- Q: What are the Different Types of Prostatitis?
- Q: Acute vs Chronic Prostatitis: What is the Key Difference?
- Q: What is Chronic Prostatitis?
- Q: What Causes Chronic Prostatitis?
- Q: What are the Types of Chronic Prostatitis?
- Q: Who is at Risk of Developing Chronic Prostatitis?
- Q: What are the Symptoms of Chronic Prostatitis?
- Q: How is Chronic Prostatitis Diagnosed?
- Q: How to Treat Chronic Prostatitis?
- Q: How to Prevent Chronic Prostatitis?
- Key Patient Questions about Chronic Prostatitis
- Conclusion
- Our Medical Review Process
- Our Editorial Guidelines
- Medical Disclaimer
- Source
If you’re experiencing persistent pelvic pain, urinary issues, or discomfort that won’t go away, you might be dealing with chronic prostatitis. This condition affects many men and can be challenging to diagnose and treat.
We spoke with Dr. Letsa, a leading specialist in urology, to gain deeper insights into chronic prostatitis, its causes, symptoms, and treatment options. In this interview, Dr. Letsa shares his medical expertise and research-backed perspectives to help men better understand this condition and take the right steps toward relief.
All information in this article is based on clinical studies, medical research, and expert analysis provided by Dr. Letsa. The content has been medically reviewed for accuracy and reliability, ensuring that you receive the most up-to-date and trustworthy information on chronic prostatitis.
Q: What are the Different Types of Prostatitis?
Dr. Letsa answers: Prostatitis is an inflammatory condition of the prostate gland, and there are four main types:
- Acute Bacterial Prostatitis – A sudden bacterial infection causing severe symptoms such as fever, chills, and painful urination.
- Chronic Bacterial Prostatitis – A persistent bacterial infection that can come and go over time, leading to recurring urinary tract infections.
- Chronic Non-Bacterial Prostatitis (Chronic Pelvic Pain Syndrome – CP/CPPS) – The most common type, characterized by chronic pain and urinary symptoms without a clear bacterial cause.
- Asymptomatic Inflammatory Prostatitis – This type is typically discovered accidentally during medical exams, as it does not cause noticeable symptoms.
In this discussion, we’ll focus on chronic prostatitis, the most challenging and persistent form of prostatitis.
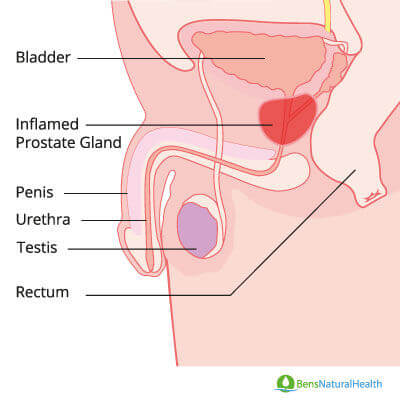
Q: Acute vs Chronic Prostatitis: What is the Key Difference?
Dr. Letsa answers: The main difference between acute and chronic prostatitis is the onset, duration of symptoms, and underlying causes. Acute prostatitis usually presents with sudden and severe symptoms, including intense pelvic pain, fever, chills, and painful or difficult urination. This type is often caused by a bacterial infection, making diagnosis and antibiotic treatment relatively straightforward. These symptoms’ rapid onset and severity require immediate medical attention to prevent complications.
Approximately five percent of men experience symptoms of chronic prostatitis at some point in their lives. Chronic prostatitis accounts for up to 25% of office visits to urologists. Chronic prostatitis is characterized by persistent or recurring symptoms ranging from mild discomfort to significant pain. Common symptoms may include pelvic pain, urinary discomfort, and sexual dysfunction, which can vary in intensity.
Chronic prostatitis differs from acute prostatitis in that it can be caused by various factors, including bacterial infections, nerve damage, or inflammation that does not have a clear infectious cause. This complexity often makes diagnosis and treatment more challenging, requiring a comprehensive approach involving medication, physical therapy, and lifestyle changes. The persistent nature of chronic prostatitis can significantly affect a person’s quality of life, making long-term management strategies essential.
Get Your FREE PSA Lowering Diet Plan!
- Naturally lower PSA levels
- Reduce nighttime trips to the bathroom
- Enjoy better bladder control and urine flow
Q: What is Chronic Prostatitis?
Dr. Letsa answers: Chronic prostatitis is a long-term inflammation of the prostate gland. Unlike acute prostatitis, which appears suddenly and resolves with treatment, chronic prostatitis can persist for months or even years.
This condition can significantly affect a man’s quality of life, causing pain, discomfort, and urinary difficulties. In many cases, the exact cause remains unknown, making it difficult to treat effectively.
Statistics show that prostatitis is one of the most common diagnoses among men visiting urologists. In the United States alone, around two million men seek medical attention for prostatitis annually. Studies show that about 8.2% of men experience symptoms at some point in their lifetime, with chronic prostatitis being the most common type and accounting for up to 95% of cases.
Q: What Causes Chronic Prostatitis?
Dr. Letsa answers: In the majority of cases, when a patient is diagnosed with chronic prostatitis, the cause behind the condition cannot be identified.
Certain tests can be done, but these tests may not yield any valuable data that can help determine why the patient has developed the condition. This, however, is not always the case. For example, when a patient is diagnosed with chronic bacterial prostatitis, then the cause behind the condition is an infection by bacterium species.
Microorganisms can make their way toward the prostate through a tube that is connected to the bladder. This is known as the urethra. In some cases, the infection may initially infect the bladder and then move toward the prostate, as they are located close to each other.
There have been cases before where a contaminated catheter has also caused male patients to develop an infection in their prostate, which led to bacterial prostatitis.
When it comes to chronic prostatitis where no specific cause is found, it should be noted that certain risks and factors can contribute to the condition.
Individuals should note the following possible factors have been linked to chronic prostatitis:
- There are cases where the immune system may start to attack the prostate, which leads to inflammation.
- A compound that forms part of urine, known as uric acid, can irritate the prostate. This can cause inflammation in the area and lead to symptoms associated with chronic prostatitis.
- Certain types of sexually transmitted diseases, such as chlamydia, can cause microorganisms to infect the prostate gland.
- A blockage may sometimes develop that interrupts urination.
- In some cases, an abnormality in muscle or nerve function may also contribute to chronic prostatitis.
Q: What are the Types of Chronic Prostatitis?
Dr. Letsa answers: There are two major types of chronic prostatitis, and each presents unique challenges:
- Chronic Bacterial Prostatitis:
- Caused by a persistent bacterial infection in the prostate.
- Diagnosed through urine or prostate secretion tests.
- Requires long-term antibiotic treatment to manage the infection.
- Chronic Non-Bacterial Prostatitis (CP/CPPS):
- The most common form of chronic prostatitis.
- No bacterial infection is found, even after extensive blood testing.
- Symptoms can be severe and often mimic those of a chronic urinary tract infection or pelvic pain syndrome.
Understanding these subtypes helps us tailor treatment approaches more effectively.
Q: Who is at Risk of Developing Chronic Prostatitis?
Dr. Letsa answers: Chronic prostatitis can affect men of all ages, but it is more common in younger and middle-aged men. Several factors increase the risk:
- A previous history of prostatitis
- Recent urinary tract infections
- Use of a urinary catheter or recent urologic procedures
- Engaging in rectal intercourse
- Structural or functional abnormalities of the urinary tract
- Pelvic trauma from activities like cycling or horseback riding
- Not drinking enough fluids, leading to dehydration
Identifying these risk factors early on can help in preventing or managing symptoms effectively.
Q: What are the Symptoms of Chronic Prostatitis?
Dr. Letsa answers: The symptoms of chronic prostatitis develop gradually and may overlap with other conditions like interstitial cystitis. Common symptoms include:
- Frequent urge to urinate
- Burning sensation while urinating
- Painful ejaculation
- Weak or interrupted urine flow
- Difficulty starting urination
- Persistent feeling of a full bladder after urinating
Additionally, men often experience pelvic pain that affects areas such as:
- Lower abdomen and lower back
- Perineum (area between the anus and testicles)
- Region above the pubic area
Some men may also develop chills or fever, particularly if a bacterial infection is involved. Early recognition of symptoms is crucial for effective treatment.
Q: How is Chronic Prostatitis Diagnosed?
Dr. Letsa answers: The diagnosis of chronic prostatitis involves multiple steps:
- Symptom evaluation – The first step is for the patient to consult with a physician, who will ask the individual more about the symptoms that they are experiencing. A doctor will ask about urinary symptoms, pain levels, and medical history. If the symptoms do not indicate chronic prostatitis, then the physician will likely need to conduct a digital rectal examination. This will help them detect any abnormalities with the prostate gland.
- Digital rectal examination (DRE) – A digital rectal examination is when the physician uses a glove to insert a finger into the patient’s rectum. A lubricant will be used during the procedure. During this examination, the physician will be able to feel if the prostate of the patient is enlarged or tender
- Ultrasound imaging – To assess prostate size and structure. An ultrasound of the patient’s prostate may be ordered following the digital rectum examination. The ultrasound will provide the physician with a view of the patient’s prostate, which allows them to detect inflammation and other issues with the gland.
- Urine, semen, and blood tests – A urine sample will be requested from the patient, which will be used to test for the presence of bacteria. If bacteria are present in the urine sample, then they will be diagnosed with chronic bacterial prostatitis. If symptoms do not improve following antibiotic treatment, or there are no signs of an infection, other tests might be necessary, such as urine, semen, or blood testing to look for signs of infection or other prostate issues.
- Prostate biopsy (if necessary) – To rule out serious conditions like cancer. In some cases, a prostate biopsy may be advised to check prostate health. This involves the Doctor using a needle to remove a small sample of tissue from the prostate for analysis. If the physician can make a diagnosis for chronic prostatitis, then the cause of the condition needs to be identified.
These tests help confirm the diagnosis and determine the most appropriate treatment plan.
Q: How to Treat Chronic Prostatitis?
Dr. Letsa answers: So, how to get rid of chronic prostatitis? Once chronic prostatitis is diagnosed, treatment options are based on the cause and severity of the condition.
For chronic bacterial prostatitis, long-term antibiotic treatment (often 12 weeks) is typically required. This can help clear up the infection and reduce inflammation.
For non-bacterial prostatitis, the goal is to manage symptoms, as no bacterial infection is involved. Several medications can help, including:
- Painkillers and muscle relaxers to relieve pelvic muscle spasms
- Alpha-blockers to help with urinary symptoms
- Anti-anxiety medications may be prescribed to help alleviate pain and discomfort
Heat therapy (such as hot baths or heating pads) can also provide relief from pain and discomfort. Additionally, pelvic floor exercises may benefit men with urinary symptoms. Pelvic floor muscle disorders are responsible for pain in about 50% of CP/CPPS cases, so strengthening these muscles can help.
Some doctors may recommend prostatic massage, though it can be painful or prompt new symptoms in some patients, and is not generally preferred.
Q: Are there any natural or alternative treatments for chronic prostatitis?
Dr. Letsa answers: Many people seek natural and alternative treatments to manage the symptoms of chronic prostatitis, often alongside conventional medical approaches. These treatments aim to alleviate pain, reduce inflammation, and enhance overall well-being.
Common options include herbal remedies such as saw palmetto, quercetin, and beta-sitosterol, which are believed to have anti-inflammatory and muscle-relaxing properties. Acupuncture and massage therapy are also frequently utilized to relieve pelvic pain and muscle tension, promoting relaxation and improved blood flow to the affected area. Cognitive-behavioral therapy (CBT) may also be beneficial in addressing the psychological aspects of chronic pain and in reducing anxiety.
Lifestyle modifications are essential for natural management. Regular exercise, stress reduction techniques like yoga and meditation, and a balanced diet can help strengthen the immune system and reduce inflammation. Pelvic floor and Kegel exercises can enhance muscle control and alleviate urinary symptoms. It’s important to remember that while these alternative treatments may offer symptomatic relief, they should not replace conventional medical care. Consulting with a healthcare provider is crucial to ensure a comprehensive and safe treatment plan.
Q: How to Prevent Chronic Prostatitis?
Dr. Letsa answers: Prevention is always better compared to treating the development of a specific condition. Thus, men should be aware of specific techniques that they can use to reduce their risk of chronic prostatitis possibly.
A man can reduce the likeliness of developing bacterial prostatitis. However, there are times when preventative measures may not completely eliminate the chance of developing chronic prostatitis that is not linked to an infection.
- Good hygiene is the best way to prevent chronic bacterial prostatitis. The man should ensure their penis is always kept clean, which can help to reduce the risk of bacteria entering their urethra.
- Drinking adequate amounts of fluid is also important, as this will help to ensure frequent urination.
If a man suffers a bladder infection or an infection of their urinary tract, then these conditions should be treated as fast as possible. This way, the risk of the bacteria infecting the prostate is reduced.
Key Patient Questions about Chronic Prostatitis
Q: How long does chronic prostatitis last?
Dr. Letsa answers: Chronic prostatitis is a condition that lasting months to years. Unlike acute prostatitis, which usually resolves with antibiotics, chronic prostatitis often requires ongoing management. Factors such as the underlying cause and treatment effectiveness influence its duration.
Regular healthcare follow-ups are vital to monitor symptoms and adjust treatments. While there may not be a definitive cure, many individuals can find significant relief and improved quality of life through medical interventions, lifestyle changes, and alternative therapies by following a management plan.
Q: Can chronic prostatitis lead to prostate cancer?
Dr. Letsa answers: Whether prostatitis increases the risk of prostate cancer is uncertain. Chronic prostatitis and prostate cancer share some symptoms, but there is no definitive evidence that chronic prostatitis directly causes prostate cancer. However, chronic inflammation may increase the risk of developing prostate cancer. Studies are divided, and while inflammation is often seen with prostate cancer, the significance of this is still being researched.
Q: How does chronic prostatitis affect sexual health and fertility?
Dr. Letsa answers: Chronic prostatitis can significantly impact sexual health, causing issues like pain during ejaculation, erectile dysfunction, and decreased libido. The associated psychological distress can exacerbate these problems, leading to frustration and strain on relationships.
Some studies suggest a potential link between chronic prostatitis and male infertility, as inflammation in the prostate may affect sperm quality and motility. This discomfort may also reduce sexual activity, further impacting fertility.
Men facing sexual dysfunction or fertility issues related to chronic prostatitis should consult a healthcare provider for proper evaluation and management.
Q: What lifestyle changes can help manage chronic prostatitis symptoms?
Dr. Letsa answers: Several lifestyle changes can help manage the symptoms of chronic prostatitis:
- Avoid Irritants: Steer clear of alcohol, caffeine, and spicy foods.
- Hydration: Drink plenty of fluids, but limit caffeinated beverages.
- Warm Baths: Soaking in a warm bath can alleviate pelvic pain.
- Pelvic Floor Exercises: Strengthening the pelvic floor muscles can improve urinary symptoms.
- Stress Reduction: Utilizing relaxation techniques to manage stress can help reduce symptom flare-ups.
Q: How does stress and anxiety contribute to chronic prostatitis flare-ups?
Dr. Letsa answers: Stress and anxiety can significantly worsen the symptoms of chronic prostatitis. The pelvic floor muscles surrounding the prostate are particularly sensitive to stress. When individuals experience stress, these muscles can become tense and constricted, leading to increased pain and discomfort. This muscle tension can also disrupt urinary function, resulting in more frequent and urgent trips to the bathroom. Additionally, the psychological effects of chronic pain and urinary issues can contribute to heightened stress and anxiety, creating a vicious cycle.
Moreover, stress can impact the immune system, making individuals more prone to inflammation and infection. The body’s response to stress can trigger the release of inflammatory chemicals, further aggravating prostatitis symptoms.
Q: Can diet impact chronic prostatitis symptoms? If so, what foods should be avoided?
Dr. Letsa answers: Diet can indeed impact chronic prostatitis symptoms. Certain foods and drinks can trigger or worsen symptoms. Here are some foods to avoid:
- Caffeine: Can irritate the bladder and worsen symptoms.
- Alcohol: Can also irritate the bladder and exacerbate symptoms.
- Spicy Foods Can increase rectal sensitivity and trigger symptoms.
- High-Glycemic Carbs: Sugary foods and refined carbohydrates can raise insulin levels and worsen symptoms.
- Fried Foods: Associated with higher prostate cancer risk and can contribute to inflammation.
A diet rich in fruits, vegetables, and whole grains can provide essential nutrients and antioxidants that promote prostate health. Staying hydrated by drinking plenty of water helps flush out toxins and reduce urinary irritation. Additionally, identifying and avoiding individual trigger foods through an elimination diet or keeping a food diary can help manage symptoms.
Conclusion
Chronic prostatitis is a challenging and often painful condition, but with the right diagnosis and treatment plan, many men can manage their symptoms effectively.
Dr. Letsa emphasizes the importance of early detection, lifestyle modifications, and medical interventions to help improve quality of life for men struggling with prostatitis.
Our Medical Review Process
At Ben’s Natural Health, we are committed to upholding the highest standards of transparency, accuracy, and scientific rigor. Each piece of content is meticulously developed by medical professionals and undergoes a thorough review every 12 to 24 months. This ensures that all information is current, accurate, and supported by credible, evidence-based research. We exclusively reference peer-reviewed studies from reputable medical journals and provide complete citations and direct links to enhance trust and confidence. For more details about our review process and research standards, please read about our medical review process.
Our Editorial Guidelines
For over 25 years, Ben’s Natural Health has been a trusted source for reliable, scientifically sound information on natural health. Our editorial guidelines ensure the quality and integrity of every article we publish. All content is written by qualified experts, including doctors, dietitians, nutritionists, fitness professionals, and surgeons, and is independently verified for accuracy. We value transparency, which is why we provide the credentials and biographies of our contributors at the beginning of each article. To learn more about how we create and verify our content, please read our editorial guidelines.
Medical Disclaimer
The content provided on this blog is intended for informational purposes only and should not be considered a substitute for professional medical advice, diagnosis, or treatment. Although our articles are reviewed and written by licensed healthcare professionals, they may not address your specific health needs. Always consult your primary care physician or a qualified healthcare provider before making any health decisions. Do not disregard or delay seeking professional medical advice based on the information found here. Your use of this blog and its content is entirely at your own risk.








