a more accurate view of the prostate tissue. It ensures the doctor is able to determine the most appropriate diagnosis to make.
It should be noted that additional tests are often needed after anatomic imaging of the prostate gland. This is especially the case when prostate cancer is suspected.
Prostate Histology And Pathology
When a patient is suspected of suffering problems with their prostate tissue, there are certain things that a doctor needs to take into account. This helps the doctor determine what the patient might be suffering from.
This process generally starts even before any major tests are conducted. The doctor begins to collect data on prostate pathology and histology when the patient initially complains about specific symptoms.
Certain conditions can affect prostate gland function. This is why it is important for a male patient to ensure they consult with a physician when they have symptoms that may signal prostate problems.
Histology helps a doctor determine the specific risks that affect the patient. This can be an important part of choosing the right diagnostic tools. For example, with histology, the physician needs to consider the history of conditions like BPH and prostate cancer in the patient’s family.
Some studies have liked these conditions to certain hereditary and genetic factors. For this reason, a man with a family history of the conditions may be at a higher risk of developing these problems themselves.
This also helps to reduce the risk of unnecessary tests being conducted.
For example, if a man has a family history of benign prostatic hyperplasia, a physician may consider testing for this condition first. This reduces the risk of a needle biopsy being performed, which can have serious side effects.
In cases where the patient does have a family history of prostate cancer, the physician will need to rule the possibility of this disease out. Even in such a case, however, blood and imaging tests may be conducted at first. Gleason score test may be performed. A doctor may also choose to conduct a rectal ultrasound.
The pathology of the prostate gland also plays a role here. When a digital rectal exam or any imaging tests are conducted, the normal pathology of the gland is taken into consideration.
There are specific characteristics that are associated with certain conditions that can affect the prostate gland.
Imaging tests are compared to both normal pathologies of the prostate gland and specific characteristics of these conditions. This allows the physician to have a more accurate way of defining what problems may be affecting the patient’s prostate gland.
Conclusion
Prostate gland anatomy is an important medical subject for both doctors and patients alike. It gives the doctor the ability to understand how to recognize abnormalities with the gland. The patient also gets a better idea of where the prostate is located and how it affects various parts of their pelvis.
Men also understand why certain complications may develop when problems affect the prostate gland. This helps with the recognition of the crucial role that certain tests play.
This article is for informational purposes only and does not serve as medical advice. The details provided here are not a replacement for, and should never be depended upon as, professional medical advice. Always consult your physician regarding the potential risks and benefits of any treatment.
Our Medical Review Process
At Ben’s Natural Health, we are committed to maintaining the highest standards of accuracy, transparency, and scientific integrity. Every piece of content is carefully developed by medical professionals and undergoes a thorough review every 12 to 24 months. This ensures that our information remains current, reliable, and rooted in credible, evidence-based research. We reference only peer-reviewed studies from reputable medical journals, providing full citations and direct links to enhance trust and confidence.
Our Editorial Guidelines
For over 25 years, Ben’s Natural Health has been a trusted source of scientifically backed, reliable health information. Our editorial guidelines uphold the highest quality and integrity for every article we publish. Each piece is written by qualified experts and undergoes independent quality checks. We prioritize transparency by clearly displaying contributor credentials and biographies at the beginning of every article.
Medical Disclaimer
The content on this blog is for informational purposes only and should not be considered a substitute for professional medical advice, diagnosis, or treatment. While our articles are authored and reviewed by licensed medical professionals, they may not address your specific health concerns. Always consult a qualified healthcare provider before making any medical decisions.
Article Sources
- StatPearls. (2019) Anatomy, Abdomen and Pelvis, Prostate. [online] Available at: https://www.ncbi.nlm.nih.gov/books/NBK540987/
- WebMD. Picture of the Prostate. [online] Available at: https://www.webmd.com/men/picture-of-the-prostate#1
- LiveScience. (2010) What Does the Prostate Gland Do? [online] Available at: https://www.livescience.com/32751-what-does-the-prostate-gland-do.html
- Radiology of Infectious Diseases Journal. (2015) Multiparametric MR imaging in the diagnosis of chronic prostatitis and its differentiation from prostate cancer. [online] Available at: https://www.sciencedirect.com/science/article/pii/S235262111500008X
- BioMed Research International. (2014) Anatomic imaging of the prostate. [online] Available at: https://www.ncbi.nlm.nih.gov/pubmed/25243174
- American Cancer Society. Key Statistics for Prostate Cancer. [online] Available at: https://www.cancer.org/cancer/prostate-cancer/about/key-statistics.html
Article Update History
Updated on 8 March, 2022 (Current Version)
Created on 26 March, 2020
Explore More

Guide to Prolapsed Rectum: Signs, Risks, Surgery
Rectal prolapse occurs when the rectum, a section of the large intestine, descends into the anus due to weakened supporting muscles. While it may ...

