Signs Metformin Is Not Working and What to Do

Article Summary
- The most obvious signs metformin is not working are having high blood sugar levels and other complications arising from high blood sugar.
- If metformin isn’t working for you, you can make healthy lifestyle changes or possibly add another medication in addition to (or in place of) metformin to make sure you’re meeting your blood sugar goals.
Metformin is a popular medication used to treat type 2 diabetes and tends to be effective for many people who start taking it.
Medications like metformin aren’t always effective for everyone, though.
What are the signs metformin is not working that you should watch out for? Keep reading to find out.
What is metformin?
Metformin is one of the most commonly prescribed medications for type 2 diabetes, and it may also be prescribed to patients with prediabetes. Metformin is the generic name most commonly prescribed, and the brand name for metformin is Glucophage.
There are two types of metformin – regular and extended-release (XR). Extended-release metformin is preferred if you experience side effects or prefer once-daily dosing with your medication.
Metformin doesn’t cause low blood sugar (hypoglycemia), which is one of its major benefits. Because it doesn’t cause low blood sugar, people with type 2 diabetes can take metformin along with other medications like sulfonylureas and injectable insulin.
The common dosage for metformin ranges from 500 milligrams to a maximum of 2,550 milligrams per day. It’s usually recommended to split the dose among meals, typically three times per day.
While metformin is most commonly used for type 2 diabetes, it’s also used to help treat polycystic ovarian syndrome (PCOS). PCOS is a hormonal disorder in women often stemming from insulin resistance, similar to type 2 diabetes and prediabetes.
One of the benefits of metformin is that it may support weight loss and doesn’t promote weight gain like some diabetes medications. If you’re overweight, weight loss of 5-10% of your body weight can improve your blood glucose levels and improve insulin sensitivity.
How does metformin work?
Metformin is in a drug class called biguanides. Biguanides help reduce the amount of sugar your liver makes while improving insulin sensitivity, which helps reduce high blood sugar.
Unlike other types of type 2 diabetes medication, metformin doesn’t stimulate your pancreas to make more insulin, which means it doesn’t carry a risk of low blood sugar.

Potential side effects of taking metformin
More common side effects
The most common metformin side effects are gastrointestinal-related. If you start taking metformin, you may experience some of these side effects:
- Heartburn
- Stomach pain
- Nausea or vomiting
- Bloating
- Gas
- Diarrhea
- Constipation
- Weight loss
- Headache
- Metallic taste in your mouth
Vitamin B12
Metformin might also reduce your body’s ability to absorb vitamin B12 in your stomach. It’s estimated that 6-30% of people taking metformin experience vitamin B12 deficiency. According to studies, the higher the metformin dose, the greater the risk of vitamin B12 deficiency.
Vitamin B12 is important for creating DNA and red blood cells. Vitamin B12 deficiency can lead to anemia, which is when you have lower levels of red blood cells than is healthy.
Anemia from vitamin B12 deficiency is called pernicious anemia and comes with symptoms such as:
- Weakness, tiredness, and/or lightheadedness
- Heart palpitations and shortness of breath
- Pale skin
- Nerve problems like numbness or tingling, muscle weakness, or problems walking
- Vision loss
- Mood or behavioral changes
Lactic acidosis
Most people taking metformin will experience only minor side effects. However, there is a low risk of more severe side effects from taking metformin, such as lactic acidosis.
Lactic acidosis is a serious condition where your body creates more lactic acid than your body can clear.
The symptoms of lactic acidosis usually set in quickly and include:
- Abdominal or stomach discomfort
- Decreased appetite
- Diarrhea
- Fast, shallow breathing
- Discomfort
- Muscle pain or cramping
- Unusual sleepiness, tiredness, or weakness
Metformin overdose is the main risk factor for developing lactic acidosis.
If you’re worried about lactic acidosis, consider this position statement from the American Diabetes Association to help put the risk in perspective: “When metformin is used as labeled, the increased risk of lactic acidosis is either zero or so close to zero that it cannot be factored into ordinary clinical decision making.”
How long does metformin take to work?
Metformin will start to work once it builds up in your system, which usually takes around five days.
If your healthcare provider starts you on a low dose of metformin so you can gradually build up to your target dose, it might take longer to assess how well metformin is doing in lowering your blood sugar.
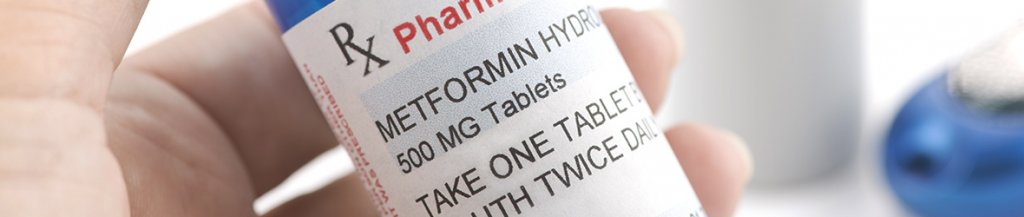
Signs metformin is not working
One of the most obvious signs metformin is not working is high blood sugar. The most accurate way to determine how effective metformin is is to check your blood sugar levels, either at home or at your healthcare provider’s office through a blood test.
Very high blood sugar has symptoms, but most of the time you can’t feel it when your blood sugar is high. If you have very high blood glucose levels, you may experience the following symptoms.
Unintentional weight loss
Your body isn’t able to use glucose as energy when you have high blood sugar. Glucose needs to move from your blood to your cells with the help of insulin to be used as fuel. When cells are starved of glucose for fuel, weight loss can occur as your body breaks down muscle and fat to get its energy.
Increased urination
With uncontrolled type 2 diabetes (and type 1 diabetes), your body will try to rid itself of some of the excess sugar by excreting it in your urine.
If you have high blood glucose levels, you may experience increased urination as your body rids itself of the sugar while pulling fluids along with it, further increasing your urinary output. If you have high blood glucose levels, you’ll have sugar present in your urine that is identifiable with a simple urine test.
Increased thirst
Increased urination can be dehydrating, which can cause increased thirst.
Fatigue
When your body isn’t able to use glucose as energy due to high blood sugar, it can result in a noticeable decline in energy levels.
Increased hunger
When the food you eat isn’t able to be used as energy, it can cause you to feel hungry as your cells starve from the lack of glucose for fuel.
If your blood sugar levels remain high for a long time, you may develop diabetes complications such as:
- Heart disease
- Neuropathy (nerve damage)
- Kidney damage (nephropathy)
- Eye damage (retinopathy)
- Foot wounds/amputations
- Hearing impairment
- Alzheimer’s disease
- Depression
If you take metformin for PCOS, the most common signs metformin is not working could include weight gain, hair loss, acne, high androgen levels/hormonal imbalance, infertility, and lack of improvement of other PCOS symptoms.
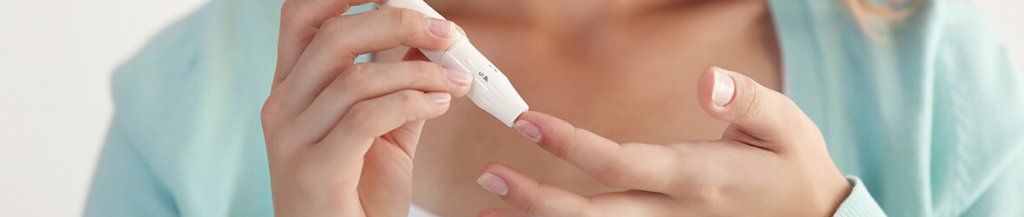
How to check if metformin is working
If you start taking metformin to manage your type 2 diabetes, you’ll probably be curious to see if it’s working. The best way you can check on your own is by testing your blood sugar levels with a glucometer.
If you’re new to checking your blood sugar levels, it’s best to start by taking your fasting blood sugar. You usually take your fasting blood sugar after you wake up and before you eat anything.
Most healthcare providers don’t recommend checking blood sugar multiple times a day when taking metformin. However, testing at other times in the day can provide useful information about your blood sugar trends.
Blood sugar goals
You should ask your healthcare provider what your blood sugar goals are since they vary among patients. Here are some guidelines for optimal blood sugar levels from some of the top diabetes organizations:
According to the American Diabetes Association (ADA), these are the goals for blood sugar in those with diabetes, though individual blood sugar goals do vary.
| Pre-meal: | 1-2 hours after starting a meal: | Hemoglobin A1c (average blood sugar over the past 90 days): |
| 80-130 mg/dL | Less than 180 mg/dL | Less than 7% |
The American Association of Clinical Endocrinologists (AACE) has more strict blood sugar goals as follows:
| Fasting: | 2 hour postprandial (after meal): | Hemoglobin A1c (average blood sugar over the past 90 days): |
| Less than 110 mg/dL | Less than 140 mg/dL | 6.5% or lower |
Blood sugar goals for women with gestational diabetes (diabetes during pregnancy) are the most strict, as high blood sugar during pregnancy can lead to adverse outcomes for mother and baby.
| Fasting/before meals: | 1 hour after a meal: | 2 hours after a meal: |
| 95 mg/dL or less | 140 mg/dL or less | 120 mg/dL or less |
Your healthcare provider can order a hemoglobin A1c test, which is the most accurate way to assess if metformin is working. The hemoglobin A1c test measures your average blood sugar over the past 2-3 months, so it gives a bigger and more accurate picture than checking your blood sugar levels at home.
Does metformin lose effectiveness over time?
Metformin doesn’t necessarily lose its effectiveness over time. Instead, what often happens is that patients starting on metformin develop more insulin resistance.
At the time you’re diagnosed with type 2 diabetes, nearly half of your pancreas’ ability to make insulin is already lost. That means that despite your best efforts, metformin may not be enough to manage your blood sugar levels over time.
The most accurate signs metformin is not working are increasing hemoglobin A1c levels, as well as potentially developing diabetes complications.
What happens if metformin doesn’t work?
If metformin isn’t working, there are other medications your healthcare provider may add to your regimen. The convenient thing about metformin is that you can combine it with many other types of diabetes medications like insulin, sulfonylureas, SGLT 2 inhibitors, DPP 4 inhibitors, and some of the newer injectable diabetes medications since it doesn’t cause low blood glucose on its own.
If metformin isn’t working and you don’t want to add more medications, you can try making healthy lifestyle changes, like the ones we discuss below.
Aim for sustainable weight loss
Losing weight if you’re overweight can help improve blood sugar levels. If you overly restrict yourself, cut out all sugar, or exercise for hours a day to try to lose weight, you likely won’t be able to maintain the weight loss.
You might notice weight loss just by making some healthy lifestyle changes. Sustainable, non-restrictive habit changes that result in weight loss are the best way to go about losing weight to help manage your diabetes or other health conditions.
Losing 5-10% of your initial body weight can help improve blood glucose control by improving insulin sensitivity. For a 200-pound person, that would equate to a 10-20 pound weight loss.
Get regular physical activity
Getting regular physical activity can help with weight loss, but it can also improve blood sugar levels and insulin sensitivity regardless of your weight. Aim to get 30 minutes of physical activity most days of the week.
Eat a blood sugar-friendly diet
A healthy eating style to help manage diabetes is a Mediterranean diet, which is rich in plant-based, high-fiber foods like whole grains, fruits, vegetables, legumes, nuts, and seeds. For protein sources, legumes, fish, and chicken are eaten more frequently than red meat.
Added sugars are eaten the least frequently in a Mediterranean diet, and there is much less reliance on processed food compared to a typical Western diet.
When to see a doctor
You should follow up with your healthcare provider if you are experiencing some of the signs metformin is not working. It’s best to monitor your blood sugar regularly since a drastic change in your blood sugar levels can indicate underlying problems like infections or other illnesses.
It’s also recommended to have a hemoglobin A1c test at least every 6 months, and more often (every 3 months) if your last A1c was above 9%.
Conclusion
The most obvious signs metformin is not working are having high blood sugar levels and other complications arising from high blood sugar. If metformin isn’t working for you, you can make healthy lifestyle changes or possibly add another medication in addition to (or in place of) metformin to make sure you’re meeting your blood sugar goals.
This article is for informational purposes only and does not serve as medical advice. The details provided here are not a replacement for, and should never be depended upon as, professional medical advice. Always consult your physician regarding the potential risks and benefits of any treatment.
Our Medical Review Process
At Ben’s Natural Health, we are committed to maintaining the highest standards of accuracy, transparency, and scientific integrity. Every piece of content is carefully developed by medical professionals and undergoes a thorough review every 12 to 24 months. This ensures that our information remains current, reliable, and rooted in credible, evidence-based research. We reference only peer-reviewed studies from reputable medical journals, providing full citations and direct links to enhance trust and confidence. Learn more about our medical review process and research standards.
Our Editorial Guidelines
For over 25 years, Ben’s Natural Health has been a trusted source of scientifically backed, reliable health information. Our editorial guidelines uphold the highest quality and integrity for every article we publish. Each piece is written by qualified experts and undergoes independent quality checks. We prioritize transparency by clearly displaying contributor credentials and biographies at the beginning of every article. Read more about our editorial standards.
Medical Disclaimer
The content on this blog is for informational purposes only and should not be considered a substitute for professional medical advice, diagnosis, or treatment. While our articles are authored and reviewed by licensed medical professionals, they may not address your specific health concerns. Always consult a qualified healthcare provider before making any medical decisions.
Article Sources
- Kim J, Ahn CW, Fang S, Lee HS, Park JS. Association between metformin dose and vitamin B12 deficiency in patients with type 2 diabetes. Medicine (Baltimore). 2019. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6867725/
- Misbin, Robert (2004) The Phantom of Lactic Acidosis due to Metformin in Patients With Diabetes. https://care.diabetesjournals.org/content/27/7/1791
- Gallwitz B. The fate of Beta-cells in type 2 diabetes and the possible role of pharmacological interventions. Rev Diabet Stud. 2006. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1828283/
- Lashen H. Role of metformin in the management of polycystic ovary syndrome. Ther Adv Endocrinol Metab. 2010. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3475283/
Article Update History
Updated on 30 May, 2026 (Current Version)
Created on 13 April, 2022
Explore More
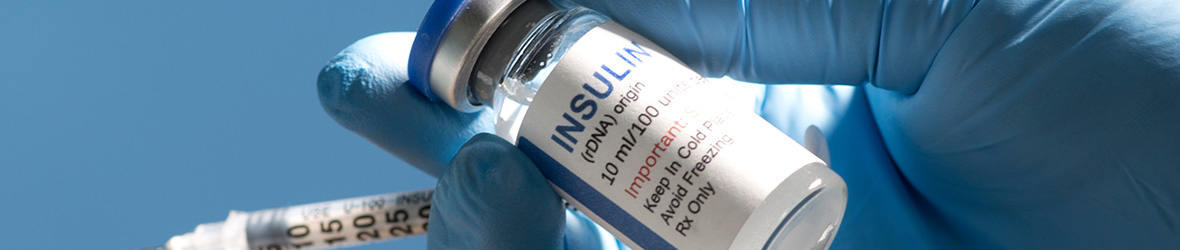
Insulin Overdose: What To Do If You Take Too Much Insulin
Insulin is a vital hormone used to regulate blood sugar (glucose) in the body; however, taking too much insulin can be dangerous. Insulin is ...

