Doctor Answers: What is an MRI Guided Prostate Biopsy?
Article Summary
- An MRI guided prostate biopsy is a type of biopsy in which the prostate is located through MRI technology.
- It is a targeted biopsy that goes directly to the trouble area so it won’t require multiple samples to be accurate.
- The risk of side effects is lower than other needle biopsies, and patients tolerate it more easily.
One promising tool that’s improving how we approach prostate cancer screening is the MRI guided prostate biopsy. We spoke with Dr. Parra, a board-certified urologist, to learn about this advanced technique.
Dr. Parra explains what this biopsy involves, how it compares to traditional methods, and what patients should expect. He also shares insights from recent studies and clinical practice to ensure all readers have accurate, up-to-date information.
[bensnaturalhealthIinlineLeadGen id =”1″ list_name=”funnel_a2_aatp”]
Q: What exactly is an MRI‑guided prostate biopsy?
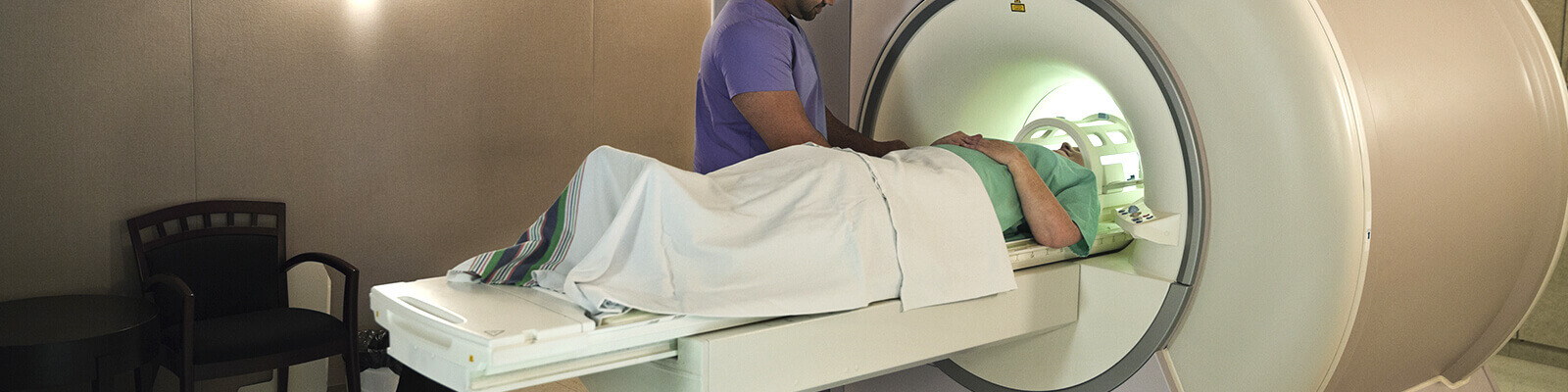
Dr. Parra answers: An MRI-guided prostate biopsy is exactly what it sounds like, a biopsy that uses magnetic resonance imaging (MRI) to guide the needle to specific areas of concern in the prostate. MRI offers far more detailed imaging than X-rays, CT scans, or prostate ultrasound, which helps us pinpoint suspicious regions more accurately; this makes a very detailed picture of the prostate gland.
Now, because MRI involves strong magnetic fields, we can’t perform the biopsy inside the MRI machine itself. So instead, we use a method called fusion-guided biopsy. First, the patient undergoes an MRI scan. Then, we use advanced software to merge those images with real-time ultrasound images taken during the procedure. This fusion allows us to visualize the prostate in great detail and precisely target areas for biopsy.
Q: How is MRI guided prostate biopsy done?
Dr. Parra answers: We only perform it when the MRI reveals a highly suspicious (MRI‑positive) lesion. If no such lesion exists, there’s little value in paying for a fusion biopsy. As research shows, typical candidates include:
-
- Men whose earlier transrectal ultrasound (TRUS) biopsy was negative even though PSA or symptoms still raise suspicion.
-
- Patients already diagnosed with prostate cancer but under active surveillance who need precise monitoring.
Step‑by‑step process
-
- Pre‑biopsy MRI mapping – I outline the prostate and each target lesion (segmentation) on the MRI images, then transfer that data to a procedure workstation.
-
- Image registration – During the biopsy, I sweep a transrectal or transperineal ultrasound probe. The software automatically aligns the live ultrasound with the stored MRI (“rigid registration”) and can perform elastic registration to stretch the MRI overlay for a perfect contour match if needed.
-
- Navigation & sampling – The system supplies real‑time feedback on needle path, optimal patient position, and probe motion, allowing millimetre‑level targeting.
Route choice: I select a transrectal approach unless a patient is infection‑prone or has a history of sepsis, in which case I use the transperineal route.
Q: What are the advantages of an MRI-guided prostate biopsy?
Dr. Parra answers: If you read and understood how MRI works, you won’t be impressed to learn the benefits of this type of biopsy.
As research shows, there are several benefits, which is why this method is gaining popularity.
Reduced number of samples
With traditional biopsies, we usually take 10 or more samples from different areas of the prostate. This increases accuracy but also raises the risk of side effects. With MRI guidance, we only need to sample specific, suspicious areas, so fewer needle insertions are required.
Fewer side effects
Because we take fewer samples, the procedure tends to be more tolerable. Patients report less pain and lower rates of complications like bleeding or infection.
May reduce the detection of clinically insignificant cancers (low-volume, low-grade disease that is unlikely to affect long-term outcomes)
Overdiagnosis is a real concern, some detected cancers don’t require treatment but still cause worry and unnecessary procedures. MRI-guided biopsies are more selective and improve the chances of catching only clinically significant cancers.
Accurate detection of high-grade lesions
This method improves the detection of aggressive, high-Gleason-score cancers. It’s more accurate in spotting the serious cases that need immediate attention.
Offers extra benefits for prostate cancer follow-up
Patients under surveillance or those needing repeat biopsies benefit a lot from this approach. It increases the chance of detecting progression early and helps with proper reclassification of the cancer stage, so treatment can be adjusted accordingly.
Q: Are there any drawbacks to MRI Guided biopsy?
Dr. Parra answers: Like any medical procedure, it’s not perfect. According to research, here are the main limitations.
It only works for MRI-positive lesions
If there’s no suspicious area on the MRI, there’s no point in using this method. Current guidelines from both the American Urological Association (AUA) and European Association of Urology (EAU) recommend multiparametric MRI (mpMRI) prior to the first biopsy in biopsy-naïve men. This improves detection of clinically significant cancers and reduces unnecessary biopsies.
Radiologists score lesions on MRI using the PI-RADS system (1–5). A score of 1–2 indicates a very low likelihood of clinically significant cancer, while scores of 4–5 suggest a high likelihood and usually warrant targeted biopsy.
Can reduce accuracy in BPH
In patients with benign prostatic hyperplasia (BPH) or a normal-looking prostate, this method may not provide much value. It’s not ideal for general screening when no clear abnormality exists.
It is more expensive than the average biopsy
MRI-guided biopsies require advanced software and imaging, which means they’re more costly. For some patients, a standard biopsy is more practical and just as effective.
It is not without side effects
While risks are lower, they’re not zero. You may still experience pain, bleeding, or even an infection, especially if bacteria from the rectum migrate to the prostate during the procedure.
Q: What should patients expect during the procedure?
Dr. Parra answers: This is usually an outpatient procedure, so you’ll go home the same day. Before the biopsy, you’ll be prescribed antibiotics to reduce infection risk, and you’ll continue them for a short period after.
Here’s what happens:
-
- You undergo the MRI first.
-
- Once the image is reviewed, you’ll return for the actual biopsy.
-
- We use a transrectal ultrasound probe and insert the needle alongside it after numbing the area with local anesthesia.
-
- If we use the transperineal route, we go through the pelvic floor, and sedation or a nerve block is typically required.
Q: How does this biopsy compare to other types of prostate biopsies?
Dr. Parra answers: Great question, let me break down a few common methods and how they stack up.
Transrectal ultrasound-guided systematic biopsy (TRUS)
This is the most widely used method. It doesn’t require an MRI and is suitable for initial biopsies. However, because it lacks detailed imaging, we take more samples to ensure accuracy.
Thus, it could be better to use this biopsy instead of an MRI-guided biopsy in some patients who never had a prostate biopsy done in the past.
This type of biopsy does not feature a high-resolution 3D picture of the prostate. Thus, the study confirms that it requires a higher number of samples to diagnose prostate cancer accurately.
Transurethral biopsy
This is less common but still used in some cases. We insert a cystoscope through the urethra and take tissue from inside the prostate. It’s often better for targeting lesions near the urethra.
Transperineal biopsy
The transperineal approach is through your pelvic floor. Compared to the standard transrectal biopsy, this type is more accurate in anterior lesions of the prostate. In other words, if cancer was far from the rectum, a transrectal biopsy won’t reach this area. A transperineal biopsy will.
This biopsy technique is also recommended in patients with a history of sepsis or very severe infections. Compared to the usual transrectal approach, local anesthesia is not enough in this case. Nerve block anesthesia is used instead. You could get an MRI-guided prostate biopsy using a transperineal method. However, it is not the most usual and may not be available everywhere.
Q: What should patients expect after the biopsy?
Dr. Parra answers: Most patients return to normal activities fairly quickly. You might feel sore for a few days, and it’s common to notice small amounts of blood in your urine, stool, or semen.
However, if you experience heavy bleeding, fever, or flu-like symptoms, contact your doctor right away. These could be signs of infection or other complications.
We’ll also schedule a follow-up to check how you’re doing. Depending on your results, you might need further monitoring with PSA tests, digital rectal exams, or additional imaging. Even if the biopsy is negative, we often recommend ongoing evaluations, especially if there’s still concern based on symptoms or PSA levels.
Key FAQs on MRI Guided Prostate Biopsy
Q: Can patients with pacemakers undergo MRI-guided prostate biopsy?
Dr. Parra answers: Depending on the specifications of your pacemaker, you may or may not be a candidate for MRI-guided prostate biopsy. Most scientific literature available online discourages MRI studies and procedures in people with pacemakers and implantable cardiac defibrillators. However, newer devices often address this issue and continue functioning correctly during and after the exam.
Studies show that after the year 2000, pacemakers were designed with MRI technology in mind and are less likely to cause any issues. Furthermore, there is now a term to identify pacemakers that function normally after an MRI. They are called MRI-conditional pacemakers and come equipped with an MRI mode that can be activated to minimize any risk of interference. However, even if you have a new model with this function, it is important to inform your doctor about your pacemaker before your prostate biopsy is scheduled.
The problem with older devices is that the magnetic field created by the MRI machine is made with a type of metal that can be heated and cause dangerous effects. Additionally, MRI scanners can interfere with their function and disrupt the pacing effect. Thus, patients with pacemakers and implantable heart devices are evaluated before, during, and after the procedure to ensure there are no arrhythmias or dangerous side effects.
Q: How soon can sexual activity be resumed after an MRI-guided biopsy?
Dr. Parra answers: The minimum resting period without sexual activity after an MRI-guided biopsy is 48 hours. After that, most people can resume their sexual activity without issues. However, most professionals recommend not adhering strictly to the minimum and resuming sexual activity after 7 days. Depending on individual circumstances, your recommendation may vary, especially if there were complications during the procedure or if it was particularly difficult to complete.
The most common finding after a prostate biopsy of any type is blood in the semen. This symptom can persist for a long time, even up to 48 hours. Therefore, if you continue to see blood in your semen after a few days or weeks, don’t worry. It is a normal finding and doesn’t indicate that something went wrong with your prostate or that it is not healing properly.
An informative pamphlet by the University of Michigan Health System states that blood in the semen usually persists for six weeks. You may also notice blood in your urine, which typically lasts no more than three weeks. Both symptoms are expected during the recovery period, and you should only contact your doctor if there is spontaneous persistent bleeding after seven days or if your urine is cherry-red in color.
Q: Are there specific MRI machines or sequences better suited for prostate biopsy planning?
Dr. Parra answers: The best MRI approach for planning prostate biopsy is known as multiparametric MRI. This imaging style is more detailed than others and is regarded as the gold standard, or the most recommended approach, as long as it is available and patients can afford it. The benefits of multiparametric MRI for prostate biopsy planning reside in the combination of several MRI sequences to evaluate the prostate.
The strength of MRI machines typically ranges from 1.5 to 3 Tesla. This indicates the strength of the magnetic field produced by the imaging device and affects the sharpness and quality of the prostate images. The optimal choice would be a 3T MRI machine for sharper images. However, a 1.5T machine can also be combined with an endorectal coil to enhance image clarity. This small device is placed in the rectum and is generally painless, although it may be somewhat uncomfortable for some patients.
A study published by The Lancet shows that multiparametric MRI is not an unnecessary expense before a prostate biopsy. Quite the opposite; it avoids a primary biopsy in up to 27% of patients who won’t benefit from it. If reducing unnecessary biopsies by a quarter is not enough, MP-MRI can also reduce the over-diagnosis of the disease and improve cancer detection when the problem requires active treatment.
Q: What are the long-term follow-up protocols after a negative MRI-guided biopsy?
Dr. Parra answers: The American Urological Association issued a statement to unify best practices and recommend actions when a patient receives a negative result after an MRI-guided biopsy. Follow-up may still be necessary, which consists of digital rectal exams, PSA measurements, and new imaging tests. The protocol depends on each particular case, especially the PI-RADS score, which reflects the likelihood of cancer a lesion has.
Even if you have a negative biopsy, it was performed due to a very suspicious image on your MRI. Therefore, it is prudent to continue investigating to determine if such lesions change shape or present additional signs and symptoms. For this reason, PSA monitoring enables doctors to assess the progression of your lesion, while digital rectal exams assist in detecting shape abnormalities that might indicate cancer. If suspicions remain high, repeating MRI scans can be useful for monitoring new lesions and observing how existing lesions evolve.
A study published in the Journal of Urology shows how frequently patients with a negative MRI-guided biopsy are later diagnosed with prostate cancer. As mentioned above, this depends on their PI-RADS score. Patients with PI-RADS 3 or higher have a 32% chance of being diagnosed with prostate cancer, even after an initial negative result from the prostate biopsy. In contrast, when PI-RADS scores are lower than 3, the chance of a future prostate cancer diagnosis is minimal. This underlines the need for follow-ups, even when your biopsy results are negative.
Q: Can MRI-guided biopsies detect cancer missed by genomic testing or PSA alone?
Dr. Parra answers: Yes, PSA measurements, genomic testing, and MRI-guided biopsies are different approaches to prostate cancer. Some lesions can be detected by one of these modalities and not by the others. For instance, PSA testing indicates how much of this protein (PSA) leaks into the general circulation. It is a protein produced in the prostate tissue to make semen more fluid, and when the prostate grows, either due to cancer or benign tissue, more PSA is produced.
However, PSA measurements are indirect, and some types of prostate cancer can yield normal results or show no progression in PSA levels. This was confirmed by a study conducted on nearly 20,000 men who had never recorded a high PSA reading in their lives. They also did not have suspicious results in their digital rectal examinations. Nonetheless, 15% of these patients were diagnosed with cancer due to a false negative test. In other words, cancer was missed by their PSA reading.
Something similar occurs with genomic testing, but the exact statistics are more challenging to determine. There is much more involved in cancer than just genetics and family predisposition. Other risk factors can affect the development of prostate cancer, and not all mutations associated with prostate cancer are known. Moreover, some prostate cancers may result from spontaneous mutations that happen during a man’s lifetime, rather than being inherited.
Q: How often do insurance plans cover MRI-guided prostate biopsies?
Dr. Parra answers: Not all insurance plans cover MRI-guided prostate biopsies; some offer coverage only when patients meet specific requirements. The coverage rate may vary based on individual insurance policies and the stance of health authorities on this matter.
However, a study published in the Journal of the American College of Radiology reported that only 11% of patients had their MRI-guided prostate biopsy covered without issues. The remaining 89% must have a previous negative prostate biopsy to receive funding.
Other restrictions may apply, and your insurance company may need a record of PSA levels to determine if there is a rising trend or an abnormal digital rectal examination to approve coverage for MRI-guided prostate biopsies.
Q: Are there any dietary restrictions before undergoing the MRI-guided prostate biopsy?
Dr. Parra answers: There is no specific protocol or list of dietary restrictions for patients scheduled for an MRI-guided prostate biopsy. However, doctors always recommend certain dietary choices to make the experience less uncomfortable.
For instance, in the patient indication brief provided by the Department of Radiology at the University of California, a light evening diet is recommended to avoid gastrointestinal complaints during the procedure. Processed foods and bulky foods are discouraged, while poultry and chicken are considered good dietary choices.
A light breakfast or lunch is also recommended, provided you eat 3 hours prior to the procedure. You should avoid drinking coffee or tea to prevent frequent urination since you’ll have to stay one hour or longer without a bathroom break.
Conclusion
MRI-guided prostate biopsy is an advanced, more targeted way to diagnose prostate cancer. It’s not suitable for everyone, but in the right patients, especially those with visible MRI lesions or who need repeated biopsies, it provides more accurate results with fewer complications.
Whether the approach is transrectal or transperineal depends on your anatomy and medical history. Ultimately, this biopsy helps detect aggressive cancer types earlier, monitor disease progression, and guide treatment with greater precision. Be sure to discuss this with your urologist to see if it’s right for your case.
This article is for informational purposes only and does not serve as medical advice. The details provided here are not a replacement for, and should never be depended upon as, professional medical advice. Always consult your physician regarding the potential risks and benefits of any treatment.

Dr. Hamad Shafqat
Medical Doctor & Senior Medical Writer
Dr. Hamad Shafqat is a dedicated physician with over 4 years of experience in clinical medicine, research, and healthcare writing.
Our Medical Review Process
At Ben’s Natural Health, we are committed to maintaining the highest standards of accuracy, transparency, and scientific integrity. Every piece of content is carefully developed by medical professionals and undergoes a thorough review every 12 to 24 months. This ensures that our information remains current, reliable, and rooted in credible, evidence-based research. We reference only peer-reviewed studies from reputable medical journals, providing full citations and direct links to enhance trust and confidence.
Our Editorial Guidelines
For over 25 years, Ben’s Natural Health has been a trusted source of scientifically backed, reliable health information. Our editorial guidelines uphold the highest quality and integrity for every article we publish. Each piece is written by qualified experts and undergoes independent quality checks. We prioritize transparency by clearly displaying contributor credentials and biographies at the beginning of every article.
Medical Disclaimer
The content on this blog is for informational purposes only and should not be considered a substitute for professional medical advice, diagnosis, or treatment. While our articles are authored and reviewed by licensed medical professionals, they may not address your specific health concerns. Always consult a qualified healthcare provider before making any medical decisions.
Article Sources
- Rawla, P. (2019). Epidemiology of prostate cancer. World journal of oncology, 10(2), 63. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6497009/
- Kongnyuy, M., George, A. K., Rastinehad, A. R., & Pinto, P. A. (2016). Magnetic resonance imaging-ultrasound fusion-guided prostate biopsy: review of technology, techniques, and outcomes. Current urology reports, 17(4), 32. https://pubmed.ncbi.nlm.nih.gov/26902626/
- Gordetsky, J. B., Thomas, J. V., Nix, J. W., & Rais-Bahrami, S. (2017). Higher prostate cancer grade groups are detected in patients undergoing multiparametric MRI-targeted biopsy compared with standard biopsy. The American journal of surgical pathology, 41(1), 101-105. https://europepmc.org/article/med/27574875
- Egbers, N., Schwenke, C., Maxeiner, A., Teichgräber, U., & Franiel, T. (2015). MRI-guided core needle biopsy of the prostate: acceptance and side effects. Diagnostic and interventional radiology, 21(3), 215. https://pubmed.ncbi.nlm.nih.gov/25858525/
- Acar, Ö., Esen, T., Çolakoğlu, B., Vural, M., Onay, A., Sağlıcan, Y., … & Rozanes, İ. (2015). Multiparametric MRI guidance in first-time prostate biopsies: what is the real benefit?. Diagnostic and Interventional Radiology, 21(4), 271. https://pubmed.ncbi.nlm.nih.gov/26027768/
- Kinnaird, A., Sharma, V., Chuang, R., Priester, A., Tran, E., Barsa, D. E., … & Marks, L. S. (2020). Risk of prostate cancer after a negative magnetic resonance imaging guided biopsy. The Journal of Urology, 204(6), 1180-1186.
- University of Michigan (2012). Instructions following prostate biopsy. Available online at: https://med.umich.edu/1libr/urology/ProstateBiopsyPostOp.pdf
- Bovenschulte, H., Schlüter-Brust, K., Liebig, T., Erdmann, E., Eysel, P., & Zobel, C. (2012). MRI in patients with pacemakers: overview and procedural management. Deutsches Ärzteblatt International, 109(15), 270.
- Strom, J. B., Whelan, J. B., Shen, C., Zheng, S. Q., Mortele, K. J., & Kramer, D. B. (2017). Safety and utility of magnetic resonance imaging in patients with cardiac implantable electronic devices. Heart Rhythm, 14(8), 1138-1144.
- Ahmed, H. U., Bosaily, A. E. S., Brown, L. C., Gabe, R., Kaplan, R., Parmar, M. K., … & Emberton, M. (2017). Diagnostic accuracy of multi-parametric MRI and TRUS biopsy in prostate cancer (PROMIS): a paired validating confirmatory study. The Lancet, 389(10071), 815-822.
- Thompson, I. M., Pauler, D. K., Goodman, P. J., Tangen, C. M., Lucia, M. S., Parnes, H. L., … & Coltman Jr, C. A. (2004). Prevalence of prostate cancer among men with a prostate-specific antigen level≤ 4.0 ng per milliliter. New England Journal of Medicine, 350(22), 2239-2246.
- Booker, M. T., Silva III, E., & Rosenkrantz, A. B. (2019). National private payer coverage of prostate MRI. Journal of the American College of Radiology, 16(1), 24-29.
Article Update History
Updated on 19 May, 2026 (Current Version)
Created on 23 June, 2021
Explore More
Should You Poop Before A Prostate Exam?
The prostate gland is located below the bladder and in front of the rectum, producing fluid that makes up part of the semen. Below ...


