Prostate Biopsy: Risks And Side Effects

Article Summary
- Prostate cancer is the most common cancer in men.
- By the age of 50, many men start to get screened, usually undergoing a PSA test.
- Based on the results of the PSA test, a Doctor may recommend a prostate biopsy.
- However, biopsy has a number of adverse side effects and complications that you should be aware of.
Prostate cancer is one of the most common cancers among men worldwide.
Prostate cancer is known to affect a significant proportion of American men during their lifetime. Starting at around the age of 50, many men consider undergoing a PSA test for prostate cancer screening.
If an initial PSA test suggests the possibility of cancer, healthcare professionals may recommend a biopsy to further investigate.
This is to confirm whether cancer is present, as to make a prostate cancer diagnosis and determine the aggressiveness of the disease.
Recent research indicates that a prostate biopsy may be associated with certain negative side effects.
In this article, we will explore the safety of prostate biopsies and discuss potential side effects that could impact one’s quality of life.
[bensnaturalhealthIinlineLeadGen id =”1″ list_name=”funnel_a2_aatp”]
What is a prostate biopsy?
A prostate biopsy is a procedure to detect prostate cancer. They remove small samples of the prostate and then observed them under the microscope.
Doctors may consider a prostate biopsy based on various factors, including elevated PSA levels, but it is a decision made in consultation with the patient, considering their unique medical history and risk factors.
Another is if your doctor detects signs of a prostate problem during your digital rectal exam (DRE). While elevated PSA levels and abnormal DRE findings may raise suspicion of a prostate issue, a biopsy is often used to confirm or rule out cancer, but it is not always necessary.
A prostate biopsy involves:
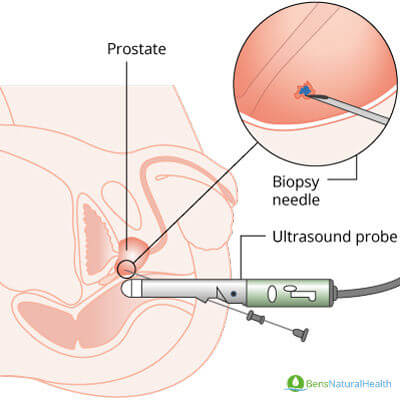
- Collecting minute samples of the prostate gland. The doctor passes a needle through the rectal wall or makes a small cut in the area between the anus and rectum to obtain the samples. A CT or MRI scan is also used to guide them through the procedure.
- A prostate biopsy is a relatively quick procedure, typically lasting around 10 minutes, and is commonly performed in a doctor’s office. The samples will be sent to a lab and will be looked at under a microscope to see if they contain cancer cells.
- If cancer is detected in the patient, it will also be assigned a grade. Typically, biopsy results are available within 1 to 3 days, although in some cases, it may take longer to receive the final report.
Side effects of a prostate biopsy
Although one of the most common procedures for detecting prostate cancer, a prostate biopsy has many potential side effects, risks, and complications which we will discuss below.
1) Bleeding
As with many invasive procedures, there is a risk of bleeding associated with a prostate biopsy. It’s normal to see a small amount of blood in your semen or urine for about two weeks. However, it becomes a significant problem if bleeding takes a long time or if it gets worse.
One study reviewed the safety of transrectal ultrasound-guided needle biopsy. It found that 58 patients (63%) experienced haematuria and experienced rectal bleeding 23 patients (25%).
While severe rectal bleeding is uncommon, it’s a complication that should be recognized and addressed promptly by both patients and healthcare practitioners. So, both patients and practitioners should be aware of the risks.
2) Pain
After the biopsy, it is common for patients to experience discomfort and pain during ejaculation or urination. This usually only lasts for a few days after the procedure, but the degree of pain will vary for each individual.
While some may find it very painful, other people only report a slight discomfort. This is because of the injury caused by the needle on your prostate cells.
A prospective cohort study measured the short-term outcomes of men undergoing a prostate biopsy. The participants were asked to complete a questionnaire, measuring the frequency and effect of symptoms related to pain, infection, and bleeding.
The results found that pain was reported by 43.6%, fever by 17.5%, haematuria (blood in urine) by 65.8%, hematochezia (anal bleeding) by 36.8%, and haemoejaculate (the presence of blood in a man’s ejaculate) by 92.6%)men during the 35 days after a biopsy.
Although researchers in a recent study [insert citation/reference] concluded that most men tolerate prostate biopsy well, it is associated with significant symptoms in a minority of cases and may affect their willingness to undergo repeat biopsy.
Pain is a very important symptom to monitor. Worsening and persistent pain may indicate a bigger problem. If this is the case, you need to see your doctor for a follow-up.
3) Infection
A further risk of having a prostate biopsy is an infection. Surgeons typically prescribe strong antibiotics to reduce the risk of infection, but it’s important to note that infection, while a possible risk, does not always occur.
Research suggests that antibiotic resistance is increasing, which can affect the likelihood of infection. In rare cases, infection may lead to long-term sexual dysfunction, but it’s important to note that such cases are uncommon.
Occasionally, these infections can turn into life-threatening sepsis. This is as needles to detect cancer are passed through the rectum.
As a result, if the needles transport bacteria from the bowel into the prostate, bladder, and the bloodstream, an infection can occur.
A study conducted by researchers at Johns Hopkins and published in The Journal of Urology found that men hospitalized due to biopsy-related infections faced a significantly increased risk of mortality compared to those who did not undergo a biopsy.
4) Acute urine retention
The procedure may result in temporary swelling of the prostate, which, in some cases, can lead to difficulty passing urine.
If the prostate is particularly enlarged (>50mL) or the man has pre-existing risk factors, e.g., a poor flow, a high residual volume or previous urinary retention, then the risks of biopsy-induced urinary retention are significant.
Acute urine retention is a serious medical condition, and if you experience difficulty passing urine following a prostate biopsy, it is essential to seek immediate medical attention. The doctor often inserts a catheter to drain the retained urine, and it will take a few days for you to recover.
5) Sexual problems
Several studies have suggested a risk of temporary erectile dysfunction in some men after prostate biopsy. For instance, a 2015 study published in BJUI International [insert citation/reference] involving 220 men who underwent transrectal prostate biopsy reported an increased risk of temporary erectile dysfunction.
Overall the researchers reported an increased risk of temporary ED after biopsy of approximately 5%.
While the development of temporary erectile dysfunction after a prostate biopsy is relatively rare and typically improves over time, the study suggests that the impact of TRUS-guided prostate biopsy on erectile dysfunction may be underestimated.
It is important to be aware of these prostate biopsy side effects so patients can be appropriately counseled. If sexual problems persist, you should consult your doctor.
Types of prostate biopsy
A prostate biopsy may be done in several different ways:
Transrectal method
At the moment, most biopsies are done using a transrectal ultrasound-guided (TRUS) technique. A TRUS prostate biopsy is where the needle goes through the wall of the back passage (rectum).
Perineal method
This is done through the skin between the scrotum and the rectum.
Transurethral method
This is a type of biopsy done through the urethra using a cystoscope (a flexible tube and viewing device).
Transperineal biopsy
Unlike the TRUS Guided Biopsy, this is where the doctor inserts a needle into the prostate through the skin between the testicles and the anus. This area is the perineum.
The needle is inserted through a template or grid. This is a targeted biopsy, which can focus on specific areas of the prostate using MRI scans. An advantage of the TP biopsy is that it can now be performed under local anesthesia.

Are prostate biopsies safe?
One of the challenges with prostate cancer screening tests is the potential for misdiagnosis, which can lead to overtreatment, but it’s important to consider the benefits and risks of these tests.
Even if you take many samples, a biopsy can still sometimes miss cancer. This occurs if none of the biopsy needles pass through the rights areas. Thus, the biopsy will have a false-negative result.
What is the alternative to a prostate biopsy?
MRI
Recent medical advances have shown that new imaging studies like high-resolution MRI and ultrasound can serve as alternatives to a traditional prostate biopsy.
They have proven to be very accurate and safe. A multi-parametric MRI or a color Doppler ultrasound has a 95 to 98% chance of determining the location and grade of prostate cancer cells.
According to the Diagnostic Center for Disease, An MRI scan can often provide valuable insights into the presence of prostate cancer and may complement traditional biopsy procedures.
A hi-res MRI features the most sensitive and specific imaging modality that allows it to produce a very clear picture of the entire prostate and pelvic region.
Some experts suggest that this approach represents a significant advancement compared to blind biopsy methods, potentially reducing the need for biopsies and offering cost-saving opportunities for the healthcare industry.
An MRI will give you a high resolution 3D image of your prostate and any specialist worth their salt will be able to see if there is growth, or if you’re experiencing the normal indicators of BPH, producing more antigens, therefore raising your PSA.
If you line up an MRI for 90 days time, you will be able to ascertain the rate of growth, if any. That will allow you to act accordingly, as you will have a far better picture than your current ‘snapshot’ and you will still be able to avoid a biopsy. Any specialist will be able to see if there is growth or any progress in the area of suspicion.
PCA3 Test
The PCA3 test, short for ‘Prostate Cancer gene 3,’ is an alternative diagnostic test that detects elevated levels of a specific protein produced by prostate cancer cells.
Unlike the PSA test, a high PCA3 test can only result from cancer – not from an enlarged prostate, inflamed prostate or other non-cancerous prostate problem.
For this test, you need to undergo a Digital Rectal Examination (DRE). This examination helps stimulate PCA3 to leak into the urine.
They then take a urine sample and send it to the lab. It takes about 1-2 weeks to get the results. The higher the PCA3 score, the more likely you have prostate cancer.
This test can also provide insights into the aggressiveness of prostate cancer. A higher PCA3 score may indicate a more aggressive form of the disease.
Our Natural & Non-Invasive Prostate Biopsy Alternative
An alternative to traditional prostate biopsy is the Advanced Prostate Cancer Risk Assessment (APCRA). This consists of non-invasive blood tests and specialized color Doppler scans.
The variety and sophistication of some of these new blood tests make this a very realistic alternative to a prostate biopsy, especially if you have a preference for non-invasive diagnostics and treatments.
After this testing, you will receive a thorough, 3-hour consultation from a Naturopathic Physician who is also a Professor of Urology and a very detailed, written report of your results to be discussed during the appointment.
He will walk you through the results of his assessment and explain every aspect and each option available to you, while also answering any questions that you may have. Your consultation will be like an educational mini-seminar about the real issues facing you as a patient.
Most urologists will have a preference for the particular treatment that they provide. However, the consultant you will see has no agenda and is completely free to offer honest, independent advice.
He will try and help with any information you need in order to arrive at your decision. But he will not try to sway you one way or the other.
Aside from that, the greatest additional benefits of the APCRA are that it is non-invasive, does no damage, and does not close off any avenues for future treatment.
To book our Advanced Prostate Cancer Risk Assessment please call our customer service team on +1-888-868-3554 who will be happy to assist you and offer any further information.
Conclusion
Before undergoing a prostate biopsy, it’s advisable to conduct thorough research and make an informed decision, considering potential side effects. Do not blindly agree to a prostate biopsy without being aware of the possible life-changing side effects it could have.
There are alternative diagnostic methods to consider, such as MRI and the PCA3 test. These methods offer non-invasive options, but their suitability may depend on individual circumstances.
Plus, they don’t have the negative side effects that result from a prostate biopsy.
Have you had a prostate biospy? Share your experience below.
Explore More

Our Natural & Non-Invasive Advanced Prostate Cancer Risk Assessment (APCRA).
This article is for informational purposes only and does not serve as medical advice. The details provided here are not a replacement for, and should never be depended upon as, professional medical advice. Always consult your physician regarding the potential risks and benefits of any treatment.
Our Medical Review Process
At Ben’s Natural Health, we are committed to maintaining the highest standards of accuracy, transparency, and scientific integrity. Every piece of content is carefully developed by medical professionals and undergoes a thorough review every 12 to 24 months. This ensures that our information remains current, reliable, and rooted in credible, evidence-based research. We reference only peer-reviewed studies from reputable medical journals, providing full citations and direct links to enhance trust and confidence.
Our Editorial Guidelines
For over 25 years, Ben’s Natural Health has been a trusted source of scientifically backed, reliable health information. Our editorial guidelines uphold the highest quality and integrity for every article we publish. Each piece is written by qualified experts and undergoes independent quality checks. We prioritize transparency by clearly displaying contributor credentials and biographies at the beginning of every article.
Medical Disclaimer
The content on this blog is for informational purposes only and should not be considered a substitute for professional medical advice, diagnosis, or treatment. While our articles are authored and reviewed by licensed medical professionals, they may not address your specific health concerns. Always consult a qualified healthcare provider before making any medical decisions.
Article Sources
- Glaser, A, Downing, A, Wright, P, Hounsome, L. (2018). Life after prostate cancer diagnosis: One step beyond.. Journal of Clinical Oncology. 36 (6), p40-40 .
- Lee G, Attar K, Laniado M, Karim O.. (2006). Safety and detailed patterns of morbidity of transrectal ultrasound guided needle biopsy of the prostate in a urologist-led uni. International Urology and Nephrology. 38 (2), p281-285.
- Liau, J, Goldberg, D, Arif-Tiwari, H. (2019). Prostate Cancer Detection and Diagnosis: Role of Ultrasound with MRI Correlates. Current Radiology Reports. 7 (7), 0.
- Loeb S, Carter HB, Berndt SI, Ricker W, Schaeffer EM. Is repeat prostate biopsy associated with a greater risk of hospitalization? Data from SEER-Medicare. J Urol. 2012;189(3):867–870. doi:10.1016/j.juro.2012.10.005
- Murray KS, Bailey J, Zuk K, Lopez-Corona E, Thrasher JB1. (2015). A prospective study of erectile function after transrectal ultrasonography-guided prostate biopsy.. BJU International . 116 (2), p90-95.
- Rosario DJ, Lane JA, Metcalfe C, et al. Short term outcomes of prostate biopsy in men tested for cancer by prostate specific antigen: prospective evaluation within ProtecT study. BMJ. 2012;344:d7894. Published 2012 Jan 9. doi:10.1136/bmj.d7894
Article Update History
Updated on 26 October, 2023 (Current Version)
Created on 29 May, 2019
Explore More

Prostatitis Statistics: Key Facts and Insights in 2025
Prostatitis, an inflammatory condition of the prostate gland, remains a key health concern worldwide. In 2025, a deeper understanding of its prevalence, types, diagnosis, ...

