- What Is Pancreatitis?
- Types Of Pancreatitis:
- Pancreatitis Symptoms
- Where do you feel pancreatitis pain?
- Pancreatitis Diagnosis
- What Causes Pancreatitis?
- Diabetes And Pancreatitis
- What are the complications of pancreatitis?
- Pancreatitis Treatment
- How to Treat Pancreatitis medically
- Preventions/tips
- Foods to eat if you have pancreatitis
- Foods to avoid if you have pancreatitis
- Conclusion
- Source
You may have heard of pancreatitis, but what you may not know is how complex the different types of pancreatitis are.
Your pancreas is an organ that is part of your digestive system and handles hormone secretion.
There is a particular set of symptoms to look out for when it comes to the different types of pancreatitis that we will discuss in this article.
What Is Pancreatitis?
Pancreatitis is an umbrella term used to describe diseases primarily affecting the pancreas. There are two main types of pancreatitis – acute pancreatitis and chronic pancreatitis.
Hereditary pancreatitis is another and the least common type of pancreatitis.
It is a rare condition, which, according to Genetics Home Reference, is thought to affect three to six individuals per million in Europe. Due to the rarity of hereditary pancreatitis, we will not be covering it in this article.
In order to better understand the causes and effects of pancreatitis, it is important to first know a bit about the organ and its’ functions.
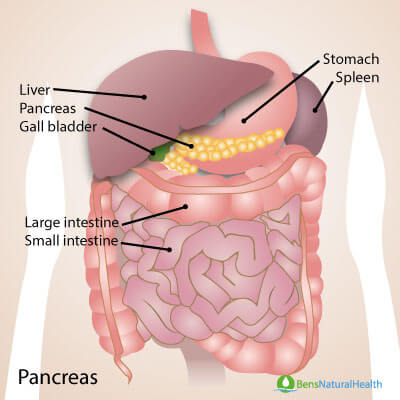
Now, where is the pancreas? This organ measures around 6 inches and is located in your upper abdomen, behind your stomach (1,2). It is made up of several parts and plays a key role in turning the food that we eat into energy for our body’s cells.
Your pancreas is made up of the following three parts (1):
- a wide end (the head)
- a thin end (the tail)
- and the central bit (the body)
It has two main functions, which are the exocrine functions, and endocrine functions.
Exocrine functions assist with digestion, whereas endocrine functions help with the regulation of healthy blood sugar levels.
The endocrine pancreas secretes hormones, which include:
- insulin and glucagon (essential hormones in blood sugar control)
- somatostatin
- ghrelin (the hunger hormone)
- pancreatic polypeptide.
The endocrine cells of the pancreas makeup approximately 5% of the organ and are arranged as something called the islets of Langerhans. The islets of Langerhans are made up of five different types of endocrine cells:
- Alpha cells, and,
- Beta cells (1,2).
A healthy pancreas is also essential for the maintenance of optimum blood glucose (sugar) levels (2,3). There is a link between diseases of the pancreas and diabetes.
You may have heard of beta cells in relation to type 1 diabetes. In type 1 diabetes, it is the insulin-producing beta cells that eventually become worn out and stop producing insulin.
You can read some more about type 1 diabetes here.
The exocrine portion of the pancreas is the most significant part, which, as mentioned, helps with digestion. Exocrine pancreatic tissues produce pancreatic enzymes (also known as digestive juices), which allow the digestive process to happen successfully.
Pancreatic enzymes are secreted by the pancreas and flow down a tube (the pancreatic duct) into the duodenum (the top part of the small intestine that is joined to the stomach).
They then continue to digest the food that has left the stomach (1,2). The enzymes made by the pancreas include:
- Lipase, which helps to digest fat
- Amalayse, which helps to digest sugars (carbohydrates).
- Proteases, which help to digest proteins.
As you can see, the pancreas does a lot for a small organ. As with any organ, its functions are complex, and there are many reasons why it may become damaged or diseased.
Types Of Pancreatitis:
Now that we have spent some time looking at the pancreas and its’ functions, we will look at the different types of pancreatitis.
Acute pancreatitis:
Acute pancreatitis is a painful condition that is characterized by inflammation of the pancreas. In acute pancreatitis, the exocrine pancreas becomes red, swollen, and can lead to extreme pain.
Cases of pancreatitis acute can range from relatively mild to life-threatening (4,5). According to the National Pancreas Foundation, deaths from pancreatitis sit at a fairly static level of around 10%, which is a level it has been at for around 20 years.
Chronic pancreatitis:
Although there are similar characteristics between the two most common forms of pancreatitis, there are also crucial differences. Chronic pancreatitis does not improve over time and will lead to permanent damage to the organ.
As chronic pancreatitis develops, it can affect your ability to digest food and make enzymes. This can lead to specific symptoms and complications (see below) (6).
In the UK, chronic pancreatitis is fairly rare. Although these figures are thought to be an underestimate, due to the diagnosis being difficult, it is thought that around 6,000-12,000 cases of chronic pancreatitis are diagnosed each year in the UK (7).
Get Your FREE Diabetes Diet Plan
- 15 foods to naturally lower blood sugar levels
- 3 day sample meal plan
- Designed exclusively by our nutritionist
Pancreatitis Symptoms
There are some shared symptoms between acute and chronic pancreatitis, whereas some symptoms are unique to one type only.
- Pain
For both acute and chronic pancreatitis, there are similarities between the symptoms experienced. Pain may occur in both types, although this is not always the case. For some people with chronic pancreatitis, they experience no pain at all, whereas in acute pancreatitis, it is typical to experience intense pain.
The pain usually starts in the upper abdomen and can spread to the lower back. In both acute and chronic pancreatitis, the pain can become worse upon eating and drinking. In acute pancreatitis, the pain would usually last several days in the absence of treatment.
People with chronic pancreatitis can experience a significantly reduced quality of life due to the pain that they experience. Being admitted to the hospital for treatment is not unusual.
There are several other shared symptoms of acute and chronic pancreatitis. If you have one either form of the disease, you may experience the following symptoms of pancreatitis (4,5,6,7):
- Nausea and vomiting
- Swollen and tender abdomen
Further symptoms of acute pancreatitis
Some symptoms are far more likely to be present in acute pancreatitis. These include, but are not limited to:
- Fever
- Rapid pulse
In acute pancreatitis, you are likely to feel and look unwell. Typically, people with acute pancreatitis will require treatment, which commonly involves admission to the hospital.
Further symptoms of chronic pancreatitis
Additional to pain and abdominal tenderness, other signs and symptoms of chronic pancreatitis include (4,5,6,7):
- Unintentional weight loss
- Stools that are oily, pale in color, difficult to flush and smell particularly unpleasant
It is common for people with chronic pancreatitis to lose weight, which can lead to malnutrition (8). The reasons for this often rapid weight loss is, are:
- The body is not secreting enough pancreatic enzymes, due to damage to the pancreas/inflammation
- Digestion of food is inhibited
- Nutrient absorption is limited
- Your body cannot maintain weight and carry out usual growth and repair when it is not absorbing adequate nutrients
Where do you feel pancreatitis pain?
Pancreatitis pain tends to begin in your upper abdomen and may spread to your back.
The pain often feels worse after eating.
Some patients describe the pain as ‘gnawing’ or ‘grinding’.
Pancreatitis Diagnosis
Depending on the suspected issue with your pancreas, several tests may be performed to determine and further investigate a diagnosis of pancreatitis.
For acute pancreatitis to be diagnosed, doctors will likely perform the following:
- Blood tests. These will be looking for elevated levels of lipase and amylase, the pancreatic enzymes responsible for helping your body to digest and absorb carbohydrates and fats.
- Levels of amylase or lipase in the blood can be elevated to triple the normal levels in acute pancreatitis.
Diagnosis of acute pancreatitis will also likely involve:
- A physical examination
- Assessment of your medical history.
Once a diagnosis of acute pancreatitis is confirmed, some tests may be necessary to help identify the cause (4,5,6,7,9).
- Computerized Tomography (CT scan). While not typically formed during an initial exploration into acute pancreatitis, a CT scan can be useful. It can help to confirm an uncertain diagnosis or to determine the extent of the damage to the pancreas during illness. It may be used in this case when someone with acute pancreatitis is not recovering as quickly as would be expected.
- An abdominal ultrasound scan. If you have acute pancreatitis, you should have an ultrasound scan to test for gallstones in the gallbladder. Gallstones are the most common causes of acute pancreatitis. It may be that this test is delayed, and is not carried out straight away.
Some further tests may sometimes be, but not always, carried out during investigations of acute pancreatitis:
- Endoscopic ultrasound. This test looks for inflammation and blockages in the pancreatic duct, or in the bile duct.
- Magnetic resonance cholangiopancreatography (MRCP). This test uses MRI imaging and is a sensitive test for looking at the gallbladder, the bile ducts and the pancreas itself, for causes of acute pancreatitis.
This is not an exhaustive list. Depending on your situation, doctors may recommend other tests or examinations.
Diagnosing chronic pancreatitis can be challenging as it is a rare condition. Furthermore, some of the symptoms, such as pain and diarrhea, are similar or the same to those experienced in more common conditions like irritable bowel syndrome.
In order to diagnose chronic pancreatitis, you may be encouraged to have the following test:
- Stool investigations. A test analyzing your stools, called fecal elastase, is a simple way to investigate the function of your pancreas. This can show how effectively your pancreas is producing digestive enzymes and would measure levels of fat in your stool. However, it is not always reliable and would be carried out alongside other tests.
Unlike in acute pancreatitis, blood tests are not typically useful for helping to diagnose chronic pancreatitis. Doctors will still usually perform a physical examination and an assessment of medical history like they do for diagnosing acute pancreatitis.
The best way to diagnose chronic pancreatitis is by using tests that can evaluate the structure and/or function of the pancreas via X-ray (4,5,6,7,9).
Tests available include:
- Transabdominal ultrasound
- Endoscopic ultrasound
- CT scan
- MRCP
What Causes Pancreatitis?
When our digestive enzymes become activated while in the pancreas, they can irritate the cells of your pancreas, this causes inflammation and can lead to pancreatitis.
Unfortunately, repeated episodes of acute pancreatitis can lead to chronic pancreatitis. There are some things you can do to reduce your risk, and these will be discussed later on in the article.
Gallstone pancreatitis
The most common cause of acute pancreatitis is gallstones in the gallbladder. This is called gallstone pancreatitis. The mechanism in which this leads to pancreatitis is not completely clear, although it is thought to be due to the following:
- Gallstones causing a ‘backflow’ of bile into the pancreatic duct, and this can lead to damage or injury of the pancreas
- Obstruction of the flow of normal pancreatic fluid, due to the presence of gallstones that get stuck in the common bile duct. This happens due to the proximity of the small intestine, the main pancreatic duct, and the common bile duct to one another. Stones that get caught in the common bile duct can bear down on the main pancreatic duct, causing the injury of the pancreas.
Excessive alcohol intake
The second most common cause of pancreatitis is excessive alcohol intake. In the UK, gallstones, and drinking too much alcohol combined, account for eight out of ten cases of acute pancreatitis.
Autoimmune pancreatitis
Autoimmune pancreatitis is an autoimmune disorder involving chronic inflammation in the pancreas.
It is likely caused by the immune system attacking the pancreas.
It can be challenging to diagnose because its symptoms are similar to those of pancreatic cancer.
Symptoms
- Fatigue
- Abdominal pain
- Mass or growth in the pancreas
- Back pain
- Unexplained weight loss
There are other causes of acute pancreatitis, although they are far less common:
- Raised triglyceride levels in the blood
- Medication side effects, e.g., from steroids or azathioprine, which is an immunosuppressant medication
- Raised blood calcium levels (hyperkalemia)
- Pancreatic cancer
- Autoimmune conditions
- Uncommon viral infection
tr - As a side effect of ERCP. This is thought to occur in about 1 in 100 ERCP examinations.
There are several well-known causes of chronic pancreatitis, too:
- Heavy alcohol consumption. Alcohol is toxic to the pancreas, and regular drinking, or binge drinking, can cause damage that can lead to both acute and chronic pancreatitis.
- Autoimmune conditions can lead to chronic pancreatitis
- Damage to the pancreas from Cystic Fibrosis can lead to chronic pancreatitis
- A blocked common bile duct or pancreatic duct can be a cause for chronic pancreatitis
- If you have two or more immediate family members with pancreatitis, this can lead to increased risk for yourself. There are also, unfortunately, some unknown causes of pancreatitis chronic.
Diabetes And Pancreatitis
You are likely familiar with type 1 and type 2 diabetes mellitus and maybe even gestational diabetes, but there are also several other subtypes of diabetes. One of these, directly linked to diseases of the pancreas, is type 3c diabetes.
Type 3c diabetes is a form of diabetes that comes secondary to diseases of the pancreas (8).
Damage to the pancreas can occur for various different reasons, some of which we have already explored in this article. Diseases such as chronic pancreatitis, pancreatic cancer, and Cystic Fibrosis can lead to irreversible damage to the pancreas.
When this happens, the pancreas can stop producing enough insulin for the body’s needs. When the body does not have enough insulin, energy cannot get into the body’s cells effectively, which can lead to certain signs and symptoms, as well as the person becoming unwell and requiring treatment, for example, from metformin or insulin (8,9).
NICE guidelines state that a person with type 3c diabetes should be assessed for insulin therapy at least every 6 months.
This may be necessary if metformin is not controlling their blood sugar levels, and they are still losing weight. Yet, evidence of the best treatment in this population is limited, and a randomized control trial is needed (9).
Signs and symptoms of type 3c diabetes include (8):
- Unintentional weight loss
- Oily, pale-colored stools that are difficult to flush
- Diarrhea
- Tiredness
- Abdominal pain
As type 3c diabetes is directly linked to damage to the pancreas, it can also affect the production of digestive enzymes.
As with other types of diabetes, type 3c is complex. Treatment will depend on the extent of the damage to your pancreas. Unfortunately, it is also a condition that is commonly misdiagnosed, as found by a large 2017 primary care study conducted by the BMJ in 2017.
What are the complications of pancreatitis?
Type 3c diabetes is the main complication of chronic pancreatitis (6). Malnutrition is also common, and weight should be monitored alongside symptoms.
A registered dietitian with expertise in the area of pancreatic disease is best placed to offer nutrition support advice to people with pancreatitis. Your doctor can refer you to a registered dietitian if required.
There are also several other potential complications of chronic pancreatitis to be aware of:
- Significantly reduced quality of life. You are advised to contact your doctor for support and to utilize your specialist team. There are several charities out there, such as gutsuk! that can offer advice and support.
- Obstruction, either in the pancreas itself, or the small intestine.
- An increased risk of pancreatic cancer
- You can experience episodes of acute pancreatitis (called acute on chronic pancreatitis).
Pancreatitis Treatment
In acute pancreatitis, intravenous fluids are frequently required upon admission to the hospital. There is good evidence to support the use of intravenous fluid resuscitation, and it has been found to play a crucial role in the outcome of treatment for acute pancreatitis.
Other key treatments may include (4,5,6,7,10):
- Enteral nutrition, either via a nasogastric tube, or a nasojejunal tube. In some cases, intravenous nutrition may be given (total parenteral nutrition). The British Association of Parenteral and Enteral Nutrition (BAPEN) has some fantastic information on the different routes of enteral and parenteral feeding.
- Pain management
- Antibiotic therapy (if the infection is suspected or confirmed)
- Treatments for chronic pancreatitis can include medical and dietary and lifestyle advice. It is strongly advised that people with chronic pancreatitis do not smoke and do not drink alcohol.
How to Treat Pancreatitis medically
Medical treatments may include (4,5,6,7,10):
- Pancreatic enzyme replacement therapy (PERT). Steatorrhea caused by chronic pancreatitis indicates there may be a need for PERT, which is given to help your pancreas achieve optimum enzyme activity again. When PERT is prescribed and taken effectively, it can maximize the absorption of nutrients from your food and help you to maintain a good nutritional status.
- Vitamin supplementation. If you are unable to absorb and digest your food adequately due to chronic pancreatitis and not secreting the necessary enzymes to absorb fat, there are certain vitamins you will not be getting enough of. These are the fat-soluble vitamins, vitamins A, D, E, and K. in chronic pancreatitis; fat-soluble vitamin supplements are usually recommended alongside PERT.
- Traditionally, a low-fat diet was often recommended to help manage chronic pancreatitis. However, the risk of malnutrition can be heightened with a low-fat diet as fat provides valuable calories. A registered dietitian can help you to reduce or manage your risk of malnutrition linked to chronic pancreatitis, and PERT can be considered in view of this.
- Pain management using the World Health Organisation pain ladder approach and possible surgery. The National Pancreas Foundation information on the available treatments for chronic pancreatitis outlines these approaches here.
Preventions/tips
If you suspect you may have, or be at risk of pancreatitis, ensure you speak with your doctor immediately. Pancreatitis is a serious condition that can be extremely debilitating and reduce the quality of life.
There are some lifestyle changes you can make if you think you may be at risk of developing pancreatitis:
- Avoid excessive alcohol intake
- Don’t smoke
- Eat a balanced diet. For the prevention of pancreatitis, this is one that is rich in fruit, vegetables, and whole grains contains moderate amounts of fat from the most nutritious sources, e.g., unsaturated oils, nuts, and oily fish and is varied.
Foods to eat if you have pancreatitis
- Lean meats
- Lentils
- Beans
- Dairy alternatives
- Spinach
- Blueberries
- Tomatoes
- Cucmber
Foods to avoid if you have pancreatitis
- Red meat
- Full-fat dairy
- Fried food
- Butter and margarine
- Added sugars
Conclusion
Pancreatitis is a complex disease, of which there are several types. Acute and chronic pancreatitis is the most common forms that, while are conditions that have some similarities, they also have key differences between one another.
Early detection and treatment will likely lead to better outcomes, and it is essential to consult a specialist for appropriate medical treatment and lifestyle advice.
Next Up








