Early-Stage Prostate Cancer: Symptoms & Diagnosis

Article Summary
- Prostate cancer is a type of cancer found only in men. Cancer develops in the prostate gland, which is responsible for producing semen.
- Prostate cancer is the most common cancer among men. Most cases are found in men ages 65 and older.
- The best way to treat prostate cancer is to find it early before cancer can spread to other parts of the body.
- There are a number of options for treating men with prostate cancer. Your doctor will discuss the different options with you so you can make the best decision for your body.
Prostate cancer is a type of cancer found only in men. Cancer develops in the prostate gland, which is responsible for producing semen.
It is located below your bladder and near your urethra. The prostate is about the size of a walnut, but it often grows larger with age.
Prostate cancer is the most common cancer among men. Most cases are found in men ages 65 and older, but men as young as 50 can be diagnosed with this disease.
The best way to treat prostate cancer is to find it early before cancer can spread to other parts of the body.
What is early Prostate Cancer?
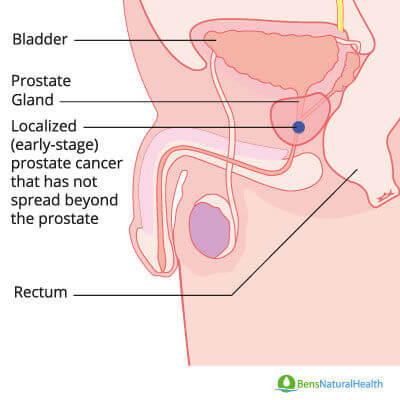
Cancer is divided into four different stages, based on far it has spread. If you have early-stage prostate cancer, then your cancer is either Stage I or II.
This means cancer has not spread outside the prostate gland. Since it is contained, it is easier to treat and does not require common types of cancer treatment, like chemotherapy.
Risk factors for Prostate Cancer
Although the causes of the prostate cancer remain largely unknown, certain factors can increase your risk .
Non-Modifiable Risk Factors:
- Age 55 years or more
- African American race
- Family history of prostate cancer in first-degree relatives (father, brother).
Modifiable Risk Factors
- Overweight
- Sedentary lifestyle
- Unhealthy diet
- Smoking
Symptoms of Early Stage Prostate Cancer
Early prostate cancer often does not have any symptoms. You may have been diagnosed after a routine prostate exam, or it was found while seeking treatment for a different ailment.
Many times, the symptoms of early prostate cancer mimic those of the swelling of the prostate gland, which is a common, benign condition in most men.
If you do have any symptoms from early prostate cancer, they could include: trouble urinating, needing to urinate more often, blood in your urine or semen, and a frequent urge to urinate. You may also feel like you cannot completely empty your bladder after urinating.
If you are experiencing these symptoms, you should notify your Doctor. He will recommend prostate cancer screening, which will involve tests, including:
- PSA screening–The PSA test is a simple blood test that is carried out to detect levels of a protein known as a prostate-specific antigen. This analysis is performed to test for prostate cancer and irregularities with the prostate gland that could result in cancer later in life.
- DRE– Digital rectal exam-A doctor will insert a gloved finger up the rectum of the patient and will feel the prostate. If they detect any lymph nodes or irregularities, this could be a warning sign of cancer.
- Prostate biopsy-A prostate biopsy is a procedure used to detect prostate cancer. Small samples of the prostate are removed and then observed under the microscope.
- MRI– A multi-parametric MRI or a color Doppler ultrasound has a 95 to 98% chance of determining the location and grade of prostate cancer cells.
What is the purpose of the Gleason Score?
Named after its creator, Dr. Donald Gleason, The Gleason score is a measurement that is given to indicate the aggressiveness of prostate cancer.
Aggressiveness is a medical term used to describe the likelihood of cancer spreading outside the prostate.
The Gleason scoring system was developed at a VA hospital in the 1960s and was quickly adopted all over the world as an effective predictor of the pace of prostate cancer growth.
When he created this measurement, Dr. Gleason assigned a number between 1 and 5 to the different patterns of prostate cancer cell growth. Prostate cancer cells display different patterns of growth, which reveal their aggressiveness.
When your pathologist checks your biopsy samples, they examine your prostate cells under the microscope and will look at the different patterns.
They will then choose the two most commonly appearing patterns and give you a score. The first number indicates the most common pattern in all the samples. The second is the second most common pattern. When these two scores are added together, the total is called the Gleason score.
For more information on the Gleason Score click here.
What are the treatment options for early Prostate Cancer?
There are a number of options for treating men with prostate cancer.
Your doctor will discuss the different options with you so you can make the best decision for your body. Let’s take a closer look at some of these treatments.
Watchful waiting
Watchful waiting is usually used by men experiencing other health problems, who may be unable to handle surgery or radiotherapy.
It can be used in men with both low-risk cancer or men whose cancer has spread (advanced prostate cancer).
It involves fewer tests than active surveillance and is less intensive, more often than not taking place at the GP surgery than a hospital. If you do have treatment in the future, it will aim to control the cancer and manage any symptoms, rather than to cure it.
Active surveillance
Active surveillance includes grade group 1 or Gleason 6, a PSA level <10, cancer that is confined to the prostate (localized prostate cancer).
It can be a good option for those with slow-growing cancer who may not be able to recover from surgery or radiation quickly. If you are older, your doctor may recommend this treatment as well.
Some people find that the side effects of cancer treatments are worse than the treatment itself. In fact, one of the main benefits of monitoring low-risk cancer is that you might avoid having unnecessary surgery.
One study of men undergoing active surveillance found that, 15 years later, less than 1% of men developed metastatic disease.
Surgery
In some instances, your doctor may recommend surgery and removing your prostate gland, thereby removing all of the cancer. This surgery is called a prostatectomy and can be done with cuts in either your lower belly or in your perineum.
Laparoscopic surgery may also be an option, depending on the type of technology available at your treatment center. Robotic surgery is becoming more popular and can help control the precision of the cuts needed for this delicate surgery.
However, it is essential to note that in cases of prostate problems or even cancer, this gland is there for a purpose. Our bodies don’t have extraneous parts. Once the surgery is performed, the prostate cannot be put back.
The same sexual and urinary function of the area may never return to normal. A prostatectomy can sometimes result in nerve damage around your penis so it may affect your ability to control your bladder or get an erection. Talk to your doctor about these possible side effects before opting for surgery.
A study that compared radical prostatectomy with active surveillance drew some interesting conclusions. It found that while radical prostatectomy improved the cancer survival rate of men under the age of 65, active surveillance remained an effective management protocol for early-stage prostate cancer.
A further study supported this result, concluding that for most men ages 65 and older with localized, early-stage prostate cancer, observation might be the preferred treatment.
For more information on prostate surgery click here.
Radiation
Radiation is a form of high energy x-rays that can be produced through external beams or brachytherapy. With external beam radiation therapy, a machine focuses on x-rays on your prostate to target the cancer. Brachytherapy involves inserting small pellets of radiation into your prostate.
This usually involves either being put under or numbed so that the pellets can be placed via thin needles.
Low doses can be relatively safe, but high doses can cause long term side effects such as urinary dysfunction, bowel dysfunction, and erectile dysfunction.
Another form of radiation treatment is proton therapy. A large-scale study treated prostate cancer patients with proton therapy and found it to be an effective treatment for low-risk prostate cancer.
The cohort of 1,327 men was treated at the University of Florida Health Proton Therapy Institute between 2006 and 2010, with a median follow-up of five-and-a-half years. The researchers reported that 99%, 94%, and 74% with low, intermediate, and high-risk cancer have no signs of cancer recurrence after five years of follow up.
Nerve-sparing surgery
Radical retropubic prostatectomy most effective to preserve a man’s erectile nerves. It can substantially limit the duration of post-surgical ED but requires a surgeon to be highly skilled and trained in the process.
In this type of procedure, the surgeon takes care not to damage the erectile nerves that surround the prostate as it is removed. However, if cancer has infiltrated these nerves, it may not be possible to save them.
Preventing injury with nerve-sparing surgery significantly improves the chances of a man recovering erectile function within two years of the surgery.
Minimally invasive surgery
Minimally invasive procedures are claimed to work better than drugs in easing the symptoms of an enlarged prostate.
Prostate artery embolization is the only truly minimally invasive procedure that does not damage the prostate.
Prostate artery embolization involves inserting a catheter into an artery in the groin or wrist. Using an X-ray, it is passed into the blood vessels, and plastic particles are injected into the vessels to reduce the prostate gland’s blood supply. The aim is to shrink the prostate gland.
The UroLift system is another minimally invasive procedure. It is the first permanent implant for an enlarged prostate and works by pulling back the prostate tissue that is pressing on the urethra.
The Rezūm System uses the stored thermal energy in water vapor (steam) to treat the extra prostate tissue that is causing symptoms.
Conclusion
A prostate cancer diagnosis is concerning, but understanding it can reduce confusion. Early detection is key, and when you are fully informed about the type of cancer you have and the risks involved with each treatment, you can work with your doctor to create the best treatment plan.
If you are diagnosed with prostate cancer is very important to be open and honest with your doctor and ask lots of questions about treatments and their side effects.
Surgery is a significant decision. While sometimes necessary, it is typically chosen during moments of concern and distress.
Do your homework before diving headfirst into this life-changing decision. Remember, catching prostate cancer in its early stages is the best time.
Explore More

New Study Investigates Treatment-Associated Regrets In Prostate Cancer.
This article is for informational purposes only and does not serve as medical advice. The details provided here are not a replacement for, and should never be depended upon as, professional medical advice. Always consult your physician regarding the potential risks and benefits of any treatment.
Our Medical Review Process
At Ben’s Natural Health, we are committed to maintaining the highest standards of accuracy, transparency, and scientific integrity. Every piece of content is carefully developed by medical professionals and undergoes a thorough review every 12 to 24 months. This ensures that our information remains current, reliable, and rooted in credible, evidence-based research. We reference only peer-reviewed studies from reputable medical journals, providing full citations and direct links to enhance trust and confidence.
Our Editorial Guidelines
For over 25 years, Ben’s Natural Health has been a trusted source of scientifically backed, reliable health information. Our editorial guidelines uphold the highest quality and integrity for every article we publish. Each piece is written by qualified experts and undergoes independent quality checks. We prioritize transparency by clearly displaying contributor credentials and biographies at the beginning of every article.
Medical Disclaimer
The content on this blog is for informational purposes only and should not be considered a substitute for professional medical advice, diagnosis, or treatment. While our articles are authored and reviewed by licensed medical professionals, they may not address your specific health concerns. Always consult a qualified healthcare provider before making any medical decisions.
Article Sources
- Holmberg, L, Bill-Axelson, A, Helgesen, F, Salo,J. (2002). A Randomized Trial Comparing Radical Prostatectomy with Watchful Waiting in Early Prostate Cancer. The New England Journal of Medicine. 347 (1), p781-789.
- Osman SO, Horn S, Brady D, et al. Prostate cancer treated with brachytherapy; an exploratory study of dose-dependent biomarkers and quality of life. Radiat Oncol. 2017;12(1):53. Published 2017 Mar 14. doi:10.1186/s13014-017-0792-1
- Patel P, Young JG, Mautner V, et al. A phase I/II clinical trial in localized prostate cancer of an adenovirus expressing nitroreductase with CB1954 [correction of CB1984] [published correction appears in Mol Ther. 2009 Jul;17(7):1302]. Mol Ther. 2009;17(7):1292–1299. doi:10.1038/mt.2009.80
- Prado K, Chin AI. How nerve-sparing technique has been applied to radiotherapy?. Asian J Androl. 2016;18(6):898–899. doi:10.4103/1008-682X.184995
- https://www.health.harvard.edu/blog/early-stage-prostate-cancer-treat-or-wait-2009031010
Article Update History
Updated on 13 November, 2023 (Current Version)
Created on 30 May, 2019
Explore More

New Guidelines On Prostate Cancer Screening For Black Men
The goal of prostate cancer screening is to detect it early and find it before it spreads and causes symptoms. Late detection can lead ...

